A 73-year-old white male presented with a one-day history of a cold, painful, right foot. The foot had a blue discoloration to it, particularly the toes. The emergency physician suspected an atheroembolic cause, given this patient’s age and history of coronary artery disease. However, the patient also reported a one-year history of painful pallor in his digits; therefore, further rheumatologic workup for presumed Raynaud’s phenomenon was requested.
History & Labs
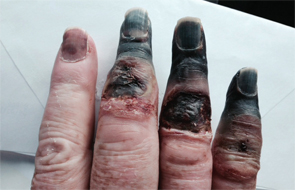
The patient’s necrotic digits on his right hand had to be amputated.
The patient reported that nine months prior to the onset of his current symptoms, he was admitted to this same hospital with similar complaints, namely a cold and painful right foot. In fact, he had been admitted multiple times over the preceding two years for painful, blue fingers and toes, thought to be secondary to microembolic disease with an unknown source.
Each time he presented with these symptoms, he was placed on a heparin drip, and his symptoms spontaneously resolved. Nine months prior, he had been placed on a heparin drip when he presented with a cold and painful right foot. Despite this treatment, on hospital day 3, he suddenly developed cyanosis with necrosis of the third to fifth digits of the right hand, distal to the PIP joints. Thromboembolic disease was suspected, and the patient was found to have a patent foramen ovale that was subsequently closed. A thrombus or vegetation was found on an atrial pacer lead as well.
He was started on warfarin. The necrotic digits of his right hand required surgical amputation, but the right foot symptoms spontaneously improved, and he was discharged home without further sequela.
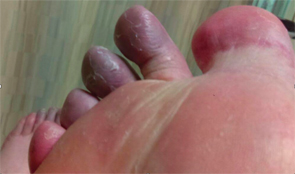
The patient’s first to fourth digits on his right foot had a bluish discoloration, as did his forefoot.
The patient has a remote history of tobacco use (quit 25 years prior to presentation). He notes that during the past one year, several of his fingers would turn white and were painful, especially when exposed to the cold. He was exposed to extremes of hot and cold weather frequently during his 32 years of service in the army and never noticed his hands becoming painful nor turning white, blue or red. He reports that he has had an unintentional 40 lb. weight loss in the past year. He bruises easily, but attributes this to the warfarin prescribed since his admission nine months earlier for presumed microembolic disease.