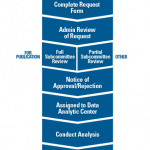
Research is an essential tool to advance medical therapies and improve patient care, but to be most effective it requires comprehensive data that represent the full patient population. Unfortunately, as highlighted by recent studies, rheumatology suffers from a lack of demographically representative patient data in clinical datasets and from randomized clinical trials. In particular, a shortage of data from historically marginalized populations has created misunderstandings about rheumatic diseases and slowed development of therapies, particularly for such diseases as systemic lupus erythematosus (SLE or lupus) that predominantly affect people of color.
Efforts to diversify data on rheumatic patients will require a commitment from researchers and practitioners to identify existing gaps in understanding and increase engagement of marginalized communities in research.

Dr. Sam Lim
Despite the dearth of diverse research data, S. Sam Lim, MD, knows the face of lupus well. A professor at Emory University School of Medicine and Rollins School of Public Health, Dr. Lim also works as the chief of rheumatology at the Grady Health System in Atlanta. “Grady is the only charity hospital in Atlanta and, given our area and the social forces at work, I predominantly see lower socioeconomic patients who identify as Black,” he says.
Dr. Lim had long considered his view of lupus patients skewed. After all, as he and co-author Cristina Drenkard, MD, PhD, wrote in a recent review, “As recently as the early 1950s … there was relatively little attention to race [of lupus patients], with the distribution of disease in the population being felt to be proportionate to the population under care at that time, which were mostly females with light hair, fair skin, and an inability to tan.”1
This perception has expanded since the first major population-based SLE study in the 1970s, but a complete picture of the lupus patient population is still developing. With a long history of volunteering with the ACR, where he has served on multiple committees and now serves on the Board of Directors, Dr. Lim is helping shape the rheumatology field’s perspective on lupus and its complicated relationship with racial identity. “New data coming from CDC lupus registries now show that my view of lupus at Grady is, in fact, the view of a typical lupus patient,” he says.
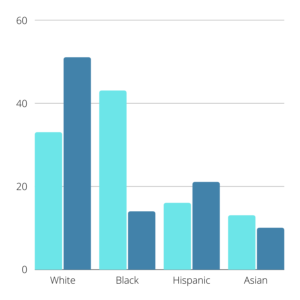
Figure 1: For each demographic group, light blue bars show representation among lupus cases and dark blue bars shows representation in randomized clinical trials. Data sourced from Falasinnu et al.