Currently, multiple sclerosis, Crohn’s disease and systemic sclerosis are the autoimmune diseases with the most supporting clinical data, including information from large series and randomized controlled trials. Retrospective analyses support its possible efficacy for additional conditions.6 Currently, no official U.S. guidelines exist for HSCT for rheumatological disease treatment, but the European Society for Bone and Marrow Transplantation recommends autologous HSCT as part of clinical trials for the treatment of certain subgroups of patients with severe systemic sclerosis, systemic lupus and juvenile idiopathic arthritis.7
Ongoing Treatment Concerns
Although the therapy has a great deal of potential, many clinicians are concerned about the risk/benefit ratio. The conditioning regimen puts patients at risk of complications, such as infection, secondary autoimmune disease and malignancy.8 Some studies have shown an increase in short-term mortality following HSCT, but safety of HSCT has improved since its beginnings.8,9 Researchers continue to work to develop regimens that are effective, but less toxic.
Georges Georges, MD, is an associate member at Fred Hutchinson Cancer Research Center and an associate professor of medicine at the University of Washington, both in Seattle. He is part of a team that has performed such transplants in patients with severe autoimmune disease.
“There is always a competition between transplant and nontransplant therapy to find the most effective therapy that causes the least risk and discomfort. There is always the hope that there is some simpler drug therapy that can be developed [to] target specifically the cells responsible for the disease process.” He points out that this may be partly why research interest in HSCT has lessened for certain diseases that have more effective drug treatments, such as rheumatoid arthritis.
Patient Perspectives
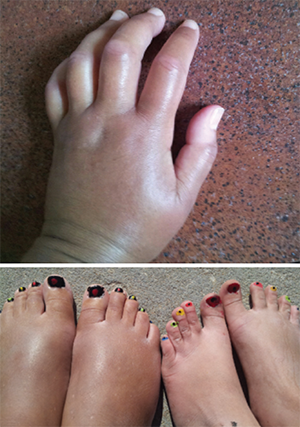
Ms. Gould was diagnosed with systemic sclerosis in 2015. These photos show her hands and feet (left) prior to the transplant.
What follows are perspectives from three women who received HSCT for disabling autoimmune conditions. All three received their treatment through Northwestern Feinberg School of Medicine’s Division of Immunotherapy for autoimmune disease.
HSCT & Lupus: Kathy Peel is a 36-year-old woman, a sales analyst, wife and mother of two. She was diagnosed with lupus in 2005.
Ms. Peel’s doctors had an extremely difficult time getting her disease under control, even with treatment. Her lung function had significantly deteriorated. Her doctor told her that she would never be able to come off prednisone and her disease would probably never go into remission.
Ms. Peel and her mother began researching alternatives. Ms. Peel says, “I found a YouTube video of a girl who had basically the same story and was in remission after HSCT. I connected with a group of people on Facebook who had either had the procedure or wanted to have it done, and I found out most of my information through them.”