Current guidelines are inadequate to incorporate vasculitic syndromes involving skin.
Clinical Photography, Central Manchester University Hospitals NHS Foundation Trust, UK / Science Source
CHICAGO—Warren Piette, MD, professor of dermatology at Rush University Medical Center, Chicago, updated rheumatologists on the topic of cutaneous vasculitis at the ACR’s State-of-the-Art Clinical Symposium in April. He began by explaining that the current vasculitis criteria developed by the ACR in 1990 and the Chapel Hill Consensus Conference (CHCC) in 1994 are inadequate to incorporate vasculitic syndromes involving skin. This deficiency has led an international group to propose revised criteria that will soon be submitted to Arthritis & Rheumatology.
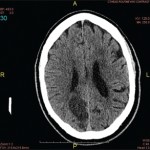
Dr. Piette focused his talk on immune complex vasculitis and anti-neutrophil cytoplasmic autoantibody (ANCA)-associated vasculitis and the purpura that are key to their diagnosis. He explained that purpura can be primary or secondary, and distinguishing the two clinically is more art than science. He emphasized the importance of lesional morphology in sorting purpura pathophysiology into simple hemorrhage, inflammatory hemorrhage or microvascular occlusion, and he also disputed a few dogmas.
Primary Palpable Purpura Are Not Specific for Vasculitis
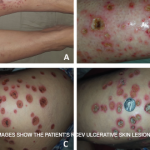
Primary palpable purpura are not specific for vasculitis. Moreover, explained Dr. Piette, vasculitis is not always palpable or purpuric. He then showed a series of slides of purpura and talked the audience through their diagnoses.
He emphasized the importance of determining if the lesion is blanchable. If the early lesion completely blanches, then it is not purpura, although it could still be vasculitis. If the early lesion partially blanches, then the patient likely has inflammatory purpura, but does not necessarily have vasculitis. Finally, if a lesion doesn’t blanch, then it could simply be a hemorrhage.
Dr. Piette described the four main purpura patterns—multi-generalized, acral, pauci-random and multi-dependent—and showed examples of each. He also noted that there is an evolving recognition that retiform purpura is also a typical morphologic pattern of cutaneous vascular occlusion. Multi-generalized purpura generally contain fewer than 100 lesions, distributed widely and often randomly. They are usually caused by a virus or drug and are only rarely urticarial vasculitis, lymphomatoid papulosis (LyP) and pityriasis lichenoides et varioliformis acuta PLEVA/Lyp, or bowel stasis vasculitis. If the patient with multi-generalized purpura is very ill, however, with multiple lesions retiform, Dr. Piette suggests that purpura fulminans be considered as a diagnosis.
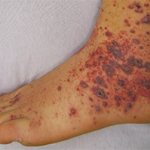
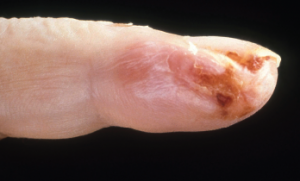
Acral purpura tend to locate on the hand and/or foot. These stocking-glove purpura are likely caused by viral infection, especially parvovirus infection. They may also be caused by sepsis/disseminated intravascular coagulation (DIC) with hypotension leading to microvascular occlusion in vasoconstricted areas. Patients who have retiform purpura in cold-exposed areas, such as ears, nose, hands and feet, likely have cryoglobulins, cryofibrinogens and/or cold agglutinins.