sdecoret/shutterstock.com
WASHINGTON, D.C.—In 2017, rheumatologists will begin to track and report quality data for reimbursement under the the Medicare and CHIP Reauthorization Act of 2015 (MACRA). Panelists shared their tips on how to score more points under MACRA and utilize existing technology at a Nov. 14 session called Implementing Quality Measurement in Your Clinical Practice at the 2016 ACR/ARHP Annual Meeting.
MACRA’s chief goal is to improve quality of care while decreasing healthcare costs, said Jinoos Yazdany, MD, MPH, associate professor of medicine at the University of California, San Francisco.
“This legislation had bipartisan support, so unlike the Affordable Care Act, MACRA may be here to stay,” she said. “The high-priority goals are patient-centered care, population health management, for practices to engage in continuous feedback and improvement, and to be able to demonstrate that you’re doing all of that.”
Most rheumatology practices will choose the MIPS (Merit-Based Incentive Payment System) track in MACRA for the first few years, said Dr. Yazdany. Under the MIPS option, providers must track and report on quality measures to the Centers for Medicare and Medicaid Services (CMS) in four domains: Quality Improvement Measures, Advancing Care Information, Clinical Practice Improvement Activities, and Quality and Resource Utilization Reporting, or cost.
Participation in MIPS can be done as an individual or a group, she said. Each measure earns points that make up a provider’s annual score, and each score will be compared on a decile scale to determine either a negative or positive payment adjustment for that participant in 2017. Based on feedback from physicians, The CMS has also included a “pick your pace” option for 2017, where rheumatologists can avoid payment penalties by reporting on just one measure.
Document to Earn Points
In the first year, the score will consist of 60% Quality Improvement Measures, 25% Advancing Care Information and 15% Clinical Practice Improvement Activities. Quality and Resource Utilization Reporting, or costs, won’t have an impact on quality scores in first year, but will rise to 10% by 2018, said Alex Limanni, MD, a rheumatologist at Arthritis Centers of Texas in Dallas. CMS made this change due to uncertainty about how costs for a particular patient should be attributed among different providers, he said.
In the first year, participants in MIPS will have to report only on a single measure to avoid a negative adjustment, the panelists stressed. In MIPS, there are 90 Clinical Practice Improvement Activities to select and report on, including “subcategories [that] center on concepts of extended patient access, population management, care coordination, beneficiary management, patient safety and practice assessment,” said Dr. Limanni.
“One of the measures is improved access to care, or 24/7 access to clinicians for urgent or emerging care. That could be expanded hours, phone visits or same-day appointments. This is something we talk about doing all the time in rheumatology. Documenting these activities will be useful for you,” he said. Telehealth also earns MIPS points, but many rheumatologists are still unsure how to incorporate this technology into clinical care, he said.
Use the ACR’s RISE Registry
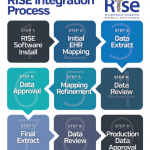
Using a qualified clinical data registry (QCDR) such as the ACR’s Rheumatology Informatics System for Effectiveness (RISE) Registry, earns points in MIPS. RISE is free for ACR and ARHP members. It passively extracts data from a practice’s electronic health record (EHR) and reports it directly to the CMS, said Dr. Limanni.
RISE helps users score points for another MIPS measure: assessing local practice patterns and improving care for vulnerable populations. “Use your registry functions and your EHR to look for local patients with specific diseases or in specific demographics, and then come up with an action plan to deal with them,” he said. Beneficiary engagement also earns points and can be done with RISE.
The ACR offers free technology support to help rheumatologists connect to RISE, said Dr. Yazdany. These consultants can tailor the registry to suit each practice’s workflow or EHR system. Practices that use an EHR with cloud-based data storage or those in large networks with IT security firewalls have had issues connecting to RISE, but the ACR is committed to lowering those barriers to more rheumatologists using the registry, said Dr. Yazdany.
Episodes of Care
Cost-Focused Quality Resource and Utilization Reporting, or QRUR, will begin to affect MIPS scores in the second reporting year. These reports will compare providers’ costs and treatment quality according to national benchmarks. They will track episodes of care or all clinical services for specific diagnoses triggered by the entry of an ICD-10 code, said Dr. Limanni. The ACR is working with the CMS to create rheumatology-specific episodes of care definitions, especially for RA and lupus.
“We don’t know what the duration of the episode is in rheumatology. As a rheumatologist, I think, rheumatoid arthritis is forever. Are they going to track my patient forever and all the costs associated with my patient forever? That’s yet to be decided,” said Dr. Limanni.
MIPS: Impact on Payments
MACRA is budget neutral and competitive by design, said Dr. Yazdany. Each year, a quality score threshold will determine whether providers receive negative or positive reimbursement.
“It’s very important for our community of physicians to make sure they are staying on top of this,” she said. The CMS made the positive payment threshold easy to attain in the first year. Participants will have to report only on a single quality measure to avoid a 4% negative adjustment. “Think of a treadmill. It will only move faster and faster. So get on at the beginning when the penalties are smaller, and be well positioned to get better incentive payments as we move along.”
The ACR will focus on building more quality measures included in the Clinical Practice Improvement Activities domain of MIPS into RISE to make reporting easier and more meaningful for members, said Dr. Yazdany.
In the first year, participants in MIPS will have to report only on a single measure to avoid a negative adjustment.
“MIPS will get less lenient as time goes on, but just by participating in some way, rheumatologists should be OK. No rheumatologist should face a penalty if they report even a single measure in 2017,” she said. “What’s nice about using RISE is that it includes specific measures that are relevant to rheumatology practices and the registry will adapt to streamline and simplify quality reporting over time.”
By using RISE, a practice can also review and compare their current quality scores on a data dashboard: green indicates a user is above the registry mean, yellow indicates at the mean, and red warns a practice is below the mean. All analytics are provided as a benefit of using RISE.
Relevant Measures
Catalina Orozco, MD, a rheumatologist in Dallas, and Brian Loggins, PA, a rheumatology practice manager in San Antonio, offered the following information and tips:
- Involve a clinician in initial set-up. RISE offers technology consultants to connect practices to the registry, but a clinician will help tailor the interface to your practice’s workflow and ensure more accurate data mapping.
- Track specific measures. The ACR’s quality subcommittee is working on developing quality measures in RISE that are relevant to rheumatology practices. Currently, measures for RA, gout and glucocorticoid-induced osteoporosis are incorporated into RISE.
- Record patient encounter information in structured data fields. This will help RISE track your quality measures more effectively, said Dr. Orozco. Users can also resubmit data if RISE does not capture or transfer it properly.
Note: Cloud-based issues are being fixed. Rheumatology practices that used cloud-based EHRs had problems using RISE in the past, but the Registry has updated technology that is tackling this problem, Dr. Yazdany said.
Susan Bernstein is a freelance medical journalist based in Atlanta.