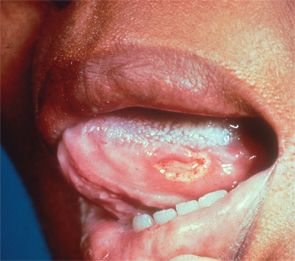
A large, deep, painful ulceration is present on the lateral margin of the tongue in this patient with Behçet’s syndrome.
ACR IMAGE BANK
SAN FRANCISCO—Behçet’s disease is a vasculitis that can be hard to pin down, with a wide variety of manifestations, many of which overlap with other auto-inflammatory conditions, an expert said at a clinical review course at the 2015 ACR/ARHP Annual Meeting.
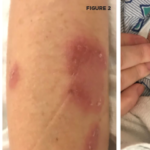
The most common feature is oral ulcers, which are expected to be seen at some point in the course of the disease, but patients can present with skin lesions, arthritis, amyloidosis, uveitis and joint problems, said Seza Ozen, MD, professor of pediatrics at Hacettepe University in Turkey.
The issues that arise from the disease can often seem unrelated. Complicating matters, it’s characterized by flares and remissions that can simply come and go on their own.
“The diagnosis is sometimes quite challenging,” Dr. Ozen said.
In fact, she said, therapies have been little studied—with very few evidence-based treatments—in part because of the disease variations that are seen, she said.
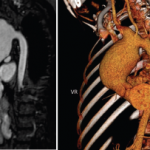
“Some patients tend to present with some skin lesions only,” Dr. Ozen said, while “some tend to present with severe eye disease as the prominent feature, and some can present with more vascular features.”
Prevalence
Prevalence varies widely, as well. In Turkey and Japan, Behçet’s occurs in more than 1 per 1,000 people. Mayo Clinic estimates prevalence in the U.S.-based population to be 5.2 per 100,000, Dr. Ozen said.
And there appears to be a genetic link to the disease. A study out of France found the North African and Asian subpopulations there had a prevalence of 34.6 and 17.5 per 100,000—about the same as the prevalence found in the native countries of those ethnicities, suggesting genetics is in play more than environmental factors, Dr. Ozen said.
Genetics
Two genome-wide association studies in 2010 found that susceptibility links between Behçet’s and the IL10 and IL23R genes. In one of the studies, the presence of the HLA B51 gene, known to be a risk factor for the disease, seemed to depend on the presence of the gene ERAP1.1,2
Dr. Ozen said it’s theorized that ERAP1, which provides instructions for making proteins, may cause problems with protein folding, including the misfolding of HLA B51, leading to activation of IL23 and IL17, which then join together in an inflammatory response.
She noted similarities to ankylosing spondylitis: uveitis, arthritis and gastrointestinal issues, and the association with an HLA and IL17.