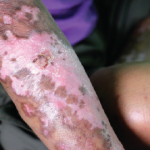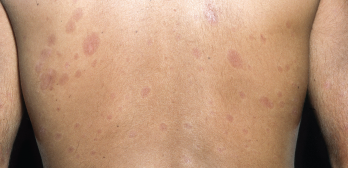
New research suggests that hardened tissues may be able to regain some plasticity.
SPL/ScienceSource.com
Systemic sclerosis (SSc) is a rare disease affecting about 49,000 U.S. adults, and it is strongly associated with high levels of morbidity and mortality.1 Of the few available antifibrotic therapies, none is targeted for SSc. However, reason for optimism exists for antifibrotic treatments in early development and clinical trials, says Jörg H.W. Distler, MD, Heisenberg Professor for Translational Matrix Biology at the University of Erlangen-Nuremberg in Erlangen, Germany. He is the lead author of a paper recently published in Arthritis & Rheumatology, “Frontiers of Antifibrotic Therapy in Systemic Sclerosis.”
“While there are some therapies used for the treatment of fibrosis in SSc, several of those treatment attempts have not proved to be effective in appropriate clinical trials, and even for those with proven efficacy, the effects are modest at best,” says Dr. Distler. “So there really is a huge, unmet medical need.”
Fibrosis is the “excessive deposition of fibrous connective tissue in an organ or tissue initiated by tissue repair programs in response to injury,” the paper’s authors describe, and fibrotic diseases can affect any organ system in the body. Fibrotic tissue responses are also common in many chronic diseases, such as atherosclerosis and pulmonary disease.2
Fibrosis was once thought to be irreversible, but recent research suggests that these hardened tissues have some level of plasticity, which may vary depending on the organ affected and the specific disease.
“We believe that different organs have different potential to regenerate. For the skin, it may not be complete regeneration of tissue, but there is the potential to restore some of the original architecture to a certain extent. We may not be able to completely reverse the process, but may induce mild regression of fibrotic changes,” says Dr. Distler. “In the past 10 to 15 years, a lot has changed in this area. SSc and other fibrotic diseases were not the main focus of the pharmaceutical industry in the past, but now, major companies are trying to develop specific antifibrotic therapies.”
A bethter understanding of the common pathways that regulate fibrotic tissue responses in affected organs led to the development of the first antifibrotic drugs, nintedanib and pirfenidone, both now approved for idiopathic pulmonary fibrosis (IPF). These two therapies have not proved effective in SSc, Dr. Distler says.
The “pathogenesis of [fibrotic] diseases is less well understood than many inflammatory diseases, and they can be harder to treat,” he says. “Fibrotic diseases, [which are] heterogeneous in nature, likely require prolonged treatment to demonstrate efficacy in clinical trials, and some are orphan diseases. It’s more difficult to recruit patients for clinical trials for therapies for these diseases.” Many patients with SSc have multi-organ involvement, such as skin and pulmonary fibrosis, which also adds to the complexity.
5-HT & Other Mediators
Early in the SSc disease process, reduced blood flow in damaged vessels can lead to the activation and degranulation of platelets.3 Antiplatelet therapy has shown promise to ease fibrosis in the aortic valve, heart, kidney and liver.4,5
Platelets contain high amounts of 5-hydroxytryptamine (5-HT) or serotonin. SSc patients have elevated levels of 5-HT in their blood, and this may be an important mediator of fibrosis in fibroblasts and mesangial cells, the study notes.6 In both humans and mice, 5-HT stimulates collagen release in fibroblasts, and mice deficient in 5-HT2B were protected from experimental skin fibrosis in one study.6 In other trials, nonselective 5-HT2 inhibitors terguride and cyproheptadine and the selective 5-HT2B inhibitor SB204741 both showed antifibrotic effects.7 In a small, non-blinded, proof-of-concept trial, SSc patients treated with terguride had lower modified Rodnan skin thickness scores (MRSSs) compared with untreated controls.8
There are other profibrotic mediators stored in human platelets, including growth factors—transforming growth factor β1 (TFGβ1), platelet-derived growth factor (PDGF), fibroblast growth factor (FGF) and vascular endothelial growth factor (VEGF)—and bioactive lipids, such as lysophosphatidic acid (LPA) and sphingosine 1-phosphate (S1P) receptor.9 Therapies targeting several of these factors are currently being studied, Dr. Distler says.
