MADRID—Scores on the Health Assessment Questionnaire for Rheumatoid Arthritis (HAQ) and C-reactive protein (CRP) levels were independent predictors of whether patients could be tapered successfully from a TNF inhibitor after having reached remission of their RA, according to findings presented in a session at the Annual European Congress of Rheumatology.
Researchers also developed a composite index of several factors they say could help predict successful tapering.
It was one of two studies that highlighted the potential to withdraw certain patients from therapy in a session that also included a comparison of the effectiveness of anti-TNF drugs after a year of use.
In the Spacing of TNF-Blocker Injections in Rheumatoid Arthritis Study (STRASS), 137 patients in sustained remission with a DAS28 of less than 2.6 for at least six months were randomized to keep taking their TNF inhibitor at their full dose or to space their injections gradually until they were discontinued, said Thao Pham, MD, PhD, professor of rheumatology at Saint Marguerite Hospital in Marseille, France.1 Successful tapering was reached when patients were able to whittle to 25% of their regimen.
Two variables differed between those for whom TNFi tapering was successful and for whom it wasn’t. Patients with success had an HAQ of 0.3, compared with 0.89 (P=.01), and the successes had a CRP reading of 2.35 mg/L, compared with 3.48 mg/L (P=.02).
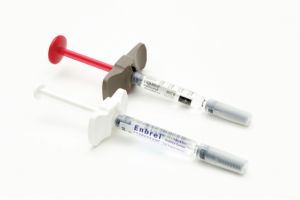
More studies are needed to accurately identify patients who can safely be taptered off TNF inhibitors, such as etanercept and adalimumab.
Martin Shields / Science Source
Researchers found that an HAQ threshold of at least 1.125 predicted a successful tapering with a specificity of 93% and an area under the curve (AUC) of 0.713 (confidence interval [CI]: 0.54–0.87). A CRP threshold of at least 6.8 mg/L had a specificity of 0.97 and an AUC of 0.689 (CI: 0.55–0.83). Dr. Pham acknowledged that these AUCs were “not satisfying.”
A composite that includes anti-citrullinated protein antibody (ACPA) status, Simplified Disease Activity Index (SDAI) scores, CRP and HAQ also may be predictive, researchers said. They found a score threshold that predicted successful tapering, with a specificity of 100%, a sensitivity of 54% and an AUC of 0.829 (CI: 0.67–0.99).
“A validation study will be need to confirm its ability to select patients for treatment decrease,” Dr. Pham said.
Withdrawing DMARD Therapy
In interim results from another study examining the possibility of reducing therapy, Canadian researchers found that withdrawing certain patients from non-biologic disease-modifying anti-rheumatic drug (nbDMARD) therapy yielded responses that were just as good as those who continued on both those DMARDs and certolizumab pegol.2