Data from the ACR’s Rheumatology Informatics System for Effectiveness (RISE) were used by rheumatology researchers in a crop of new studies that will be presented at the 2018 ACR/ARHP Annual Meeting, Oct. 19–24 in Chicago. Six abstracts, including four oral and two poster presentations, were accepted for this year’s meeting. They explore topics ranging from therapy-use patterns to the effect of common comorbidities on rheumatic diseases.
RISE 101
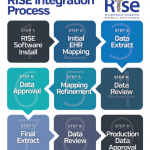
RISE is electronic health record (EHR) compatible and HIPAA compliant and includes data from more than 9 million patient encounters. The registry was created to help MIPS-eligible clinicians adapt to new payment and delivery models, and to utilize EHR data against benchmarks to assess quality of patient care. Rheumatologists and MIPS-eligible members of the broader interprofessional team may use RISE to meet reporting requirements under the Medicare Access and CHIP Reauthorization Act (MACRA) and qualify for positive payment adjustments.
“RISE is a powerful and exciting tool for research. Rheumatologists participating in RISE are creating a new source of big data that houses our collective wisdom and experience taking care of patients,” says Jinoos Yazdany, MD, MPH, chair of the ACR Committee on Registries and Health Information Technology; associate professor, Division of Rheumatology, at the University of California, San Francisco; and co-author of one of the new RISE abstracts. “We now have the opportunity to mine this data to learn how to best care for our patients, particularly those with rare conditions that are difficult to study.”
Abstracts at a Glance
Abstracts using data from RISE that will be presented at this year’s Annual Meeting include:
- “The Effect of Concomitant Diabetes on RA-Related Outcomes: Results from the ACR’s RISE Registry” (poster, Oct. 21, 9–11 a.m.): Researchers at the University of Alabama at Birmingham (UAB) analyzed data from RISE on 3,897 patients with both rheumatoid arthritis (RA) and diabetes to examine the effect of this comorbidity on RA-related physical function.
- “Rheumatologists Participating in the RISE Registry Succeeded in the First Year of the Merit-Based Incentive Payment System (MIPS)” (poster, Oct. 22, 9–11 a.m.): Dr. Yazdany and ACR staff combined efforts to analyze 346 rheumatology providers from 125 practices who used RISE to complete MIPS submissions for payment reimbursements in MACRA.
- “Practice Variation in the Use of Non-TNFi Biologics or Tofacitinib: Data from the Rheumatology Informatics System for Effectiveness (RISE) Registry” (oral, Oct. 22, 2:30 p.m.): Rheumatologists at multiple U.S. centers analyzed how different rheumatology practices in RISE prescribed newer biologic DMARDs for their patients.
- “Patterns of Biosimilar Use in the Rheumatology Informatics System for Effectiveness (RISE) Registry” (oral, Oct. 22, 3:30 p.m.): Rheumatologists from multiple U.S. centers used RISE data to analyze trends in prescription of the biosimilar for infliximab for the first 18 months after its approval in the U.S.
- “Do Patients with Moderate or High Disease Activity Escalate RA Therapy According to Treat-to-Target Principles? Results from the ACR’s RISE Registry” (oral, Oct. 23, 4:30 p.m.): The UAB researchers also used RISE data to track how often RA patients with higher disease activity adjusted their therapy to achieve either low disease activity or remission targets recommended by ACR and EULAR clinical practice guidelines.
- “Disease Activity and Its Measurement in Patients with RA Across the U.S.: Data from the Rheumatology Informatics System for Effectiveness (RISE)” (oral, Oct. 23, 5:30 p.m.): Researchers analyzed large variations in disease activity or remission among 56,850 patients from 71 rheumatology practices in RISE, including factors that may explain these wide disparities.
Tracking Rheumatology-Specific Outcomes
RISE stores data from rheumatology practices across the country, and that’s helpful for researchers like Katherine P. Liao, MD, assistant professor, Harvard Medical School, whose abstract tracked prescription patterns for a newer therapy, infliximab-dyyb. “This provided us with one way to obtain a bird’s-eye view of uptake of biosimilars in rheumatology,” says Dr. Liao. “A rheumatology-specific registry is enriched for rheumatology-related outcomes and medications, and there is generally higher accuracy for rheumatology codes compared to registries that contain all subjects. I do a lot of work using EHR data, and it is often not easy to pull out only subjects followed in a rheumatology practice. In the case of RISE, we know that everyone is followed by a rheumatologist.”