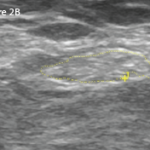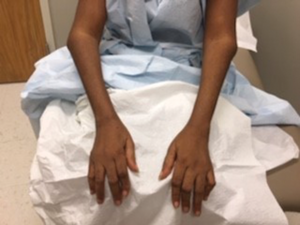
Figure A. Flexion contractures of bilateral elbows, as well as Boutonniere and swan neck deformities of the fingers in a patient with 25 years of untreated seropositive rheumatoid arthritis
Through the development of a multidisciplinary musculoskeletal institute, we have created a model that facilitates coordination of care of complex patients between medical and surgical subspecialists, physical therapists, dieticians and social workers. A case is presented to demonstrate the improved care experience for both patients and providers and to share our learnings more broadly.
The Case
Ms. K. sat in a wheelchair, wearing a large straw hat with a sunflower pasted to the brim and a smile the same size. Her daughter sat by her side, seven months pregnant. I introduced myself and shook her hand, taking care not to squeeze too tightly. As she told me about herself, I observed. Flexion contractures of both elbows, and Boutonnière and swan neck deformities of several fingers were present (see Figure A). She had profound bony hypertrophy of the knee joints with flexion contractures (see Figure B). I searched for a cane propped up in a corner but did not find one.
Ms. K. was 54 years old. She moved to Texas from Liberia to live with her daughter. Joint pain and swelling had developed 25 years earlier. Her symptoms were attributed to sickle cell trait, and pain was managed with non-steroidal anti-inflammatory drugs as needed. When she arrived in Austin, she qualifirf for the Medical Access Program, a local health coverage program that helps uninsured, low-income residents gain access to select health services. She was diagnosed with seropositive rheumatoid arthritis by her new primary care provider and referred to our rheumatology clinic.
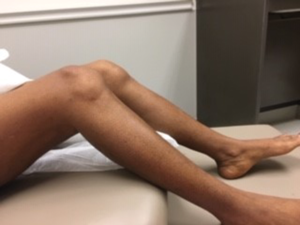
Figure B. Bilateral knee contractures with bony hypertrophy, rendering the patient unable to extend her legs past 45º.
“How long have you been using that wheelchair?” I asked.
“About one-and-a-half years.”
“Why did you start using it?”
“My knees … they don’t go straight. It hurts to stand.”
“Are you able to stand on your own, or walk at all?”
“I can stand up with some help. I can walk a couple steps. But then I have to stop. The pain is just too much.”
She was able to laterally transfer herself to the exam table without assistance. Knees were contracted by 45º bilaterally. Audible crepitus and synovitis were present. Quadriceps strength was normal with minimal muscle atrophy.
We chatted about rheumatoid arthritis, medical therapies and treatment goals. She had never seen an orthopedic surgeon before, but would be interested in joint replacement surgery if I thought it would help. “I’ll find out,” I said.
That afternoon, I emailed my new surgical colleague, Karl Koenig, MD. I had just accepted a position as the first rheumatologist in the Musculoskeletal Institute at UT Health Austin, becoming part of a multidisciplinary team comprising several integrated practice units dedicated to different musculoskeletal conditions. I gave him a quick rundown: