PopTika / shutterstock.com
A new study from Johns Hopkins University School of Medicine, published in the September 2018 issue of Arthritis Care & Research, identifies risk factors and clinical features associated with severe gastrointestinal (GI) dysmotility in patients with systemic sclerosis.1 The findings suggest a distinct pathological process may be at work in this patient group, says lead author Zsuzsanna McMahan, MD, MHS, assistant professor of medicine at Johns Hopkins, Baltimore.
Background
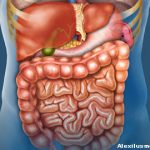
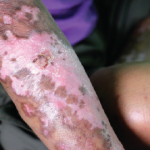
Systemic sclerosis is a complex, systemic autoimmune rheumatic disease. It attacks a variety of organs in the body and is characterized by vasculopathy, fibrosis, inflammation and autoantibody production. GI dysmotility, meaning abnormal movement of food, nutrients and wastes in the GI tract, is associated with muscle atrophy and may result in malabsorption, pseudo-obstruction and, in the most severe cases, the need for supplemental enteral or parenteral nutrition to sustain life.
GI disease, which affects 90% of patients with systemic sclerosis, presents in a variety of ways, Dr. McMahan tells The Rheumatologist. “Some are fairly mild and easily controlled while others are more extreme.”
The time intervals at which the disease progresses are also highly variable. Given the absence of biomarkers with which to predict GI complications or to assess GI disease activity in scleroderma, as well as a lack of known efficacy for disease-modifying anti-rheumatic drugs (DMARDs) in treating scleroderma-associated GI disease, medical management typically involves the treatment of complications, she says. Although severe dysmotility affects about 8% of systemic sclerosis patients, the mortality rate in patients with diffuse disease is estimated to be 85% at five years.2
“Because of the high morbidity and mortality associated with severe GI dysmotility in these patients, defining the clinical characteristics that might identify high-risk patients earlier potentially could open the door to earlier and more aggressive treatment,” Dr. McMahan explains. “Our research is trying to identify common clinical characteristics that might better define homogeneous subgroups.”
Study Methodology

Dr. McMahan
Dr. McMahan and her team performed a retrospective review of clinical features for all patients seen at the Johns Hopkins Scleroderma Center between 1999 and 2015, comparing in a cross-sectional analysis patients with severe GI disease who required supplemental nutrition (n=66) with those who had mild or no GI symptoms (n=1,736). The researchers also looked for associations with specific systemic sclerosis autoantibodies. The strongest risk factors associated with severe GI disease were male sex (odds ratio [OR] 2.47; confidence interval [CI] 95%), having myopathy (OR 5.53; CI 95%), and having symptoms of sicca (dryness in mucosal tissue; OR 2.40; CI 95%).
Making Assessments in Clinic Settings
When systemic sclerosis patients with these identified risk factors and GI symptoms are evaluated in rheumatology clinics, doctors should consider earlier testing to evaluate for dysmotility, Dr. McMahan says. Such studies may more precisely guide therapy. Initial interventions are symptom focused and may include addressing acid reflux (such as with a wedge pillow at night, modifications in lifestyle and diet, and prescribing proton pump inhibitors or H2 receptor blockers) and treating constipation (through diet and lifestyle modifications and introducing over-the-counter medications). At this stage, opioids and other such drugs should be minimized because they have a negative impact on motility and an increased risk for GI complications.
If patients are not responding to initial interventions, or if symptoms are more severe, the doctor should consider referral to a gastroenterologist, Dr. McMahan says. “The main point is to listen to your patients’ concerns. Pay attention to signs of early GI problems and try to treat them the best you can. And if the patient progresses more rapidly, consider earlier referral to the GI specialist for a workup—preferably one experienced with systemic sclerosis.”
When systemic sclerosis patients with identified risk factors & GI symptoms are evaluated in rheumatology clinics, doctors should consider earlier testing to evaluate for dysmotility.
Tracy M. Frech, MD, associate professor of internal medicine in the Division of Rheumatology, University of Utah, Salt Lake City, who has a research and clinical interest in systemic sclerosis, credits the Hopkins study for highlighting the challenges of GI disease in patients with systemic sclerosis. “We need to identify the systemic sclerosis patients at the highest risk for GI dysmotility, especially with regard to their clinical features,” she says.
“The article helps a clinician think more closely about how to treat a male scleroderma patient with myopathy. In this case, a questionnaire, such as the UCLA Scleroderma Clinical Trial Gastrointestinal Tract Instrument, Version 2.0, could be used to assess risk of severe GI involvement,” Dr. Frech notes.3 This 34-item questionnaire is available in multiple languages and can be used for online screening. “In our clinic, everyone with scleroderma fills out the questionnaire, so I can get a quick look at their gastrointestinal issues,” Dr. Frech says. Other questionnaires are available, as well.
The Bottom Line
“I think the key take-home message for rheumatologists is the importance of asking these GI questions. It can be hard in our day-to-day practice because we’re so focused on musculoskeletal concerns,” Dr. Frech says. “And when it comes to a physical exam, the abdomen is a bit of a black box. However, this new research supports the rheumatologist in asking routinely about GI issues and doing a better job of distinguishing between mild and moderate to severe complaints. It highlights that as rheumatologists we can do better.
“The important thing is to ask the questions,” Dr. Frech continues. “I just gave a talk in Boise, Idaho, at the Scleroderma Foundation Chapter, trying to make patients more aware of gastrointestinal issues and the information that is available online. If they are having worsening GI symptoms, I encourage them to talk to their doctor.”
Larry Beresford is a medical journalist in Oakland, Calif.
References
- McMahan ZH, Paik JJ, Wigley FM, et al. Determining the risk factors and clinical features associated with severe gastrointestinal dysmotility in systemic sclerosis. Arthritis Care Res (Hoboken). 2018 Sep;70(9):1385–1392.
- Steen VD, Medsger TA Jr. Severe organ involvement in systemic sclerosis with diffuse scleroderma. Arthritis Rheum. 2000 Nov;43(11):2437–2444.
- Baron M, Hudson M, Steele R, et al. Validation of the UCLA Scleroderma Clinical Trial Gastrointestinal Tract Instrument version 2.0 for systemic sclerosis. J Rheumatol. 2011 Sep;38(9):1925–1930.