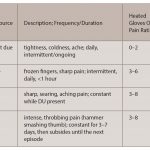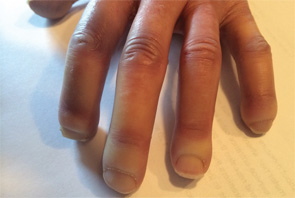
Acroosteolysis of the hands in a patient with scleroderma.
Image Credit: Lauren Tarsi
Scleroderma is a rare rheumatologic autoimmune disease that affects the skin and can also affect other organs. Due to excess formation of scar tissue, blood flow to the extremities is decreased, primarily to the hands, and tissues often become hypoxic, resulting in sclerodactyly and proximal skin involvement.2 The incidence of scleroderma in the U.S. is 50–300 cases per 1 million, and it most commonly affects women from age 30–50.1
There are two main types of scleroderma: localized and systemic. Localized scleroderma is a milder form of the disease, normally affecting the skin and less commonly, the muscles, joints and bones. Tightening of the skin usually occurs on the hands and face, and the skin often appears shiny.
Systemic scleroderma is a more severe and progressive form of the disease and can affect all internal organs, including the lungs, liver, heart, kidneys, esophagus and bowels. This type of scleroderma can be life threatening or may cause severe complications.1,3
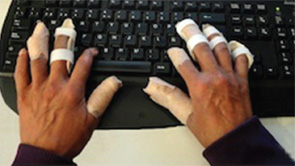
Adaptive equipment fosters functional independence in activities of daily living: Finger splints facilitate use of a computer keyboard.
There’s no cure for scleroderma; however, many patients benefit from physical and occupational therapy to address impairments commonly associated with the disease.
Acroosteolysis, Fatigue & Other Complications
Acroosteolysis, found in 20–25% of patients with systemic scleroderma, is a disease that causes a destructive lytic change to the distal phalanges, causing the bone to shorten (see Figure 1).2 On X-rays, the distal phalanges take the shape of a small pyramid or a flattened ridge.
One of the biggest limiting factors for patients with scleroderma is fatigue, either stemming from the disease itself or due to the side effects of medication.6,8 Fatigue can sometimes make routine activities of daily living (ADLs) difficult.6,11 Patients may not be able to work to the extent that they used to or will require additional time or more frequent rest breaks, depending on their occupational requirements.

This photo shows a key holder with a built-up handle.
Ulcers on the fingers and toes are a common problem and are evident in more than half of patients with scleroderma. These ulcers develop due to repeated microtrauma and increased use of the hands, underlying calcinosis and impaired blood flow.5 It’s critical that ulcers be managed immediately. Educating the patient to recognize and immediately report these ulcers is an important aspect of care. The longer the ischemia continues into the digits, the higher the risk that the ulcer won’t heal and, ultimately, will develop into a chronic ulcer.6
Primary Therapy Goals
The main goal of therapy for patients with scleroderma is to retain range of motion. Because the skin can become taut, the patient may experience a permanent loss in range of motion.9