TFGβ1 is upregulated in SSc, and therapies that inhibit TGFβ signaling have been the subject of several studies. In one recent study of fresolimumab, a high-affinity neutralizing antibody that targets TGFβ isoforms, SSc patients showed MRSS decreases after one infusion of the drug, as well as reduced levels of mRNA for several TGFβ-related genes and decreased fibroblasts in fibrotic skin.10 In some studies, fresolimumab seemed to cause patients to develop high numbers of keratoacanthomas, or low-grade skin tumors, because TGFβ inhibits keratinocyte proliferation.11
Another possible target for SSc therapies is thrombin, which can induce the expression of profibrotic growth factors and is elevated in SSc patients. Dabigatran, a direct thrombin inhibitor, has shown antifibrotic effects in a bleomycin-induced lung fibrosis model and could show promise for both fibrosis prevention and treatment.12 Thromboxane A2 (TXA2) is also a possible target, because it may play a role in impaired angiogenesis in SSc. Anticoagulation therapy has been tested in patients with SSc-associated pulmonary arterial hypertension (PAH), but does not seem more effective than other therapies.13
Vitamin D receptor (VDR) is yet another regulator of fibrotic tissue responses, and SSc patients have decreased levels of this vitamin.14 VDR expression is down-regulated in SSc patients’ skin.15 VDR also regulates fibroblasts’ sensitivity to TGFβ’s profibrotic effects, and synthetic VDR agonists have reduced TGFβ’s stimulatory effects. VDR agonists studied in both preventive and therapeutic treatment of fibrosis have showed some early promise in mouse models.16
Innate Immune Response
In early SSc, patients often have inflammatory infiltrates that induce fibroblast activation and initiate tissue repair responses, says Dr. Distler. Recent research has shown that innate immune responses play an important role in SSc and other fibrotic diseases.17
Certain inflammatory mediators, such as interleukin (IL) 6, have shown promise in ongoing clinical trials. SSc patients have elevated levels of serum IL-6, and high levels of IL-6 are present in their skin lesions.18,19 IL-6 may be involved in both fibroblast activation and collagen release, and it plays a key role in the transition from innate to acquired immunity. Tocilizumab, a human monoclonal antibody against the IL-6 receptor, has shown promising results in clinical trials, says Dr. Distler. In one Phase 2, randomized, double-blind, placebo-controlled trial of subcutaneous tocilizumab, a subset of SSc patients with inflammatory, early diffuse cutaneous SSc showed improvements in many endpoints, although not all changes were statistically significant.20 A Phase 3 trial of tocilizumab is now in the recruitment phase.
B cells are also found in those inflammatory infiltrates in fibrotic skin, says Dr. Distler. The B cell-depleting CD20 antibody drug rituximab showed promise in a retrospective analysis of European League Against Rheumatism (EULAR) scleroderma trials.21 Two trials of rituximab for treatment of SSc-associated PAH and SSc-related polyarthritis are still in progress.
Antifibrotic therapies that target nuclear receptors are a newer area of interest for researchers, especially agonists of peroxisome proliferator-activated receptors (PPARs), says Dr. Distler. PPAR-γ is decreased in the fibrotic tissues of SSc patients.22 PPAR-γ agonists like thiazolidinediones may elevate low-density lipoprotein (LDL) levels. However, a pan-PPAR agonist, IVA337, did not raise LDL levels and shows antifibrotic effects in preclinical models of SSc and is in a trial for diffuse cutaneous SSc now, he says.23
Stem Cell Pathways
Evidence is increasing that the Wnt, hedgehog, Notch, Hippo and other signaling pathways play an important role in fibrosis, says Dr. Distler. Inhibitors for all of these pathways are in clinical trials or in use now, but many raise toxicity concerns for long-term use, especially Wnt signaling to the stem cell compartment.
“There is some concern that decreasing the stem cells during treatment will lead to side effects in rapidly regenerating tissues, such as the gut,” says Dr. Distler. “That is a specific concern for those treatments. Antifibrotic treatments that target fibroblast activation will also affect physiological wound healing, and this may be of particular concern in SSc, because many patients suffer from ischemic ulcers. On the other hand, people are dying from SSc-related complications, so they may be willing to risk adverse events if we can improve their disease.”
Topical application may overcome some of those safety concerns, Dr. Distler adds. “Some of those topical treatments are going into proof-of-concept trials now,” including a small molecule, C-82. “Inhaled application may also allow treatment of pulmonary disease, and local therapies may be an option for some patients, but SSc is a systemic disease. You could treat an affected organ, but not the underlying disease.”
Polypharmacologic therapy describes the simultaneously inhibition of several targets with one drug. Nintedanib, a multiple tyrosine kinase inhibitor, is an example for this approach because it targets several profibrotic pathways.24 Nintedanib is in a Phase 3 clinical trial for treatment of SSc-related ILD now.
“Multityrosine kinase inhibitors inhibit a broader spectrum of targeted molecules, and this may provide additional efficacy, but may also be associated with a higher possibility of adverse events,” says Dr. Distler. The heterogeneity of SSc is one challenge for the development of more effective therapies.
“The pathologic pathways may be different in different subsets of patients. That leads to problems in predicting response to treatment,” says Dr. Distler. “We need to better understand the different pathways that lead to different phenotypes in these patients. Progress has been made in this effort, but our classification of different phenotypes is not fine enough yet. We don’t fully understand the pathogenesis of this disease. We have so much more to do.”
Susan Bernstein is a freelance medical journalist based in Atlanta.
References
- Helmick CG, Felson DT, Lawrence RC, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Arthritis Rheum. 2008 Jan;58(1):15–25.
- Wynn TA. Cellular and molecular mechanisms of fibrosis. J Pathol. 2008 Jan;214(2):199–210.
