
Since the mid 2000s, unprecedented changes in healthcare coverage have been looming over both payers and providers. With this influx of changes and strict regulations on such areas as quality, transparency, and compliance, the strain and cost of dealing with prior authorization and delayed processing of claims has pushed providers to their limit.
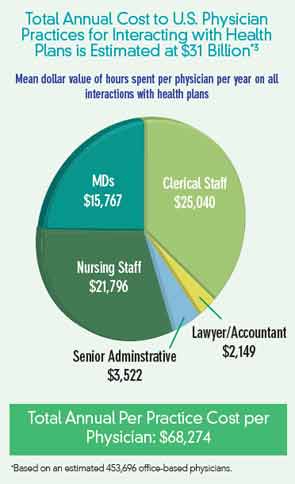
Claims processing and prior authorization of physician claims have become a costly administrative burden for most medical practices nationwide. In 2009, researchers with the Commonwealth Fund reported that the administrative cost of dealing with these claims in the United States totaled an estimated $156 billion in 2007, and they project it to reach $315 billion by 2018.1
The claims-management revenue cycle consumes an unsustainable 10%–14% of a practice’s income.2 A sizeable portion of these rising costs can be attributed to money spent having staff monitor the continuous processing of undue insurance-related activities such as validating insurance coverage, obtaining prior authorization for procedures and lab tests, appealing denials and underpayments, and reconciling unpaid claims.
The system continues to become more expensive and wasteful, and the manual processes in place for interacting with insurers may contribute to the problem. The ACR’s practice management department is collaborating with insurers to create a more automated, transparent, and real-time method of handling claims transactions, which should represent substantial progress in streamlining the process. To automate processes and reduce costs, the system should:
- Employ a standardized process that applies to all payers;
- Insert a regular, programmed workflow into the payer and physician-practice systems;
- Eliminate manual transactions between payers and providers; and
- Standardize payer and provider interaction processes and regulations.
To accomplish these goals, we must identify the portion of expenditures that go to administrative burdens that can be reduced by increasing the efficiency of the billing and insurance verification system. This also highlights the need for administrative simplicity and harmony. There are multiple stakeholders involved in the system, and there is value in broadening the scope of our collaboration to improve the system.
Overview of the Cost
On June 17, the American Medical Association (AMA) released the 2013 AMA National Health Insurer Report Card, its annual report on health insurers, including their patterns for processing and paying medical claims. The report concluded that administrative tasks associated with avoidable errors, inefficiency, and waste in the medical claims process resulted in an average cost of $2.36 per claim for physicians and insurers. Visit www.ama-assn.org/go/reportcard to access the report’s results.

