Jarun Ontakrai / shutterstock.com
Hepatitis B virus (HBV) associated polyarteritis nodosa (PAN) is an increasingly rare vasculitis in developed countries due to advances in HBV vaccination and antiviral therapy. However, the condition does persist, and rheumatologists should consider it when evaluating vasculitis cases.
Below, we discuss a case that illustrates the varied clinical presentations PAN can encompass. A high index of suspicion, along with a systematic workup, led to the diagnosis.
We then discuss a treatment strategy that differs from non-HBV-associated PAN.
The Case
A 53-year-old Caucasian woman with a history of chronic obstructive pulmonary disease and hypothyroidism presented to the hospital with a three-week history of stabbing pain and burning in her right leg from her shin down to her toes. She complained of an inability to plantar or dorsiflex her right foot and could not bear weight on it. She also complained of weakness, numbness and burning in her left hand occurring over the same period. She denied any rash, chest pain, shortness of breath or abdominal pain. She denied any hematemesis, hemoptysis or hematochezia. She did have a 20-year cigarette smoking history, but denied any illicit or intravenous drug use.
A computed tomography scan of her brain was unremarkable. An X-ray of her right foot and left hand was normal, and non-contrast magnetic resonance imaging (MRI) of her thoracic and lumbar spine revealed no central canal stenosis or neuroforaminal narrowing.
The patient’s vital signs were stable. The physical exam was notable for normal muscle strength in her right, upper extremity and left, lower extremity. However, with her left hand, the patient had difficulty closing her thumb, index and middle finger due to pain and weakness. She had significant hyperalgesia to even light touch to her right lateral shin, ankle and foot. She had a right foot drop. A gait exam was deferred. She did not have any rash, and the rest of the physical exam was normal.
Mononeuritis multiplex was suspected, and she was started on 1 g daily methylprednisolone intravenously for three days while the workup was underway. Magnetic resonance imaging and angiogram of her brain showed patent cerebral vessels and no evidence of stroke. Significant lab results appear in Table 1.
Given the positive HBV serologies, elevated inflammatory markers and mononeuritis multiplex, we suspected PAN. The HBV viral load was extremely high at 548 million IU/mL.
Interestingly, an abdominal aortogram and bilateral, lower extremity arteriogram did not show any abnormalities in her abdominal or renal vessels. The bilateral, lower extremity arteriogram demonstrated normal flow down to her ankles. Distal arch occlusive disease was noted, but with no acute cutoff to suggest vasculitis, and the changes were consistent with her longstanding smoking.
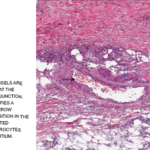
Given the non-diagnostic arteriogram and continued suspicion for polyarteritis nodosa, the decision was made to pursue a right sural nerve biopsy. The sural nerve biopsy did show vasculitis on pathology (see Figures 1, 2 & 3).