
Sports fans find enormous pleasure in arguing about topics such as the greatest player in baseball, the best heavyweight boxer, or the worst draft pick in the NFL. Most of these arguments cannot be resolved and ultimately do not matter. Nevertheless, the diehards joust with vehemence and passion, especially if fueled by some alcoholic brew.
I enjoy such arguments myself—Was Mantle better than Mays?—but, instead of such traditional subjects for debate, I would like to focus on a serious subject. Which body parts does football damage more? Bones and joints or the brain?
In other words, is the arthritis inflicted by football worse than the dementia?
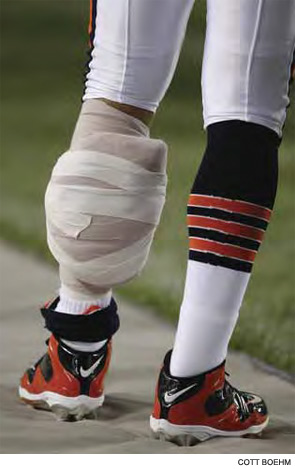
Measuring Destruction
Admittedly, the question is difficult, but it is serious and real. In actual healthcare, judgments about eventualities require valuation of the number of events, their severity, the extent of disability, and quality-adjusted life-years (QALYs). A person who can’t think or can’t walk has lost quality of life. It is a philosophical question whether a person who sits in a wheelchair wracked with pain has a lower quality of life than a person who drools while looking blankly at the members of his family whose names he cannot remember—but football can lead to both miserable outcomes.
In the past few years, the impact of football on players’ health has received extensive attention, propelled from the sports section to the front page, including the cover of Time magazine. The situation shouldn’t be a surprise. Turn on any game and you can witness horrific collisions, the size and speed of pro athletes leading to forces that match those of a bomb explosion. This brutal, smash-mouth game harms brains in terrible ways. While boxers are known to get punch drunk, the fact that football players can suffer the same fate has been treated as a major revelation.
There is growing acceptance that big hits that ring a player’s bell or cause cobwebs to accumulate are often really concussions and that, over time, traumatic brain injury can lead to dementia. In boxing, this condition is called dementia pugilistica or chronic traumatic encephalopathy. For pro football players, the increase in dementia can be 20 times that of the general population depending on the age group. About 6% of ex-players age 50 or older develop a form of dementia that can resemble Alzheimer’s disease.
The life expectancy of a pro football player is not that great anyway, but dementia is more shocking to the public sensibility than premature mortality. Sadly, the heroics on the gridiron that are supposed to lead to fame, fortune, and beautiful women have a big price—trouble finding words, forgetfulness, and incontinence that can develop just a few years after an athlete has hung up his cleats.
Concern for Heads, But Not Knees
It took some time before the toll of football on the brain became apparent. In general, the studies from the medical literature indicated that the risks of serious head injury were relatively low and that most of those who suffered a concussion had limited short-term problems. In contrast, the personal experience of the family members of pro athletes made the connection between football and dementia clear. Indeed, the wives of the players—not the players themselves—helped sound the alarm, the maimed men too ashamed to reveal their infirmities.
For its part, the NFL has taken heat for its attitude, with accusations that it, like the tobacco industry denying a link between smoking and cancer, supported bogus science to hide the role of football in permanent brain damage. Recently, the NFL has been more forthcoming about brain injury inflicted on the field and has even agreed to support scientific studies, pledging $1 million to a research center in Boston.
Congress has also gotten into the act and attitudes are changing. The league is creating new rules concerning the time interval between a concussion and a return to play and an acceptable amount of cerebral bell ringing before an athlete has to retire. New helmet designs are on the drawing board. I am not sanguine that such maneuvers will really protect the head from the mayhem, but something is better than nothing.
Leading the charge in this reform movement has been a brave group of outspoken neurologists and neuropathologists for whom a connection between a career in football and dementia later in life is, to make a terrible pun, a no-brainer. These physicians saw unequivocal clinical and pathological evidence of brain damage and acted smartly and decisively.
What is the chance of developing arthritis that would make me have a heart-to-heart talk with the athlete and tell him it’s time to say no?
When it comes to musculoskeletal injury resulting from sports, however, the medical profession has at best an ambivalent attitude even if the connection with eventual arthritis is so abundantly clear. There is simply no question that playing football at any level virtually guarantees a serious injury to joint, muscle, or bone. Fractures, dislocations, and joint blowouts mark just about every career, and many of these injuries culminate in severe lifelong arthritis.
The most common form of injury-related arthritis is osteoarthritis (OA) or degenerative joint disease. While common in the older population, arthritis is not inevitable. Its frequency in the elderly should not minimize its significance when it strikes decades earlier than expected.
Watch any gathering of former athletes at a pregame or half-time celebration to honor old-timers. These former hulks limp, shuffle, or get pushed around in wheelchairs because of the sorry state of their joints. If there were X-rays of the limbs of these former players, the joints would look either crushed or shine brightly with titanium replacements. Indeed, degenerative arthritis is three to five times more common in pro football players than men of the same age, with the impact greatest on men younger than age 60.
Every day, on the sports page, along with the box scores, an injury report will appear because of its effect on the outcomes of upcoming games. So common are these injuries that the only interest they seem to engender is the effect on the betting point spread, the team’s win–loss record, or the prospects for playoffs. The influence on the athlete’s health or well-being receives scarcely a mention.
“If it doesn’t hurt, it doesn’t help.” Growing up playing sports, I heard that statement hundreds of times but it is filled with fallacy bordering on the criminal. When it comes to bones and joints, the reality should be “If it hurts, it won’t help,” or better, “If it hurts, it harms.”
