CHICAGO—In systemic lupus erythematosus (SLE), most types of severe pulmonary manifestations are relatively rare, but it’s crucial they be caught because of the potentially dire consequences, said Richard Silver, MD, professor in the Rheumatology Division at the Medical University of South Carolina, Charleston, at the 2018 ACR/ARHP Annual Meeting.
Pulmonary Manifestations
Parenchymal disease—seen in the form of acute lupus pneumonitis, acute respiratory distress syndrome, diffuse alveolar hemorrhage and chronic interstitial pneumonitis—appears in less than 5% of lupus patients. Its mortality rate can run as high as 50%.
“When you see it, you’ve got to recognize it. You’ve got to know you’ve seen it because it can be catastrophic,” Dr. Silver said.
Acute lupus pneumonitis (ALP) usually presents with abrupt fever onset, cough, pleurisy and dyspnea, and is marked by evidence of lupus activity, such as double-stranded DNA antibodies, low C3 and C4, pleural effusions and alveolar infiltrates. The initial concern should be excluding infection, with immunosuppression treatment once infection is ruled out.
Diffuse alveolar hemorrhage (DAH), also rare but potentially fatal, can resemble ALP, but if hemoptysis is also present, consider DAH, Dr. Silver said. A falling hematocrit is a telltale sign of DAH, and rituximab has shown efficacy in its treatment.1
Risk factors for pulmonary arterial hypertension (PAH) in SLE include Raynaud’s phenomenon, anti-U1 RNP antibodies, anti-cardiolipin antibodies and anti-endothelial cell antibodies. High-risk patients can be screened with pulmonary function tests and echocardiogram, though the gold diagnostic standard is right heart catheterization.
A diagnosis occurs when a high pulmonary arterial pressure with a non-elevated pulmonary capillary wedge pressure and a pulmonary vascular resistance of greater than or equal to 3 Wood units are evident.
“You might have pulmonary hypertension on an echo or even on a right heart catheterization,” Dr. Silver said, “but if the [wedge pressure is elevated], it’s not PAH. It’s diastolic dysfunction or some other cardiac issue leading to pulmonary hypertension. Unless it’s PAH, you shouldn’t embark on PAH-specific therapy.”
More therapeutic options have emerged in recent years, he said.
“We now have a host of PAH-specific therapies,” Dr. Silver said. “Most people would either use monotherapy with an oral agent, or a dual combination oral therapy using both a PDE5 inhibitor and an endothelin receptor antagonist (ERA). This really requires the input of a PAH specialist. If patients are failing mono- or dual-combination therapy, that therapy needs to be escalated, and this usually requires a multidisciplinary approach.”
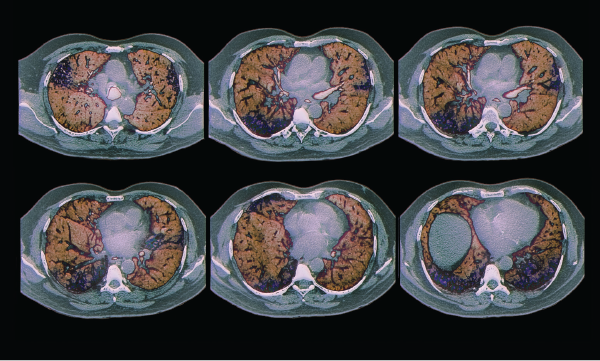
Colored computed tomography (CT) scans of axial sections through the chest of a 68-year-old patient with interstitial lung disease (diffuse parenchymal lung disease, DPLD). Parenchymal disease appears in less than 5% of lupus patients.
Zephyr / Science Source
Kidney Manifestations
Severe lupus manifestations in the kidney can prove challenging to manage, said Derek Fine, MD, a nephrologist and associate professor of medicine at Johns Hopkins, Baltimore. But he offered these suggestions on how to make the best of a challenging situation:

