Rheumatoid arthritis (RA) is a chronic, systemic, autoimmune disease with potential for multisystem involvement that promotes inflammation. Chronic inflammation of the synovial tissue results in stiffness, pain, warmth and swelling of joints. Untreated, it can lead to joint erosions and deformity resulting in disability and decreased quality of life (QOL). Both genetic and environmental factors have been implicated. Prevalence is estimated to be between 0.5 and 1.0% in the general population. Almost three times as many women as men have RA, with the highest incidence in middle age.1
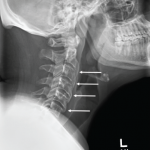
Osteoarthritis (OA) is primarily the result of mechanical wear over time, leading to the loss of cartilage between the joints. It is the most common form of arthritis, affecting an estimated 12.1% of the U.S. population ages 25 and older. The prevalence of OA increases with age.2 Degenerative disk disease (DDD) is caused by daily stress on the spine and aging, which can be exacerbated by unnoticed major or minor injuries. Early changes of DDD can be apparent on radiographs in otherwise healthy adults between the ages of 30 and 50 years old, the majority of whom will be asymptomatic.3
Case Report
A 63-year-old woman with a 23-year history of RA presented with concern about her best treatment options. Due to multiple family relocations, she had seven previous rheumatologists. Her pharmacologic treatment over the years had included hydroxychloroquine, gold injections and, at one time, monotherapy with methotrexate (MTX). In 2002, infliximab was added to MTX, but efficacy waned, and she was switched to etanercept in 2008. Her major concern was fear of infection because she had recently experienced acute diverticulitis complicated by sepsis from a perforated bowel, requiring colostomy while she was taking combination therapy with MTX and etanercept. Both immunosuppressive agents were discontinued. After six-and-a-half months, she had a successful laparoscopic colostomy takedown.
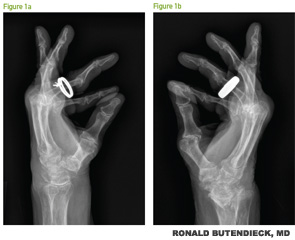
At the time of her visit, she was taking hydroxychloroquine 200 mg twice daily, as well as prednisone. Clinical evaluation demonstrated active bilateral polyarticular synovitis, flexion contractures and elevated inflammatory markers. Radiographs of the bilateral hands demonstrated changes consistent with severe, erosive, chronic rheumatoid arthritis (see Figures 1a and b, p. 50). Her prednisone was weaned off over the next six months, but secondary to persistent, active RA with elevated inflammatory markers, she agreed to start abatacept. At subsequent visits, progressive improvement was observed, and at six months, she achieved clinical remission.