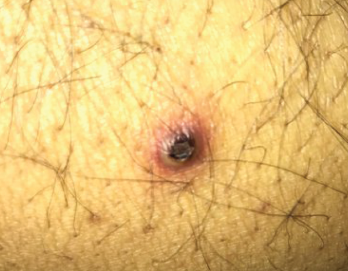
Figure 1. The patient had nodular pus-filled cystic lesions with violaceous borders on his left ear, right cheek, fingers and legs.
A 42-year-old man with a history of ulcerative colitis (UC), primary sclerosing cholangitis (PSC) and chronic sinusitis was referred to a rheumatologist to evaluate for a possible diagnosis of systemic vasculitis. This patient had developed new skin lesions, gingival hypertrophy and ulcerating tracheobronchitis, concerning for possible granulomatosis with polyangiitis (GPA).
Since 1994, the patient had sinusitis with occasional bloody discharge and nasal turbinate hypertrophy demonstrated on imaging. He was followed by an otolaryngologist, and his symptoms were well controlled with budesonide nasal rinses. In 1996, the patient presented to the hospital with abdominal pain and bloody diarrhea. A subsequent colonoscopy and biopsy confirmed a diagnosis of UC. He was treated with mesalazine, and in 1998, when he developed PSC, ursodiol was added.
Overall, his UC was well controlled until 2012. At that time, he began requiring intermittent steroids for UC flares, and in 2015, his gastroenterologist started treatment with vedolizumab.
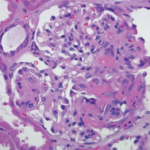
In late 2016, the patient developed nodular, pus-filled cystic lesions with violaceous borders on his left ear, right cheek, fingers and legs (see Figure 1). Biopsy of these cutaneous manifestations were suggestive of neutrophilic folliculitis, a variant of pyoderma gangrenosum.1
Around the same time, the patient also started having severely painful, bleeding gingival hypertrophy (see Figure 2). Based on the appearance of his gums, this symptom was thought to be strawberry gingivitis, a rare, but classic, feature of GPA.2 Consequently, the possibility of an overlapping vasculitis concurrently occurring with the patient’s inflammatory bowel disease (GPA-IBD overlap) was suggested. As a result, azathioprine and prednisone were added to the patient’s medication regimen.
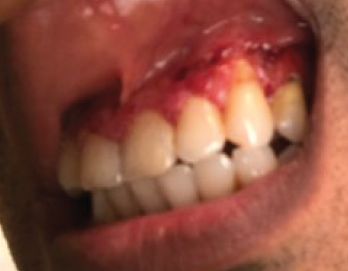
Figure 2. The patient presented with severe, painful, bleeding gingival hypertrophy.
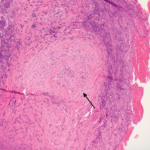
After review with multiple specialists, gingival biopsies in January 2017 demonstrated pyostomatitis vegetans, which is a known extra-intestinal manifestation of IBD.
Sinus biopsies were also performed and did not show any evidence of vasculitis. Further, serologic evaluation during this period of diagnostic inquiry was variable. In March 2016, the patient was positive for C-ANCA (anti-neutrophilic cytoplasmic antibodies), but was PR3-ANCA and MPO-ANCA negative. In February 2017, he had an atypical P-ANCA (perinuclear ANCA) with a PR3-ANCA of 49.6 (normal <20). In March 2017, all ANCA serologies were negative.
Over the next eight months, the patient was treated with increasing doses of azathioprine and prednisone, up to 150 mg once daily and 50 mg once daily, respectively. But his pyostomatis vegetans failed to respond, and he continued to have significantly distressing gum pain and bleeding.
In September 2017, in an attempt to control this symptom, he was switched from vedolizumab to infliximab. This change initially improved his gingival manifestations after the first dose; however, subsequent doses, including dose escalations, did not achieve the same therapeutic effect. Additionally, his previously well-controlled gastrointestinal symptoms flared, and the decision was made to switch him back to vedolizumab.
In March 2018, the patient was admitted to the hospital with decompensated liver cirrhosis and an acute portal vein thrombosis. He underwent liver transplant and was discharged home.