Rheumatologists should prepare their practices now for the Recovery Audit Contractor (RAC) program, being rolled out nationwide by the Centers for Medicare & Medicaid Services (CMS) as part of its arsenal to identify and correct improper payments and prevent fraud, waste, and abuse in the Medicare system.
Anyone who bills Medicare fee-for-service is open to a RAC audit. A three-year demonstration of the RAC program that ended in March 2008 heavily targeted codes used by rheumatologists—those used for injectable drugs, in particular—while three of the four RACs in the permanent nationwide program indicate that they will target IV hydration therapy, which is billable only for one unit per patient per date of service.
Some physicians in the demo regarded the thirdparty RAC companies as “bounty hunters” (it was the first time the Medicare program had paid contractors on a contingency- fee basis) operating without sufficient CMS oversight, imposing undue administrative burdens on physician practices, and lacking clinical expertise to adjudicate claims appropriately. CMS says it has modified the permanent program to address those flaws and ensure a fair and smooth auditing process. Rheumatologists can make specific preparations that allow them to respond to audits with minimal disruption to their practices, minimize recoupment disputes, and perhaps even avoid being audited in the future.
Program Rationale and Process
Out of concern that the Medicare Trust Funds may not be adequately protected against improper payments by existing error detection and prevention efforts, Congress directed CMS to use RACs to identify and recoup Medicare overpayments under Section 306 of the Medicare Modernization Act of 2003, and directed CMS to make the program permanent and nationwide by 2010 under Section 302 of the Tax Relief and Health Care Act of 2006. According to the CMS, RACs were implemented so that physicians and other providers can avoid submitting claims that do not comply with Medicare rules, CMS can lower its error rate, and taxpayers and future Medicare beneficiaries are protected.
CMS has contracted with four regional RACs for the permanent nationwide program, and each will use proprietary auditing software to review paid claims from Medicare Part A and B providers to ensure that they meet Medicare statutory, regulatory, and policy requirements and regulations. CMS will pay RACs on a contingency fee basis (i.e., they retain a portion of the monies recovered) on overpayments and a percentage basis for all underpayments they find. (The new national RACs can be found at www.cms.hhs.gov/RAC.)
The RACs use automated review for claims that clearly contain errors resulting in improper payments (e.g., claims for duplicate or uncovered services, or which violate a written Medicare policy or sanctioned coding guideline), in which case the RAC notifies the provider of the overpayment amount. Where there is a high probability (but not certainty) that the claim contains an overpayment, the RAC requests medical records from the provider (including imaged medical records on CD or DVD) to conduct a complex review and make a determination as to whether payment of the claim was correct or whether there was an overpayment or an underpayment.
As of the end of October 2009, all four RACs have the ability to begin reviewing claims, while they are realistically expected to ramp up their activities in all states some time in 2010, says Connie Leonard, director of CMS’s Division of Recovery Audit Operations. The RACs are going to start with automated review, then move into diagnosisrelated group validation, complex review, and eventually medical necessity cases, says Leonard.
When overpayments are confirmed, the RACs issue letters demanding repayment in 30 days, while the provider’s Medicare carrier or intermediary performs the collection. For confirmed underpayments, RACs inform the carrier or intermediary who then forwards the additional payment to the provider.
CMS is using a Web-based data warehouse to ensure that RACs do not review a claim that had previously been reviewed by another entity, such as a Medicare carrier, fiscal intermediary, Office of Inspector General, or Quality Improvement Organization (QIO).
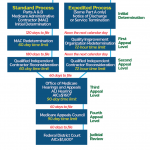
Providers can repay an overpayment by check (or installment plan) on or before 30 days after receiving the RAC demand letter. Medicare contractors (who make the actual claim adjustments) use recoupment—reducing present or future Medicare payments—on Day 41. Physicians who wish to dispute overpayment charges take their cases through the usual Medicare claims appeal process.
If physicians disagree with the RAC’s determination, Leonard explains, they should either 1) pay by check by Day 30 and file for appeal by Day 120 of the demand letter; 2) allow recoupment on Day 41 and file for appeal by Day 120; 3) stop the recoupment by filing an appeal by Day 30; or 4) request or apply for an extended payment plan and appeal by Day 120.
RACs also offer a “discussion period” from the date providers get a detailed review results letter until the date of recoupment for providers to discuss with their RAC an improper payment determination outside the normal appeal process. RACs are required send the detailed review results letter to providers following all complex reviews within 60 calendar days of the receipt of the medical records, alerting the physician that there is an improper payment and they are going to get a demand letter, says Leonard. “The physician will usually get two letters: the detailed review results letter saying the RAC reviewed the claim and found improper payment for these specific reasons, and then they’ll get a demand letter indicating the amount of overpayment, and the physician’s appeal rights. The amount of time between those two letters depends on the backlog of cases at the contractor level—it could be 30 to 60 days. So physicians are going to know a little bit before that demand letter that there’s an improper payment,” notes Leonard.
REFINEMENTS IN PERMANENT RAC PROGRAM
All new issues a RAC wishes to pursue for overpayments must be validated by CMS or an independent RAC validation contractor and posted to a RAC’s Web site before widespread review.
