Note: Updated May 2, 2018, to correct a link in the reference section. The error was introduced in editing.
A 44-year-old Caucasian woman presented to the outpatient rheumatology clinic that had followed her for several years for rheumatoid arthritis. She was compliant with her regimen of hydroxychloroquine, etanercept and salsalate. Her chief complaint was worsening pain in her left wrist with constant numbness and tingling and intermittent burning in the hand, particularly the first three-and-a-half fingers. Pain was worse at night. She had previously undergone successful carpal tunnel injections for this pain. She was wearing her splint nightly. Due to pain recurrence and severity, she had been recently referred to a hand surgeon for evaluation.
At this office visit, the physical examination included positive Tinel’s and Phalen’s tests on the affected side. Strength of the first digit was mildly diminished. She requested another injection to give her temporary relief while awaiting the orthopedic appointment. Using accepted topographical landmarks and targeting an area to the ulnar side of the median nerve, two attempts were made for perineural corticosteroid injection into her left carpal tunnel. The patient described severe paresthesia in her hand immediately upon needle insertion on both attempts. The procedure was terminated, and she was referred for sonographic evaluation and ultrasound-guided injection.
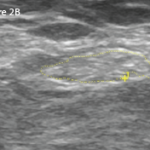
Ultrasound (US) revealed an enlarged, hypoechoic median nerve that had lost echotexture. Cross-sectional measurement of the median nerve at the wrist and forearm revealed the wrist to forearm ratio (WFR) quotient was 2.1; the median nerve had swollen to more than twice its normal size proximal to compression in the carpal tunnel. The swollen median nerve had a cross-sectional area (CSA) of 11 sq. mm.1 A notch sign, or abrupt compression of the median nerve, was noted. The US also identified significant noncompressible tenosynovitis of the flexor pollicis longus (FPL), displacing the median nerve in an ulnar direction directly in the needle path of the previous injection attempts. Power Doppler was positive surrounding the tendon. The flexor retinaculum (FR, also known as the transverse carpal ligament, or TCL) located just superficial to the median nerve had a normal sonographic appearance. (See Figure 1, for a schematic of normal carpal tunnel anatomy, and Figure 2, for this patient’s left volar wrist ultrasound, transverse view.)
An ultrasound-guided corticosteroid injection of the FPL tendon sheath on the radial aspect of the median nerve (rather than the usual ulnar side with non-US-guided injections) resulted in dramatic reduction of the tenosynovitis and marked improvement of all symptoms. The medication regimen for her rheumatoid arthritis was then changed due to the suboptimal control of the disease process as indicated by the extensive tenosynovitis. In addition, it was appreciated that with even severe active tenosynovitis, successful treatment of the median nerve compression could occur with medical rather than surgical intervention.