Spinal cord involvement has been documented in 5% of patients, but it is rarely the only manifestation.15 The thoracic cord is the predominantly affected site. A careful medical evaluation must be performed to confirm the diagnosis of PCNSV and to exclude other conditions associated with acute or subacute transverse myelitis.
Angiography-negative, biopsy-positive PCNSV can occur in patients with vasculitis limited to small vessels whose detection is beyond the resolution of conventional angiography.8 These patients often have a cognitive dysfunction at presentation, marked elevation in CSF total protein level, meningeal or parenchymal enhancing lesions on MRI, respond favorably to treatment, and have a good outcome.
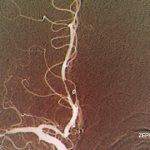
Around a quarter of PCNSV biopsy-positive patients have evidence of vascular deposits of amyloid.16 Brain biopsies show granulomatous vasculitis and vascular deposits of amyloid β peptide (see Figure 1). The relationship between these cases and older patients with amyloid deposition but no vascular inflammation (CAA) is uncertain. Patients with PCNSV with amyloid deposits are older at presentation than those with PCNSV without amyloid but younger than patients with CAA and no vasculitis. Patients with PCNSV with amyloid have a high frequency of cognitive dysfunction at presentation and enhancing meningeal lesions on MRI. As the case described above illustrates, these patients usually have a monophasic disease course and generally respond well to immunosuppressive treatment.
PCNSV may present with prominent leptomeningeal enhancement on MRI.17 These patients have an acute clinical onset, cognitive dysfunction is frequently present, and cerebral angiography or MRA are negative. CNS biopsies show a granulomatous vascular inflammation, often associated with CAA. Almost all patients respond to corticosteroid therapy (alone or combined with immunosuppressive agents), with resolution of MRI enhancement and an overall favorable course.
Rapidly progressive PCNSV represents the most severe end of the clinical spectrum of this form of vasculitis.18 Patients have a rapidly progressive course and often a fatal outcome. In these patients, disease is characterized by bilateral, multiple, large cerebral vessel lesions on angiograms and multiple bilateral cerebral infarctions. The predominant histopathological pattern is granulomatous and/or necrotizing. These patients respond poorly to the traditional immunosuppressive treatment.
Approximately 4% of PCNSV patients present with a solitary tumor-like mass lesion.19
An association with CAA was observed in 29% of these patients. Excision of the lesion may be curative; however, in some patients, aggressive immunosuppressive therapy has resulted in a favorable outcome, obviating the need of surgery.
Intracranial hemorrhage (IH) is a presenting manifestation in 11% to 12.2% of patients.20 Intracerebral hemorrhage is the most common, followed by subarachnoid hemorrhage. These patients have less frequently altered cognition, a persistent neurologic deficit, or MRI evidence of cerebral infarctions during the disease course. Necrotizing vasculitis is the predominant histopathologic pattern on biopsy.
Differential Diagnosis
Given the different therapeutic and prognostic implications, it is essential to differentiate between PCNSV and both its mimics as well as secondary causes of CNS vasculitis. The most common mimics of PCNSV are reversible cerebral vasoconstriction syndromes. Grouped under this category are several disorders with different appellations (such as Call-Fleming syndrome, postpartum angiopathy, migrainous vasospasm, and drug-induced cerebral vasculopathy) producing symptoms by vasoconstriction rather than vasculitis.21 Differentiation is crucial because immunosuppressive therapy beyond a short course of prednisone is not warranted for syndromes caused by vasoconstriction (see Table 5).