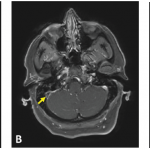
An angiogram was unrevealing. NMDA and other anti-neuronal antibody testing was also negative.
The girl was close to meeting the criteria for autoantibody-negative but probable autoimmune encephalitis, but the “exclusion of alternative diagnoses” requirement “gives us pause,” Dr. Van Mater said. Clinicians remained concerned about a post-infectious component being involved, as well as about potential angiographically silent CNS vasculitis.
The patient was discharged from the hospital with this diagnostic cloud of doubt lingering. She was given anti-seizure medication with the plan to follow up in one week to determine intravenous immunoglobulin (IVIG) and steroid frequency based on how she did. But in just three days, she had new onset of acute vision loss in her left eye. An MRI found an inflamed left optic nerve.
“This brings us into the demyelinating camp because it’s an optic neuritis,” Dr. Wells said.
Anti-MOG Autoimmune Encephalomyelitis
Clinicians began to suspect anti-MOG autoimmune encephalomyelitis and Dr. Van Mater called an expert in Australia, who confirmed that neuroretinitis was not uncommon in the disease. The MOG test came back high titer positive.
The MOG test has been commercially available for two years, and the disease is now being found in 18–35% of children with a first acute demyelinating episode. It is associated with a whole spectrum of demyelinating disease, Dr. Wells said.3
“When patients with MOG encephalitis have had brain biopsies, they are found to have lymphocytic perivascular infiltration in many cases,” Dr. Van Mater said. “And it’s now thought that many of the kids we previously diagnosed with [angiographically silent] CNS vasculitis—who didn’t have classic vasculitis on their biopsy but more of this perivascular lymphocytic infiltrate—were likely MOG positive.”
Treatment
The treatment is similar to that of autoimmune encephalitis treatment, the doctors said. Most pediatricians will treat AE with rituximab, and for adults the tendency is to treat with rituximab plus cyclophosphamide.
When treating autoimmune brain disease, they said, remember that not everyone needs the same treatment. Consider bridge therapy with steroids and IVIG when adding a disease-modifying anti-rheumatic drug, and consider spacing medications out rather than stopping suddenly. Also, they said, with aggressive subtypes, treat with rituximab early, and consider treating for a longer period of time and following CD19 and 20 cell counts to guide rituximab redosing.
The girl was treated with rituximab, intravenous steroids and IVIG. She has continued on the antiseizure medication because weaning gave rise to more seizures. Her vision has improved, but she had a mild flare with vision changes when IVIG was slowed. Clinicians added mycophenolate mofetil and continued every-six-month rituximab. Since being off steroids and IVIG for seven months, she’s had no flares, though her MOG remains positive two years later.