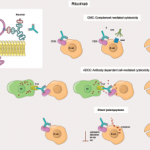
Patients with antineutrophil cytoplasmic antibody–associated vasculitis (AAV), including granulomatosis with polyangiitis (GPA) and microscopic polyangiitis (MPA), are often prescribed high doses of glucocorticoids and immunosuppressive medication, such as rituximab. Glucocorticoid treatment is commonly associated with weight gain. Despite the well-established link between glucocorticoid use and cardiovascular risk, weight gain is not always an adverse event due to the risks of weight loss associated with increased catabolic activity experienced by patients with these inflammatory conditions.
“The ability to classify increased BMI [body mass index] (e.g., weight gain) accurately as either an adverse event related to glucocorticoid exposure or a positive outcome reflecting improved disease activity is, therefore, important in studies investigating glucocorticoid-sparing strategies,” write Zachary S. Wallace, MD, and colleagues from Massachusetts General Hospital in Boston in their latest research, published in the July 2017 issue of Arthritis Care & Research.
Only one previous study, the Wegener’s Granulomatosis Etanercept Trial, has examined the relationship between AAV treatment and changes to patient BMI. It found weight gain was not associated with glucocorticoid exposure. In their latest research, Dr. Wallace and colleagues set out to replicate these findings, as well as investigate the relationship between increases in BMI and improved disease control.
The researchers used data from the Rituximab in ANCA-Associated Vasculitis (RAVE) trial, which included 197 participants with antineutrophil cytoplasmic antibody positivity with GPA or MPA and severe disease. In the RAVE trial, patients were randomized into two groups: one treated with cyclophosphamide and one with rituximab. Both groups received the same glucocorticoid protocol. Throughout the trial, glucocorticoid use, BMI and disease activity were measured regularly between baseline and 18 months.
The Results
Researchers successfully replicated the original clinical study, finding that increases in BMI are multifactorial and associated with improvements in disease activity, cumulative glucocorticoid exposure and randomization to rituximab. The study also demonstrated that “when a more granular analysis is conducted, changes in BMI during induction treatment do in fact have complex associations with glucocorticoid exposure, disease activity and randomization to rituximab,” write the authors.
The most significant increase in BMI occurred during the first six months. The mean BMI (plus or minus the standard deviation [SD]) increased by 1.1 ± 2.2 kg/m2 (P<0.001 compared with baseline). At 12 and 18 months, BMI did not significantly change. When the researchers applied the same methodologies as the original trial, conducted a multivariate linear regression analysis and adjusted for potential confounders, they found no significant association between the quantity of glucocorticoids administered and change in BMI.
The authors note, “One of the strongest predictors of BMI change at six, 12 and 18 months that emerged from this analysis concerned whether the patient had a new diagnosis of AAV or was relapsing at baseline.” Patients newly diagnosed with AAV had an increased mean BMI (± SD) of 0.8 ± 0.3 kg/m2 (P=0.008) compared with patients with relapsing disease. Randomization to rituximab also emerged as a predictor of BMI change at Months 6 and 12. Rituximab-treated patients showed a mean (± SD) increase in BMI at Month 6 of 0.9 ± 0.3 kg/m2 compared with patients randomized to cyclophosphamide (P=0.002).
Researchers were further able to determine that the change in BMI during the first six months of the RAVE trial were associated with disease activity, as reflected by BVAS/WG score, ESR and CRP level.
“In some circumstances, it seems likely that the occurrence of weight gain implies effective disease control,” write the authors in their discussion. “In contrast, the failure of a patient on glucocorticoid treatment to gain weight augurs poorly for long-term disease control. In the absence of effective disease control, the weight loss associated with active disease trumps even glucocorticoid treatment. … It is only when the inflammation associated with AAV has been controlled that the full impact of glucocorticoid treatment on weight gain is realized.”
Although the factors that contribute to weight gain are complex and may be influenced by additional factors, the authors conclude that understanding the “factors mediating the relationship between glucocorticoid exposure and BMI variation is crucial to identifying and defining the significance and potential hazards of weight gain in the treatment of inflammatory conditions.”
Wallace ZS, Miloslavsky EM, Cascino M, et al. Disease activity, glucocorticoid exposure, and rituximab determine body composition changes during induction treatment of ANCA-associated vasculitis. Arthritis Care Res (Hoboken). 2017 Jul;69(7):1004–1010.