(click for larger image)
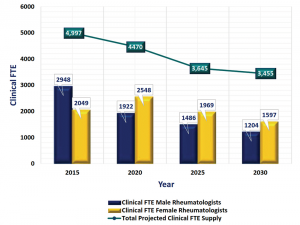
Figure 1: Projected Decline of U.S. Rheumatologists
Source: 2016 ACR/ARHP Annual Meeting, Abstract 89,
Figures: Seetha Monrad
Ten years have elapsed since the ACR conducted its last workforce study, and we know that much has changed. The comprehensive patient-centered, integrative approach to the 2015 ACR/ARHP Workforce Study of Rheumatology Specialists in the United States (now publicly available) describes the character and composition of the current clinical workforce, recognizes demographic and employment trends, informs workforce and succession planning for the ACR/ARHP, and projects future supply and demand estimates based on best- and worst-case scenarios.
When you review the study results, you’ll find that although the broad trends are akin to the findings of the 2005 ACR Workforce Study, the size of the gap between rheumatology provider supply and patient demands is much wider than expected.
The Results in Brief
In fact, the 2015 Workforce Study paints a startling picture of the rheumatology workforce in the next 10 years. It projects a shortage of 3,845 rheumatologists in the U.S. by 2025, an increase from the 2005 ACR Workforce Study, which projected a shortage of 2,576 rheumatologists. A declining rheumatology workforce resulting from significant baby boomer retirements (among both patients and rheumatologists), millennial ascendency and a gender shift toward women will be met with an increasing patient demand.
(click for larger image)
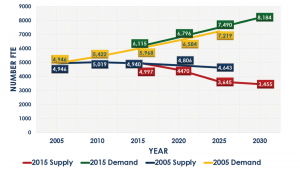
Figure 2: Demand Outstrips Supply
Source: 2016 ACR/ARHP Annual Meeting, Abstract 93
Figures: Seetha Monrad
We also anticipate a significant increase in the prevalence of doctor-diagnosed arthritis in the next 20–25 years. By 2030, an estimated 67 million adults (25% of the projected total adult population) aged 18 years and older will have doctor-diagnosed arthritis. This aging population is anticipated to increase the number of adults suffering from osteoarthritis, and other age-related conditions will be a contributor to an increased demand for rheumatologists over the coming decades.
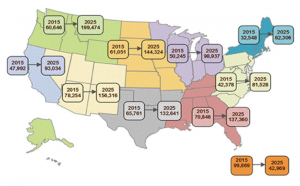
Unfortunately, a regional maldistribution of rheumatologists in the U.S. exists, and disparities will continue to increase with anticipated retirements and regional population growth estimates, particularly in the South Central, North Central and Northwest regions. The estimated total number of adult rheumatologists in the U.S. workforce in 2015 by full-time equivalent (FTE) is 4,997, with a projected decrease to 3,645 by 2025 (see Figures 1 & 2). The overall adult-to-physician ratio is projected to be 99,177 by 2025 (see Figure 3).
Challenges Ahead
(click for larger image)
Figure 3: Projected Increase in the Number of People per Rheumatologist (2015–2025)
Source: 2016 ACR/ARHP Annual Meeting, Abstract 928
New data collected solely from pediatric and adult fellows in training shed light on new challenges facing the future of rheumatology in the U.S.
Rheumatology fellowships are attracting more international medical school graduates (53%), with 11% osteopathic and 36% from U.S. schools accredited by the Liaison Committee on Medical Education. Seventeen percent of international medical school graduates plan to work abroad, further contributing to the potential shortages of rheumatologists in the future. Of the fellows in training, 18.3% indicated they would work part time, and the great majority (90%) of those who gave that response were women.
By 2030, millennial women are projected to make up 59% of the rheumatology workforce. Why does this matter? Because women physicians tend to work seven fewer hours every week and on average treat 30% fewer patients than their male counterparts, according to the 2015 State Physician Workforce Data Book published by the Centers for Workforce Studies. Since 2005, there has been a 5% decrease in patient load per week for all millennial physicians. Physicians seeing fewer patients will have significant implications for the rheumatology workforce.
Based on these results, the ACR recognizes that the next decade holds some formidable challenges for rheumatology:
- Recruitment for the rheumatology workforce needs to be ramped up;
- The declining number of rheumatologists will make it challenging to provide adequate access to, and reduce barriers to, care for rheumatology patients; and
- The existing workforce will need greater support to meet patient needs.
The challenges in recruitment of clinical and academic rheumatologists include substantial student debt, unfilled fellowship positions and competing specialties.
Potential Solutions
The study also highlights opportunities to increase the number of future rheumatologists, such as by recruiting under-represented minorities; increasing rheumatology exposure in medical school and residency; offering incentives, such as loan repayment programs and innovative mechanisms for GME funding; and increasing the use of nurse practitioners and physician assistants in the management of common musculoskeletal conditions in clinical practice.
Now is the time to develop novel strategies, processes and a multidisciplinary approach to ensure timely access to care for our rheumatology patients.
Where We Go From Here
At the 2016 ACR/ARHP Annual Meeting in Washington, D.C., 11 workforce study-related abstracts (six posters, four oral and one plenary session) were presented. Daniel F. Battafarano, DO, MACP, FACR, San Antonio Military Medical Center, workforce study co-chair and speaker in the session, The Rheumatology Workforce: Present and Future, presented the findings of the current workforce from retirements to gender shifts, regional distributions, academic rheumatology, use of telehealth and musculoskeletal ultrasound and the impact of social media in practice. In the second half of the session, a panel of workforce experts in the areas of academic rheumatology, adult private practice, pediatrics, regional differences, role of mid-level provider and diversity delved into an open discussion in defining strategies to solve the issues raised by the workforce study.
The ACR will use the findings and recommendations from the workforce study, coupled with a tactical plan designed by the ACR Committee on Rheumatology Training and Workforce Issues, to inform its next strategic plan for meeting the academic and non-academic rheumatology supply and demand needs.
On behalf of the ACR, I’d like to thank the 2015 Workforce Study Group, subgroup of the ACR Committee on Rheumatology Training and Workforce Issues, co-chaired by Dr. Battafarano and Seetha Monrad, MD, from the University of Michigan at Ann Arbor, who invested countless hours to oversee this study through completion.
 Sharad Lakhanpal, MBBS, MD, is in private practice at Rheumatology Associates and a clinical professor of internal medicine at the University of Texas Southwestern Medical School, both in Dallas, where he has lived and worked since 1986. He is also the 80th president of the ACR (2016–17).
Sharad Lakhanpal, MBBS, MD, is in private practice at Rheumatology Associates and a clinical professor of internal medicine at the University of Texas Southwestern Medical School, both in Dallas, where he has lived and worked since 1986. He is also the 80th president of the ACR (2016–17).
Note: The ACR contracted the Academy for Academic Leadership (AAL), a leading firm in the area of workforce projection, to conduct the Rheumatology Workforce Study.