- Each RAC must hire a physician medical director as well as certified coders. A provider may request the credentials of the individuals making medical review determinations and request to speak to a RAC’s medical director regarding a claim denial.
- RACs cannot audit claims earlier than three years from the start of the program, with a maximum look-back date of October 1, 2007 (replacing a four-year look-back period in the demo).
- RACs are limited to requesting 10 medical records per 45 days from a solo physician, 20 medical records from a small practice of two to five physicians, 30 from a group of six to 15, and 50 from a large group of more than 16 physicians.
- RACs must send a detailed review results letter to providers following all complex reviews within 60 calendar days of the receipt of the medical records.
- RACs must pay back contingency fees when an improper payment determination is overturned at any level in the appeals process (demo RACs were allowed to retain them on determinations overturned on second- and third-level appeal).
- RACs must have in place by January 1, 2010 a Web-based claim status platform that will allow providers to track the status of medical record submissions to RACs.
- A RAC validation contractor will conduct a thirdparty review of RAC claim determinations and provide annual accuracy scores for each RAC.
Demo Program Lessons
In 2005, a RAC demonstration project was launched in California, Florida, and New York, states selected because they are the largest states in terms of Medicare utilization. The demonstration was expanded in 2007 to include Massachusetts, South Carolina, and Arizona.
Some physicians who were audited by a demo project RAC found the experience to be onerous. Some RACs demanded multiple physician repayments for claims that had previously been reviewed and adjudicated by a local Medicare carrier, misapplied codes, demanded hundreds of medical records from single practices, exceeded time limits for reviewing claims, interpreted clinical guidelines inappropriately, and applied new regulations retroactively to previously performed procedures, according to Michael Schweitz, MD, a rheumatologist from West Palm Beach, Fla., who was audited during the RAC demo program, and who testified before a Congressional committee last spring about RAC activities. “One six-physician practice was asked to pay back $100,000” in alleged overpayments, says Dr. Schweitz.
In another case, Dr. Schweitz notes, a RAC sent demand letters to hundreds of Florida physicians asking for refunds or records as far back as 2003 pertaining to procedure codes 64470–64476 (facet joint injections) asserting that they must be performed and billed with a concurrent code for fluoroscopic guidance. The RACs cited commentary from the Federal Register as their authority, when no CMS policy had been developed or distributed until 2007 when a Local Coverage Determination was formally adopted and published, says Dr. Schweitz. “The main flaw in the demo project was that there was not adequate oversight by CMS. RACs were not following guidelines and were making medical necessity determinations without proper expertise,” he adds.
One-third of provider appeals (physician, hospital, and other providers) were successful during the demo program, according to a June 2008 CMS evaluation report.1
CMS has made programmatic revisions designed to ensure that the permanent RAC program avoids these demo program flaws (see “Refinements in Permanent RAC Program,” p. 20). For example, all new issues that a RAC wishes to pursue for overpayments must be validated by CMS or an independent RAC validation contractor and posted to a RAC’s Web site before widespread review.
Preparation Advice
Physicians can minimize practice disruption from RAC audits, as well as future improper payments, by taking corrective actions. The majority of improper payments under the RAC demo program stemmed from providers billing for services that were incorrectly coded or did not meet Medicare’s medical necessity policies, according to the CMS evaluation report.
The ACR is in the process of creating an Audit Toolkit for rheumatologists and their staff, and plans to have it available by January or February 2010, according to Antanya A. Chung, CPC, CPC-I, CRHC, CCP, ACR director of practice management. “We are aware of the burden that audits can bring on a practice, both financially and emotionally, and the ACR currently sends its coding and audit specialist to affiliated state society meetings to talk with physicians and their staff on current coding issues,” she says. The ACR also provides a wide variety of coding and billing resources on its Web site at www.rheumatology.org/practice.
Based on discussions with consultants, medical societies, and physicians affected by RAC audits, Dr. Schweitz offers several recommendations to prepare for RAC audits:
- Have a preset compliance plan for CMS regulations and test it by proactively reviewing a sample of your charts and charges periodically.
- If you hire a consultant, have him or her work with your practice’s attorney to ensure that the information they review is privileged to preempt an uncontrollable whistleblower scenario if errors are discovered.
- Ensure that your documentation and coding activities are detailed and in synch with CMS guidelines.
- Have some kind of disease activity measure to add objective detail to your patient medical records (e.g., the RAPID 3 to quantify a patient’s reported physical function, pain, and patient global estimate). Consider adding a self-report joint count as a fourth disease activity index.
- Designate someone in your practice as a dedicated point person to deal with the RAC; ensure that he or she maintains close communication with the practice’s physicians and administration.
- If a RAC issues a demand letter, make sure the practice was paid for those services in the first place, and make sure they have not already been adjudicated by a local Medicare carrier.
- Document every letter you receive and send when interacting with the RAC.
- If you think you’re correct, be firm and appeal as quickly as you can; if not, pay as soon as you can.
Christopher Guadagnino is a medical journalist based in Pennsylvania.