- Hernandez-Rodriguez NA, Cambrey AD, Harrison NK, et al. Role of thrombin in pulmonary fibrosis. Lancet. 1995 Oct 21;346 (8982):1071–1073.
- Rouzaud-Laborde C, Delmas C, Pizzinat N, et al. Platelet activation and arterial peripheral serotonin turnover in cardiac remodeling associated to aortic stenosis. Am J Hematol. 2015 Jan;90(1):15–19.
- Tu X, Chen X, Xie Y, et al. Anti-inflammatory renoprotective effect of clopidogrel and irbesartan in chronic renal injury. J Am Soc Nephrol. 2008 Jan;19(1):77–83.
- Dees C, Akhmetshina A, Zerr P, et al. Platelet-derived serotonin links vascular disease and tissue fibrosis. J Exp Med. 2011 May;208(5):961–972.
- Ebrahimkhani MR, Oakley F, Murphy LB, et al. Stimulating healthy tissue regeneration by targeting the 5-HT2B receptor in chronic liver disease. Nat Med. 2011 Nov;17(12):1668–1673.
- Farina G, Lafyatis D, Lemaire R, et al. A four-gene biomarker predicts skin disease in patients with diffuse cutaneous systemic sclerosis. Arthritis Rheum. 2010 Feb;62(2):580–588.
- Nurden AT. Platelets, inflammation, and tissue regeneration. Thromb Haemost. 2011 May;105 Suppl 1:S13–S33.
- Rice LM, Padilla CM, McLaughlin SR, et al. Fresolimumab treatment decreases biomarkers and improves clinical symptoms in systemic sclerosis patients. J Clin Invest. 2015 Jun;125(7):2795–2807.
- Lacouture ME, Morris JC, Lawrence DP, et al. Cutaneous keratoacanthomas/squamous cell carcinomas associated with neutralization of transforming growth factor β by the monoclonal antibody fresolimumab (GC1008). Cancer Immunol Immunother. 2015 Apr;64(4):437–446.
- Bogatkevich GS, Ludwicka-Bradley A, Silver RM. Dagibatran, a direct thrombin inhibitor, demonstrates antifibrotic effects on lung fibroblasts. Arthritis Rheum. 2009 Nov;60(11):3455–3464.
- Johnson SR, Granton JT, Tomlinson GA, et al. Effect of warfarin on survival in scleroderma-associated pulmonary arterial hypertension (SSc-PAH) and idiopathic PAH: Belief elicitation for Bayesian priors. J Rheumatol. 2011 March;38(3):462–469.
- Arnson Y, Amital H, Agmon-Levin N, et al. Serum 25-OH vitamin D concentrations are linked with various clinical aspects in patients with systemic sclerosis: A retrospective cohort study and review of the literature. Autoimmun Rev. 2011 Jun;10(8):490–494.
- Zerr P, Vollath S, Palumbo-Zerr K, et al. Vitamin D receptor regulates TGFβ signaling in systemic sclerosis. Ann Rheum Dis. 2015 Mar;74(3):e20.
- Ding N, Yu RT, Subramaniam N, et al. A vitamin D receptor/SMAD genomic circuit gates hepatic fibrotic response. Cell. 2013 Apr;153(3):601–613.
- Wohlfahrt T, Usherenko S, Englbrecht M, et al. Type 2 innate lymphoid cell counts are increased in patients with systemic sclerosis and correlate with the extent of fibrosis. Ann Rheum Dis. 2016 Mar;75(3):623–626.
- Feghali CA, Bost KL, Boulware DW, et al. Mechanisms of pathogenesis in scleroderma. I. Overproduction of interleukin 6 by fibroblasts cultured from affected skin sites of patients with scleroderma. J Rheumatol. 1992 Aug;19(8):1207–1211.
- Koch AE, Kronfeld-Harrington LB, Szekanecz Z, et al. In situ expression of cytokines and cellular adhesion molecules in the skin of patients with systemic sclerosis. Their role in early and late disease. Pathobiology. 1993;61(5-6):239–246.
- Distler O, Distler JH. Tocilizumab for systemic sclerosis: Implications for future trials. Lancet. 2016 Jun;387(10038):2580–2581.
- Jordan S, Distler JH, Maurer B, et al. Effects and safety of rituximab in systemic sclerosis: An analysis form the European Scleroderma Trial and Research (EUSTAR) group. Ann Rheum Dis. 2015 Jun;74(6):1188–1194.
- Wei J, Ghosh AK, Sargent JL, et al. PPARγ downregulation by TGFβ in fibroblast and impaired expression and function in systemic sclerosis: A novel mechanism for progressive fibrogenesis. PLoS One. 2010 Nov;5(11):e13778.
- Ruzehaji N, Frantz C, Ponsoye M, et al. Pan PPAR agonist IVA337 is effective in prevention and treatment of experimental skin fibrosis. Ann Rheum Dis. 2016 Dec;75(12):2175–2183.
- Huang J, Beyer C, Palumbo-Zerr K, et al. Nintendanib inhibits fibroblast activation and ameliorates fibrosis in preclinical models of systemic sclerosis. Ann Rheum Dis. 2016 May;75(5):883–890.