 The Lupus Initiative (TLI) has been an emergent creation inside the American College of Rheumatology (ACR) for the past six years. In 2009, the Office of Minority Health and Office of Women’s Health (now called the Office of Health Disparities) solicited an application from the ACR to develop resources for educating non-rheumatologists, both in training and in practice, to recognize the signs and symptoms of lupus and make appropriate referrals. The ACR created TLI to carry out this task, which it has done under the guidance of a national consortium of lupus and health disparities experts from academia, research, clinical practice and patient services.
The Lupus Initiative (TLI) has been an emergent creation inside the American College of Rheumatology (ACR) for the past six years. In 2009, the Office of Minority Health and Office of Women’s Health (now called the Office of Health Disparities) solicited an application from the ACR to develop resources for educating non-rheumatologists, both in training and in practice, to recognize the signs and symptoms of lupus and make appropriate referrals. The ACR created TLI to carry out this task, which it has done under the guidance of a national consortium of lupus and health disparities experts from academia, research, clinical practice and patient services.
What began as a one-year grant to develop educational resources aimed at eliminating racial-, ethnic- and gender-related health disparities in the diagnosis and treatment of lupus, has evolved to become a robust platform to disseminate lupus-related research and training. These projects, led by our members and a national network of lupus experts, have produced resources that are now used nationally in medical schools, other health professions schools, hospitals and private practices.
Six years later, TLI has evolved into Collaborative Initiatives, whose goal is to leverage the models, programs and partnerships developed for educating non-rheumatologists about lupus to the benefit of our members. These resources are available to all rheumatologists and health professionals and currently include multiple CME/CE activities, PowerPoint presentations, case studies (both traditional and interactive), a video reference library, lectures and more. Further, TLI is developing six new interactive cases for students and trainees. TLI’s expanding portfolio of resources can help you, as a medical professional, foster a deeper dialogue with your patients about their care.
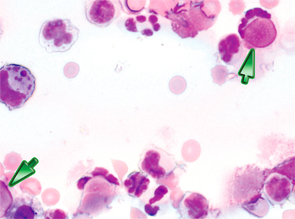
Lupus erythematosus cells.
Image Credit: vetpathologist/shutterstock.com
National Attention
A foundational impetus for the growth of this initiative is the increased national attention on health disparities and treatment of chronic diseases. It is well known that lupus disproportionately affects women and minorities, and recent studies show lupus could be the most common chronic disease among African American women and that another minority, American Indians/Alaska Natives, could have the highest lupus-related mortality rates.1,2 Because of the success of TLI, the National Association of Chronic Disease Directors (NACDD) and the Lupus Foundation of America selected the ACR to be a contributor to the National Public Health Agenda for Lupus, set for release in September 2015.
This agenda is the product of collaboration among more than 45 representatives from public health, physicians, national lupus associations, health insurers and persons with lupus. It will provide a “comprehensive public health approach to address lupus, which can supplement complementary efforts in lupus biomedical research and clinical care.”3
Moreover, the Department of Defense has included lupus as one of only 50 disease areas in its $278.7 million Senate appropriations bill that will fund the 2016 Peer Reviewed Medical Research Program. These new dollars will support scientists working to improve the treatment for lupus. Further, the Centers for Disease Control and Prevention (CDC) and the National Institutes of Health (NIH) have each issued requests for grant proposals centered on health disparities and lupus. Both agencies expect applicants to have strong, robust collaborations crossing multiple sectors (e.g., academia, research, health professionals, public health and patient services). The ACR is well positioned to respond to this funding opportunity because of TLI’s previous accomplishments, including the current projects:
- The Lupus Initiative’s Fellows Project, a focused pilot project in which rheumatology fellows in four focus cities have been educated to teach an estimated 600 frontline physicians and health professionals to recognize the signs and symptoms of lupus and its associated comorbidities. This project aims to enhance the ability of non-rheumatologists to recognize lupus and communicate better with their patients, as well as make appropriate referrals to rheumatologists. We expect this program will also translate into stronger bonds between physicians and the community as the level of knowledge about lupus increases, misinformation decreases and more timely diagnoses lead to earlier treatment. To date, approximately 400 health professionals have been educated through this program. Although we have not yet assessed the results of this project, a preliminary survey has shown that following this course, 93% of providers were more confident in recognizing the signs and symptoms of lupus, 94% gained knowledge about when to consider the diagnosis of lupus, and 90% were more secure about when to refer.
