


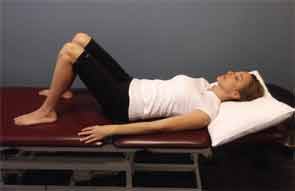
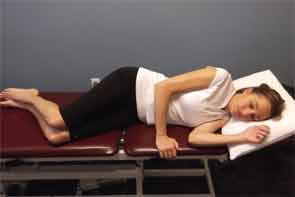
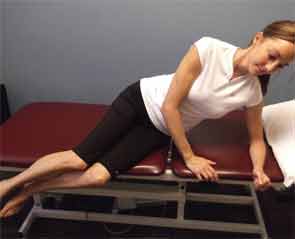
Patients with rheumatic diseases are no strangers to pain. Because back pain is highly prevalent worldwide—and higher yet among patients with rheumatoid arthritis (RA), ankylosing spondylitis (AS), and fibromyalgia—rheumatologists may need to have a few tips and tricks for preventing and alleviating back pain on hand. A tailored exercise program that helps improve mobility, strength, and function can be beneficial for the rheumatic patient with back or neck pain. Rheumatologists and rheumatology health professionals can help these patients by offering tips on posture, general health, and functional activities, as well as referring them for physical therapy. Through a multidisciplinary approach, patients who have rheumatic disease and present with back or neck pain can find relief.
Prevalence
The average point prevalence of low back pain worldwide is about 12%, and it is highly recurrent after the first episode.1 It is also more common in those between 40 and 80 years of age, as well as in women.1 Additional research shows that low back pain incidence is highest in the third decade of life, and overall prevalence increases with age until between 60 and 65, then gradually declines.2 In the United States, approximately 27% of adults have low back pain and about 14% have neck pain.3
In practice, patients of all ages, genders, and ethnicities present with back pain. “Back pain occurs along the spectrum, the continuum of life, if you will,” says Jan K. Richardson, PT, PhD, OCS, professor emeritus at the School of Medicine, Duke University Medical Center in Durham, N.C., and chief medical officer at Priority Care Solutions, Inc., in Tampa, Fla. “It’s not uncommon for adolescents as they’re moving into their teens and having these very fast growth spurts to develop back pain. … Then there seems to be a lull and the next group is the working group, those who are employed. There’s a high prevalence of back pain in the second, third, and fourth decade of the working population, especially in the demographic group who either has very active and labor-types of jobs and those who are very sedate and do a large amount of sitting.”
You’d want to try a conservative course of pharmacology and nonpharmacology treatments, including physical therapy, and exhaust those possibilities and interventions before you refer [the patient] on to a surgeon.
—Jan K. Richardson, PT, PhD, OCS
Risk Factors
In addition to job type, risk factors for low back pain include low educational status, stress, anxiety, depression, job dissatisfaction, and low levels of social support in the workplace.2 Psychiatric disorders frequently appear in patients with nonspecific back pain.4



