Though I have labored in the rheumatologic vineyards as a clinician for more than 35 years, the details of my first cases of polymyalgia rheumatica (PMR) and giant cell arteritis (GCA) are still fresh. The former brought a bottle of holiday cheer, with gratitude for the triumphant effects of low-dose prednisone on aching and stiffness of nearly disabling extent; the latter, nothing but heartache. On three occasions during the preceding month, the patient with GCA had hunted medical care for symptoms of anorexia, low-grade fevers, and occipital headaches, twice from her general practitioner and once from a local emergency room. When I first met her, she had just been hospitalized, having lost vision in the left eye the previous day. Now she was admitted to hospital with amaurosis fugax affecting the right eye, which, despite the use of high-dose corticosteroids, ended in permanent loss of sight in that eye as well. Since that first year of fellowship, both diseases remain at the core of my clinical interests, and a potential referral for either still quickens the clinical pulse.
PMR and GCA: Relatedness, Including Misnomers
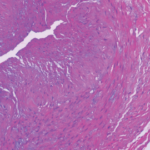
The kinship of PMR and GCA is well known. PMR is found in up to one-half of patients with GCA (though the two need not occur synchronously). GCA is commonly cited as affecting 15% of patients with PMR, though in clinical practice that percentage is probably somewhat lower. Both are quintessential conditions of older adults—in effect, never occurring under the age of 50, with 90% of cases over the age of 60, and a median age of onset in the 70s. The clinical and epidemiologic connections carry down to the immunologic level, as the temporal arteries from patients with PMR and GCA both contain activated dendritic cells and similar cytokine profiles—with the notable exception of interferon-γ (IFN-γ), which is present in the temporal arteries of patients with GCA but absent in PMR, and which likely plays a pivotal role in the transformation from a vasculitis that is subclinical to one that is clinically explicit.1
PMR and GCA share another similarity: both are misnomers.
“Polymyalgia rheumatica” was coined by Barber in an article dating from 1957, and has remained embedded in the literature since then.2 But as Andy Healey, MD, emeritus clinical professor of medicine at the University of Washington in Seattle, suggested in the 1980s, and as expanded on by Carlo Salvarani, MD, director of rheumatology at Arcispedale Santa Maria Nuova in Reggio Emilia, Italy, and Gene Hunder, MD, emeritus professor of medicine at the Mayo Clinic in Rochester, Minn., and others, PMR, in fact, prominently affects the synovium of the joints and bursae, not the muscles.3,4 The designation “polymyalgia rheumatica” implies a myopathic process, and, I believe, tends to hinder and delay consideration of its correct diagnosis among nonrheumatologists. “Axial presbyarthritis” is more anatomically correct, but doesn’t have a particularly euphonious ring, and so I rather doubt it will supplant the more venerable “polymyalgia rheumatica.”