Clint Thayer
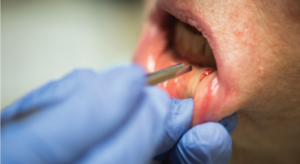
Labial salivary gland biopsy (i.e., lip biopsy) is a useful tool to help diagnose Sjögren’s syndrome in suspected patients, but most rheumatologists are not trained to perform the minimally invasive procedure. A new, 40-minute training video and slide presentation with step-by-step instructions may help them fill that critical skill gap. Two rheumatologists collaborated to create the video, which they are making freely available via YouTube.
“Trying to establish a diagnosis of Sjögren’s [syndrome] can be really challenging. … In many situations, a lip biopsy is recommended,” says Sara McCoy, MD, MS, assistant professor of medicine and director of the University of Wisconsin Health Sjögren’s Syndrome Clinic, Madison. She and Robert W. Ike, MD, associate professor emeritus of internal medicine at the University of Michigan in Ann Arbor, created this video based on a training workshop on labial gland biopsy which they led together at the 2019 ACR/ARP Annual Meeting.
Delayed Diagnosis
Many patients with suspected Sjögren’s syndrome who don’t have access to large medical centers face long delays in getting this biopsy because rheumatologists must often refer patients to an otolaryngologist for the biopsy, and then a trained pathologist must be available to interpret results, says Dr. McCoy.
“So there are two weak links in the chain.” To speed up the process, she says, “We can address a major one, which is having a rheumatologist do the biopsy bedside. It’s a simple procedure, minimally invasive and something we can accomplish on our own. This makes it better for the patient, better for the provider.”
There are no ACR-approved diagnostic criteria for Sjögren’s syndrome. Thus, many rheumatologists use the 2016 ACR/EULAR Classification Criteria to help make clinical diagnoses by using the results of five different tests, such as serological tests for anti-Ro antibodies, to rule out other causes for a patient’s symptoms.1 (Note: Classification criteria are designed to identify patients for inclusion in clinical trials and research studies and, thus, create a more uniform group of patients. They are not intended to be used for diagnostic purposes.)
In a weighted score in which four or more points are required to classify a patient with Sjögren’s syndrome, a positive labial salivary gland biopsy is worth three points, highlighting the value of this procedure for diagnosis.
Rheumatologists who conduct Sjögren’s syndrome research and diagnose patients in clinic say video-based procedure training is welcome, especially because in-person learning has mostly halted due to COVID-19. Free video training on performing a lip biopsy would be useful for community providers, agrees Jason E. Liebowitz, MD, who practices at Morristown Medical Center in Rockaway, N.J.
“Labial [salivary gland] biopsy can provide data to establish a Sjögren’s syndrome diagnosis, particularly in patients with subjective symptoms and signs, but negative or equivocal antibody studies. When read by an experienced pathologist, the objective data provided by a biopsy can be of great help. The biopsy itself has minimal risks, but the difficulty is finding a physician who is willing and able to perform this biopsy correctly,” such as an otolaryngologist, Dr. Liebowitz says. “A video would be very helpful for learning the proper technique and allowing for remote education, especially during the pandemic.”
“Labial [salivary gland] biopsy is a useful tool for diagnosis of Sjögren’s syndrome in patients who have clinical symptoms concerning for this condition but negative serology, which is not uncommon,” says Alireza Meysami, MD, CPE, RhMSUS, head of the Division of Rheumatology at Henry Ford Health System and associate professor of medicine, Wayne State University School of Medicine, Detroit.
‘Labial biopsy is a useful tool for diagnosis of Sjögren’s syndrome in patients who have clinical symptoms concerning for this condition but negative serology, which is not uncommon at all.’ —Dr. Meysami


