- b. If a ZPIC auditor shows up at a practice and requests to see medical records and the practice chooses not to comply, the auditor will contact the carrier and immediately suspend the provider’s NPI number until the request is complied with.
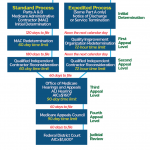
- Redetermination. Although the provider has 120 calendar days to submit a request in writing, an automatic recoupment will begin on Day 41 if an appeal is not requested within 30 days of the date of the demand letter.Reconsideration. Providers not in agreement with a carrier’s redetermination decision may file for reconsideration to be conducted by a Qualified Independent Contractor (QIC). This level of appeal must be filed within 180 calendar days of receiving notice of the redetermination decision from the carrier.
Administrative Law Judge (ALJ) Hearing. A provider who is dissatisfied with a reconsideration decision or chooses to exercise the escalation provision at the reconsideration stage may request an ALJ hearing. The request must be filed within 60 days of receipt of the QIC’s decision. There must be at least $130 in dispute.
Medicare Appeals Council (MAC) Review. A MAC review request must be filed within 60 calendar days of receipt of the ALJ’s decision. The MAC review must classify and explain the parts of the ALJ action the provider disagrees with. There must be at least $130 in dispute.
Federal District Court. This is the final step in the appeals process. A request for a review in the district court must be filed within 60 calendar days of receipt of the MAC’s decision. The disputed amount must be at least $1,260.