One of my fellows could take better care of his patients if it weren’t for the attendings getting in his way. Or so he tells me.
I can hear the howls of protest already. This statement isn’t fair—it is too broad, it doesn’t fairly depict the nuances of the situation or his point of view. First, I should point out that I know for a fact the trainee in question does not read this column, so I think I am safe, as long as none of you tell on me.
Should he find out, I would quote Erma Bombeck. If you are of a certain age, you may recall Ms. Bombeck was a nationally syndicated writer and humorist, whose columns were read by millions. She was also a wife and mother, who often wrote about her own life experiences. As you might imagine, as her children aged, they found this less amusing. One day, her children held an intervention: They informed her that if she was going to write about them, then she should be more even-handed in her depiction of them. To this, Ms. Bombeck responded with the same motherly affection and tenderness I would pass on to my own trainee, should he raise any objections: “Go out, and get your own column.”1
Honestly, the dispute comes down to a single patient, and I don’t know all the details. As a program director, I often hear bits and pieces about what irritates the fellows about various faculty members (including—more often than I like to admit—me). As in any family, however, not all arguments were meant to be voiced, and over the years, I have decided I should function less in loco parentis and more in loco avunculus—I try to lend a sympathetic ear, give some free advice when I can and slip them a $20 when Dad is being especially tough.
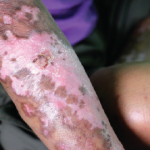
This particular patient is a young woman who has centromere-positive, limited scleroderma, whose care the fellow had inherited. The fellow noted, astutely, that she had a little interstitial lung disease, and over the past year, had developed a little more.
The fellow fought to start treatment, in this case, with mycophenolate mofetil, imagining that a few pills now would save her from needing a lung transplant later. His attending demurred, arguing the lung disease was still asymptomatic, and watchful waiting was all that was needed at this time.
I certainly understand the impulse to treat—I often joke with colleagues that if I wanted to just watch sick patients become sicker, I would have become a neurologist. I am glad some physicians are attracted to this important work, but I find the management of diseases like stroke and amyotrophic lateral sclerosis to be incredibly depressing. I became an internist because I want to be able to make people better.
A true product of my training, for any patient’s complaint, I can come up with a pill. This is probably one reason why my clinic visits run long; I just can’t resist giving a patient a Medrol dose pack for his slipped disc or a steroid cream for his nummular eczema. From the legions of discharged patients who walk out with a prescription of docusate clutched in their hands, I know many of you feel the same way.