WASHINGTON, D.C.—The first treatment option for most kinds of scleroderma bowel disease, or gastrointestinal involvement related to scleroderma, is lifestyle change—but proven medical treatments are hard to come by and are severely understudied in this disorder, an expert said at the 2012 ACR/ARHP Annual Meeting, held here November 9–14. [Editor’s Note: This session was recorded and is available via ACR SessionSelect at www.rheumatology.org.]
Most of the medical treatments do not come with a long track record, said John Clarke, MD, clinical director of the Center for Neurogastroenterology at Johns Hopkins University in Baltimore, in a session titled, “Scleroderma Bowel Disease: From Top to Bottom.”
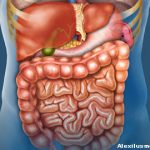
Scleroderma is a systemic process, and the gastrointestinal (GI) tract is the largest organ system in the body except for the skin, so it shouldn’t be surprising that GI involvement is the most frequent internal complication. The esophagus is the most commonly affected organ, but any part of the GI system can be involved, with symptoms from dysphagia to heartburn, vomiting to incontinence. And the complications can be very serious. Severe GI involvement is seen in only about 8% of cases, but among those, only 15% survive more than nine years, Dr. Clarke said.
“Scleroderma does affect the gut within the vast majority of cases,” Dr. Clarke said. “Treatment is geared primarily toward decreasing reflux, reducing the complications associated with it, enhancing gastrointestinal function, avoiding bacterial overgrowth, and optimizing nutrition. Treatments at this point are mainly reactive in nature.” He offered treatment guidance for a variety of symptoms and conditions related to scleroderma bowel disease:
Oropharyngeal
Treatment is limited to lifestyle changes—small bolus sizes, soft foods, liquid supplementation, and dental follow-up.
Esophageal Dysmotility
“Treatment can be somewhat challenging,” Dr. Clarke said. “The scleroderma-specific therapies haven’t been shown to make a difference in terms of gastrointestinal dysfunction. The goal of treatment is certainly to reduce symptoms as well as treat any complications that arise.”
Patients should avoid foods known to slow gastric emptying or decrease sphincter pressure, such as chocolate, high-citrus fruits and juices, onions, garlic, and caffeine. Quitting smoking, avoiding alcohol, elevating the head when sleeping, sleeping on the left side, and not eating within three hours of sleeping are also recommended.
Medically, proton-pump inhibitors are the mainstay, “by far the most effective, but also the most expensive,” Dr. Clarke said. Prokinetics are not great options, but the EULAR Scleroderma Trials and Research (EUSTAR) consensus in 2009 recommended considering them, he said.1