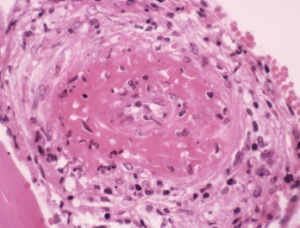
Light micrograph of a section through a human artery, showing a large thrombus (blood clot, center) due to cryoglobulinemia.
CNRI / Science Source
A study that focused on the detection and immunological characteristics of cryoglobulins provides insights for rheumatologists and other rheumatology providers, as well as lab professionals.
Co-researchers Marie N. Kolopp-Sarda, PharmD, PhD, and Pierre Miossec, MD, PhD, Clinical Immunology Unit, Department of Immunology and Rheumatology, University of Lyon, France, included in their retrospective study, published in Arthritis & Rheumatology, a large cohort of 13,439 patients who were tested for cryoglobulins—immunoglobulins (Ig) that precipitate in cold temperatures—from January 2010 to December 2016 in Lyon.1
Previous studies on the characteristics of cryoglobulins vary due to population selection bias and because of different methods to detect and characterize cryoglobulins, the researchers noted. “The topic is usually seen as complex and even mysterious,” Dr. Miossec says.
The Study
The researchers analyzed cryoglobulin isotype, clonality, concentration and rheumatoid factor in cryoprecipitate, as well as serum complement and rheumatoid factor. They also analyzed markers of gammopathy, viral infection and autoimmunity.
If no cryoprecipitates were detected, one or two blood samples were analyzed to confirm the negative result. Cryoglobulins were identified by electrophoresis-immunofixation of the dissolved cryoprecipitate with various antisera and were then classified by their immunoglobulin clonality profile, according to the classification of cryoglobulin (type I: monoclonal Ig; type II: monoclonal Ig with rheumatoid factor activity; type III: polyclonal Ig with rheumatoid factor activity). Rheumatoid factor activity was measured in the cryoprecipitate and in the serum aliquot. Complement functional activity and C3 and C4 concentration also were measured. Researchers also combined biological data with the most frequent underlying diseases associated with cryoglobulin detection.
Autoantibodies identified as markers of an autoimmune context included double-stranded DNA antibodies, often associated with systemic lupus erythematosus; anti-SSA/Ro60 Ab, often associated with Sjögren’s syndrome; and anti-cyclic citrullinated peptide Ab, associated with rheumatoid arthritis.
Results from the Cryoglobulin Analysis
Cryoglobulins were detected in 1,675 (1,018 women and 657 men; with a mean age of 54 years) of the 13,439 patients. In the full cohort, 89% tested negative for the first sample; 18.5% were retested to confirm the result, and 8.9% then tested positive.
The specialties of origin for the patients were internal medicine (42.9%), neurology (15.1%), hepatology (9.6%), nephrology (9.5%), rheumatology (7.8%), dermatology (5.5%), pulmonary medicine/cardiology (4.2%), hematology (3.7%) and infectious diseases (1.8%).
The study also found that complement activation by immune complexes—specifically, IgM cyroglobulin associated with IgG—is one of the mechanisms contributing to cryoglobulinemic vasculitis, especially hepatitis C-associated cryoglobulinemic vasculitis.
Type I cryoglobulins were present in 9.3% of those who tested positive. About 79% of the type I cryoglobulins were composed of monoclonal IgM, and nearly 21% were monoclonal IgG.
Type II cryoglobulins were found in 788 patients (47%), with 64.9% of the cryoglobulins being monoclonal IgMκ, 19.3% IgMλ, 10.4% IgGκ, 4.4% IgGλ and 1% IgAκ or IgAλ.
Type III cryoglobulins were found in 43.7%. These were most frequently polyclonal IgG and IgM, followed by polyclonal IgG or IgM alone.
Both cryoprecipitate and serum were rheumatoid factor positive in 21.6% of patients with type II cryoglobulins and 10.1% of patients with type III cryoglobulins.
