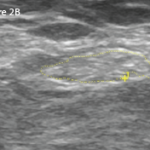
Using quantitative magnetic resonance imaging (MRI), researchers have shown in a small clinical trial that chondroitin sulphate (CS) treatment significantly reduces the cartilage volume loss in knee osteoarthritis (OA) starting at six months of treatment, and subchondral bone marrow lesions (BML) at 12 months.1
Published in the Annals of the Rheumatic Diseases, the pilot multicenter randomized, controlled, double-blind trial studied 69 patients with clinical signs of synovitis. Compared with those in the placebo group, patients in the CS group experienced a reduction in cartilage volume loss in the global knee at six months (p=0.030) that persisted at 12 months (p=0.021), a similar reduction at both six and 12 months in the lateral compartment (p=0.015 and p=0.004, respectively), and the tibial plateaus (p=0.002 and p=0.017, respectively). Reductions were also noted at six and 12 months in the lateral and medial tibial plateau, as well as the lateral condyle. The BML data showed no difference between the two groups at six months, but at 12 months there was a trend favoring the CS group (p=0.062 for the global knee, p=0.035 for the lateral compartment, and p=0.044 for the lateral condyle).
These results were in contrast to a controversial network meta-analysis published in the British Medical Journal (BMJ).2 In that study, Wandel et al used a Bayesian model to make direct comparisons of the treatment effects of glucosamine, chondroitin, or their combination with placebo or head to head, within randomized controlled trials in more than 200 patients with osteoarthritis of the knee or hip. The researchers concluded that, “compared with placebo, glucosamine, chondroitin, and their combination do not reduce joint pain or have an impact on narrowing of joint space.” They further opined that “health authorities and health insurers should not cover the costs of these preparations, and new prescriptions to patients who have not received treatment should be discouraged.”
Critical Eye on the Research
Several criticisms of the BMJ study were reported on the journal’s website in subsequent months, including remarks from Jean-Pierre Pelletier, MD, professor of medicine at the University of Montreal and senior author of the new study in the Annals of the Rheumatic Diseases.
“The BMJ article is a meta-analysis (in) which we disagree with the opinion of the principal investigators,” Dr. Pelletier tells The Rheumatologist. “Our opinion is not different from the one expressed by the BMJ deputy editor,” he says, referring readers to the BMJ website for rapid responses to the BMJ article. “The study published by our group in Annals of the Rheumatic Diseases is well in line and supports previous publications on DMOAD [disease-modifying OA drug] effects of CS,” he adds.