
Pressmaster/shutterstock.com
WASHINGTON, D.C.—The importance of biomedical research to advancing clinical care with the ultimate goal of improving patients’ lives was on display during an ACR Discovery 2016 plenary session at the 2016 ACR/ARHP Annual Meeting.
The session offered new ways to think about and treat select rheumatologic diseases, including research showing for the first time the efficacy of a steroid-sparing medication for giant cell arteritis (GCA), research suggesting that statins may lower mortality risk in patients with ankylosing spondylitis (AS) or psoriatic arthritis (PsA) and research showing the importance of normalizing uric acid levels to improve renal function in patients with chronic kidney disease (CKD).
Steroid-Sparing Medication for GCA
“The era of unending glucocorticoid treatment with no viable alternative is over,” said John H. Stone, MD, MPH, director of clinical rheumatology and the Edward A. Fox Chair in Medicine at the Massachusetts General Hospital, who presented the findings of the GiACTA trial.
The GiACTA trial, the largest trial ever conducted of patients with GCA, enrolled 251 patients from 14 countries and 76 sites for 22 months to evaluate the efficacy and safety of tocilizumab for patients with GCA. Dr. Stone said that GiACTA is also the first trial for any disease to employ a blinded, variable-dose, steroid-tapering regimen.
The trial compared the efficacy of four different treatment arms for patients with GCA: 26-week prednisone taper (PBO + 26; n=50), 52-week prednisone taper (PBO + 52; n=50), tocilizumab 162 mg once weekly + PBO + 26 (TCZ QW; n=100), and tocilizumab 162 mg once every two weeks + PBO + 26 (TCZ Q2W; n=50).
At 52 weeks, the study showed significantly greater sustained remission in patients treated with tocilizumab compared with prednisone (see Table ).
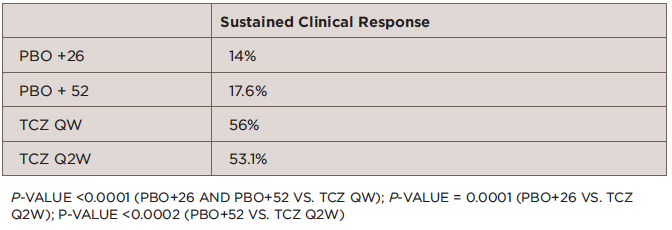
TABLE 1: Primary Outcome: Sustained Remission from Week 12 to Week 52
The most surprising finding of the study, according to Dr. Stone, was the poor results in the patients treated with prednisone only. “I think most rheumatologists will find it surprising that the therapy we have regarded as the standard of care—that has been the standard of care for many decades—fared so poorly,” he said.
Along with the significant benefit to adding tocilizumab, the study found no significant differences in adverse events among the treatment arms. “In fact, patients in the steroid-only groups were more likely to experience more than one serious adverse event than were those in the tocilizumab groups,” he said, adding that this “underscores the major contribution of glucocorticoids to toxicity in this disease.”
Based on these findings, Dr. Stone emphasized that an effective steroid-sparing medication for GCA is now available for the first time in 67 years “since the invention of cortisone in 1949. … This is a great achievement for rheumatology and for patients with GCA,” he said.
Although both dosing schedules of tocilizumab showed significant benefit compared with prednisone alone, Dr. Stone speculated that most clinicians would choose to use the once-weekly dosing because of the critical need to quickly and completely shut down inflammation from GCA to avoid irreversible damage, such as vision loss and complications of large-vessel vasculitis.
Dr. Stone also highlighted the need for a paradigm shift in how clinicians think about GCA. “In addition to beginning steroids promptly when this diagnosis is suspected, we also need to begin treatment with tocilizumab once the diagnosis is confirmed,” he said. “Failure to exert and maintain disease control only leads to increasing steroid toxicity over time and places patients at risk for serious complications of GCA.”
‘I think most rheumatologists will find it surprising that the therapy we have regarded as the standard of care [prednisone only]—that has been the standard of care for many decades—fared so poorly.’ —Dr. Stone
Survival Benefit with Statins
Amar Oza, MD, clinical fellow, Department of Rheumatology, Massachusetts General Hospital, presented data from a population-based cohort showing a survival benefit of statins in patients with PsA and AS.
Data from The Health Improvement Network (a United Kingdom population database) were used to identify patients with PsA and AS between January 2000 and December 2014. Investigators quantified the all-cause mortality reduction in patients initiated on statins compared to propensity-matched patients not initiated on statins.
The study found that statin initiation was associated with a 32% reduction in all-cause mortality, with a hazard ratio of 0.68 (95% CI, 0.57–0.81). Along with suggesting that statins may be beneficial in lowering the risk of all-cause mortality in patients with AS and PsA, Dr. Oza said the results suggest that “the magnitude of this mortality reduction is larger than large meta-analyses of the general population, on the order of 9–14%.”
Dr. Oza said that a future study will look at biologic treatment and adherence, because the current study did not include these medications.
Lowering Uric Acid Improves Chronic Kidney Disease
Gerald D. Levy, MD, rheumatologist, Kaiser Permanente, Downey, Calif., presented data from a large retrospective cohort of patients with hyperuricemia that showed that lowering uric acid (UA) levels to below 6 mg/dL improved both hyperuricemia and chronic kidney disease (CKD).
According to Dr. Levy, these benefits were seen in 6% of patients who achieved the targeted UA goal compared with patients who did not achieve this goal.
The study also found that CKD stage was an important factor in which patients improved after UA lowering therapy, with 3% of patients with stage II CKD improving and nearly 10% of patients with stage III CKD stage improving. The study found no benefit in patients with stage IV CKD.
These results, emphasized Dr. Levy, indicate the need to monitor patients with hyperuricemia and CKD. “Consider utilizing urate-lowering therapy in addition to the usual ‘tools’ of optimizing glucose and blood pressure control,” he said, “along with ACE and ARBs to stabilize and possibly improve renal function.”
Dr. Levy also pointed out the need for rheumatologists to better educate primary care physicians on the need to assess and monitor uric acid levels not only for diagnosing and treating gout, but also for the connection between high uric acid levels and renal disease. “Numerous studies show that primary care physicians under-diagnose and under-treat this generally, easily controlled disease,” he said. “This led to unnecessary pain and lost function by millions of patients.”
Saying that the current guidelines on uric acid give mixed messages and focus largely on gout, he emphasized that published data show the importance of normalizing uric acid for CKD benefit (current study) as well as for cardiac and cerebral benefits. “To focus only on the aspect of acute gout attacks is likely to lead to more [emergency department] visits, with the associated costs, lost work and wages, and patients who ultimately develop renal, cardiac and cerebral problems that could be avoided simply by using a well-tolerated relatively inexpensive medication,” he said.