- Another TLI project, the Professional Outreach Project, provides lupus education to diverse health professionals via live continuing education sessions and a real-time tele-lecture series. To date, 266 providers have been reached through medical conferences and tele-lectures, with an additional three live medical conference sessions and one virtual education session yet to be completed. This activity is another avenue for providing largely non-rheumatologists with information about lupus and lupus-related health disparities in a way that can increase quality of patient care across the medical disciplines. Although the final analysis is yet to be done, preliminary data indicate 97% of provider respondents experienced a positive change in awareness about the severity, symptoms and prevalence of lupus. Ninety-one percent reported positive self-efficacy and intention change, which in this case means that a health professional will be more likely to act on what they’ve learned about lupus.
- The Lupus Initiative’s Expert Outreach Project supports the creation of an online lupus-specific education module to provide credit toward maintenance of rheumatology board certification (CARE: Lupus). This is available to our members and others at no cost and will provide 10 MOC credits.
Member support and involvement are vital, and many ACR members have been integral in both the development and execution of TLI projects. Notably, S. Sam Lim, MD, MPH, associate professor of medicine at Emory University School of Medicine in Atlanta, is chair of the TLI Consortium and principal investigator of the Georgia Lupus Registry and has served an important leadership role.
Also, from TLI’s Emory University partnership, Karen Law, MD, is developing a curriculum for multiple online, interactive case studies, and Cristina Drenkard, MD, has provided cultural competency expertise.
Elizabeth Ferucci, MD, MPH (Alaska Native Medical Center, Anchorage), has led multiple online professional outreach sessions and is the principal investigator for the Indian Health Services Lupus Registry; Ben Smith, PA-C (Tallahassee, Fla.), and Kori Dewing, DNP, ARNP (Virginia Mason Medical Center, Seattle), have led live professional outreach sessions at medical conferences for physician assistants and nurse practitioners.
The leaders of the Fellows Project include Amanda Sammut, MD (New York); Amy Caron, MPH (New York); Diane Gross, MPH (New York); Rosalind Ramsey-Goldman, MD (Chicago); and Maria Dall’Era, MD (San Francisco).
Other members instrumental to the success of these projects over the past year have been Megan Clowse, MD, MPH (Durham, N.C.); Greg Dennis, MD (Potomac, Md.); Mary Anne Dooley, MD, MPH (UNC Chapel Hill, N.C.); Candace Feldman, MD, MPH (Brigham and Women’s Hospital, Boston); and Ed Treadwell, MD (East Carolina University School of Medicine, Greenville, N.C.).
The Future
Data from national lupus registries, the research from advocacy and research groups, and the results of TLI’s own efforts suggest lupus may affect more Americans than previously thought. Through TLI and Collaborative Initiatives, the ACR is increasing its impact, expanding its reach and broadening its collaborations in lupus, keeping it ahead of the curve in the national conversation about lupus, chronic diseases and health disparities. Continuing to expand the work of the Collaborative Initiatives beyond lupus will allow the ACR to advance the care of other chronic rheumatic diseases and be at the leading edge of healthcare. Educated providers plus well-informed patients promises to enrich our specialty and its clinical practice, which is my reason for headlining this effort.
More information about The Lupus Initiative.
 E. William St.Clair, MD, is president of the ACR and chief of the Duke Division of Rheumatology and Immunology, Durham, N.C. Dr. St.Clair, a rheumatologist, has 25 years of experience as a clinical investigator. Contact him at [email protected].
E. William St.Clair, MD, is president of the ACR and chief of the Duke Division of Rheumatology and Immunology, Durham, N.C. Dr. St.Clair, a rheumatologist, has 25 years of experience as a clinical investigator. Contact him at [email protected].
References
- Lim SS, Bayakly AR, Helmick CG, et al. The incidence and prevalence of systemic lupus erythematosus, 2002–2004: The Georgia Lupus Registry. Arthritis Rheum. 2014 Feb;66(2):357–368.
- Somers EC, Marder W, Cagnoli P, et al. Population-based incidence and prevalence of systemic lupus erythematosus: The Michigan Lupus Epidemiology and Surveillance Program. Arthritis Rheum. 2014 Feb;66(2):369–378.
- National Association of Chronic Disease Directors. National Public Health Agenda for Lupus. 2015 Apr 6.
