The main symptoms—including pain, fatigue, and a feeling of stress—are not easily measured and can be difficult to describe to doctors, she said.
“It comes back to having the trust, creating the work relationship with your specialist,” she said. In the end, patients have to be their own best advocates, she said. “We have to be much better at understanding, and also presenting our diseases.”
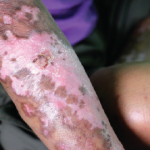
Scleroderma
Ann Tyrrell Kennedy, president of the Federation of European Scleroderma Associations (FESCA), said a major problem with scleroderma, which often involves physical disfigurement, is self-stigmatization—a “corrosive” psychological hindrance in which patients distress over their body image and are convinced other people are always staring at them. This makes social interaction difficult.
The disease’s damage to the toes and fingers generates self-consciousness, she said. “The psychological effect can be more devastating than the physical effect,” Kennedy said. “This is rarely given enough attention by clinicians.”
A Canadian group has developed a way to assess scleroderma patients’ body image, with a tool called the Brief-Satisfaction with Appearance Scale (Brief-SWAP). Results of a study using this method found a pattern of self-stigmatization. “They show that people who evaluated themselves as disfigured stigmatized themselves, particularly women and the young,” Kennedy said.
She also noted that, while small changes to physical appearance through medical procedures might help a great deal with self-esteem, major overhauls, especially to the face, can lead to problems with self-identity.
Ankylosing Spondylitis
Cor van Drogen, a member of the executive committee of the Ankylosing Spondylitis International Federation, recalled the unpleasant experience of his own diagnosis. His general practitioner didn’t recognize the disease, then an acquaintance, also a doctor, said it might be ankylosing spondylitis (AS).
van Drogen asked his general practitioner for a blood test and an X-ray, only to be told that he didn’t have AS and that those steps were unnecessary. van Drogen insisted, and finally the diagnosis was made by a rheumatologist.
“From that moment, I had another general practitioner,” van Drogen said.
He stressed the value of getting involved with patient-advocate organizations. “The right attitude,” he said, “will help the patient to get along with the disease on an acceptable level.”
Thomas Collins is a freelance medical writer based in Florida.