Among the larger patient cohort of more than 13,000 patients, 40% were tested for their autoimmune antibody status. Of those, 11.2% were positive for at least one autoantibody. Among them, 25.4% were positive for cryoglobulin. Type II cryoglobulin was significantly less frequent than type III cryoglobulin in patients with an autoimmune diagnosis. Improvement of techniques used to detect rheumatoid factor in a cryoprecipitate is needed, the researchers note in the study.
The study also found complement activation by immune complexes—specifically, IgM cyroglobulin associated with IgG—is one of the mechanisms contributing to cryoglobulinemic vasculitis, especially hepatitis C-associated cryoglobulinemic vasculitis, the researchers write.
Lab Transport & Clinical Implications
In addition to clinical insights, one important point addressed in the study is the lab procedures that can contribute to false negative results. “Strict preanalytical conditions must be respected for cryoglobulin detection, conditions of sampling, transport and treatment, to reduce loss of cryoglobulin responsible for false negative results,” the researchers write.
Despite the use of validated procedures, nearly 9% of patients with a negative first test for cryoglobulins tested positive on a second sample. Thus, in the case of negative detection with a suggestive clinical context, repeat cryoglobulin testing is recommended, say the researchers.
Although it can be challenging to improve sample transportation procedures in a large hospital, it still is important to consistently educate nurses and technicians about cryoglobulin sample detection. The researchers described the best ways to transport blood samples for cryoglobulins in a previous paper (see sidebar, below).2
Takeaways
Rheumatologist Lindsay S. Lally, MD, Hospital for Special Surgery, New York, praises the study’s large patient sample. “It adds much to our understanding about the epidemiology and immunologic phenotypes of cryoglobulinemia,” she says. She was surprised that only 8% of the samples originated from rheumatology, but believes this is part of the heterogenous and multisystem nature of cryoglobulinemic vasculitis.
“Another notable takeaway is the need to repeat testing if your suspicion is high,” Dr. Lally says. “In this cohort, 9% of patients had initial negative testing and then a positive [cryoglobulin test] on repeat testing. This speaks to high false-negative rates.”
Yet another take-home message, according to Dr. Lally: “We often associate rheumatoid factor positive with mixed cryoglobulinemia, but in this population, only 20% of patients with mixed cryoglobulins had a detectable serum rheumatoid factor, and most of these were patients with hepatitis B or C rather than autoimmune disease,” she says.
What’s Next
Researchers plan to next focus on the link between cryoglobulins and hepatitis C infection, says Dr. Miossec, noting physicians look for a hepatitis C infection only in 30% of cases when cryoglobulin is detected. They also will continue ongoing research into the limitations of detecting rheumatoid factor in type II and type III cryoglobulinemic vasculitis.
Vanessa Caceres is a medical writer in Bradenton, Fla.
How to Transport Blood Samples for Cryoglobulins
Nurses and technicians must receive training in the proper way to transport and handle blood samples intended for cryoglobulin testing.1 Proper sampling, transport and care are critical to lower the chances of a false negative test result. Here are a few tips to follow:
- Use preheated tubes during blood collection;
- The sample tube should be carried to the lab in a container that maintains a temperature of 37°C.1,2 This is particularly important for the detection of type I cryoglobulins;
- A preheated centrifuge creates the best conditions for the detection of cryoglobulins at low concentrations; and3
- Allow the serum to cryoprecipitate at 4°C for at least three, and preferably seven, days.3
References
- Kolopp-Sarda MN, Nombel A, Miossec P. Cryoglobulins today: Detection and immunological characteristics of 1,675 positive samples from 13,439 patients obtained over six years. Arthritis Rheum. 2019 Nov;71(11):1904–1912.
- Kolopp-Sarda M-N, Miossec P. Cryoglobulins: An update on detection, mechanisms, and clinical contribution. Autoimmunity Reviews. 2018 May;17(5):457–464.
- Vermeersch P, Gijbels K, Mariën G, et al. A critical appraisal of current practice in the detection, analysis, and reporting of cryoglobulins. Clin Chem. 2008 Jan;54(1):39–43.