Pain is the body’s warning system and was designed by Mother Nature to alarm the body of danger. By making a damaged part uncomfortable or unpleasant to move or use, nociceptive pain prevents further injury and allows healing. Nature exacts its price with pain, but the system is wise and works. Ignoring pain to an injured muscle or joint is risky and dangerous.

Modern Medical Marvels
Recently, I attended a medical conference on the worldwide burden of musculoskeletal disease, especially from joint trauma. During the presentations, I was struck by the frequency in which the trauma depicted was an athletic event. Since this was an international meeting, the most dramatic pictures featured soccer players engaged in vicious tackles. The scenes looked dreadful and, no doubt, a meniscus or anterior cruciate ligament (ACL) would disintegrate or pop under the hit. The speakers’ message was clear. After a few years, arthritis would strike those engaged in sports combat.
Most of the speakers at the conference were orthopedic surgeons and, when it comes to reconstructive surgery, these physicians are miracle workers. While, in the past, all the king’s horses and all the king’s men couldn’t do the job, if Humpty Dumpty were alive today, these surgeons could put him back together, toiling in the glare of the operating room lights, patching cracks in Humpty’s shell with some nifty adhesive, popping in a custom-made prosthesis to complete the jigsaw puzzle of the broken exterior.
Too often, in sports medicine, the perspective seems to be the next game or the next season and not the long-term health of the athlete. Indeed, in some trials on reconstructive surgery of the joint, the outcome of success for the intervention is the time until return to sports. Orthopedists and athletes are very much allied, especially since many orthopedists are former athletes and they believe in the ethos of sports. Knowing personally what a game can mean to an athlete, they share the desire for a return to the field. As long as the athlete can suit up to play, many sports medicine physicians seem willing to condone an athlete’s return into battle even if it is risky and can lead to further injury.
Countless football players who have had major joint surgery have returned to the game almost as swift, elusive, and powerful as before their operation. Drew Brees is a recent example, with his shoulder remarkably restored. With the advent of arthroscopic surgery, a player can again play a few weeks after a nip or tuck in the meniscus or loose pieces of cartilage are extracted with the scope. Certainly, many football players have their knees drained of fluid before games or injected with lidocaine or steroids, quick fixes where there is no time for a trip to the operating room during the press of the season.
Of course, with the athlete fixed, temporarily or permanently, he is allowed to return to the exact same activity that caused harm in the first place. Once damaged and out of alignment, a surgically repaired joint is likely to break down under the stress of twisting and pivoting. Repeat injury is common.
While a surgeon can restore the body, should he tell Humpty to climb back on the wall or stay safely on the ground?
During the question-and-answer period at the meeting, I asked one of the speakers, a noted sports medicine expert, why the attitude to musculoskeletal injury in sports differs from that of brain injury. Why, I asked, shouldn’t physicians advocate for new rules, regulations, and even legislation to reduce devastating and debilitating bone and joint injury from football? “Isn’t arthritis serious enough to merit prevention?” I asked.
The surgeon looked surprised by my question because it is contrary to much of sports medicine, the goal of which is to return the athlete quickly to competition. The surgeon replied that the situation with bone and joint injury is different than that of brain injury. Indeed, he said, with strength training, conditioning, pads, and braces, the magnitude of sports-related injury could be reduced.
The orthopedists have their bases covered. If an ounce of prevention does not work, the operating room can provide a pound of cure so that, after going under the knife, the athlete can be as almost as good as new. If I were a surgeon, I would be very proud that a person on whom I operated could again toss a fast ball at 100 miles an hour, smash an overhead, or rocket a 70-yard pass down the field in a perfect spiral.
On the other hand, how would I feel if I knew that a return to sports would increase the likelihood of serious debilitating arthritis in my patient five- or 10-fold and that the eventual outcome would be permanent disability? Would I still recommend or even allow a return to sports? What is the chance of developing arthritis that would make me have a heart-to-heart talk with the athlete and tell him it’s time to say no?

Sports Injuries Exact a Long-Term Toll
Physicians do not like to be scolds, moralists, or spoilsports but, in the case of musculoskeletal injury, the times call for spoilsports. Consider the data. The chance of serious injury in soccer is 1,000 times greater than a high-risk occupation like mining. Remember, mining has special safety programs because of the hazards deep beneath the ground but those risks are a trifling compared to an afternoon on the pitch.
Following a meniscal tear, the chance of OA jumps dramatically, with over 50% of people suffering symptoms and having X-ray evidence in 10 to 20 years. Unfortunately, many people with a meniscal tear will damage other joint structures at the same time. Experiments in animal models indicate dramatically the likelihood that these injuries will lead to arthritis because the standard models for OA involve the severing of an anterior cruciate ligament or removal of a meniscus from the knee of a rabbit or dog. Like clockwork, arthritis develops in the operated animals.
If the studies are to be believed, the increase in the frequency of arthritis from sports—especially among female athletes—will dwarf that attributable to the aging of the population. Indeed, sports have created a new entity—old knees in young people—as sports participation has transformed a problem of baby boomers into one of babies. For many people, OA starts with injury when they are young—on the field or behind the driving wheel. Injury is the real culprit in a process that may take 10, 20, or 30 years to culminate in a joint in which cartilage is eroded and tattered and pain accompanies every step. Once a joint is injured in a sport, the clock starts ticking on the time bomb called arthritis.
Once I attended the Blue–White scrimmage of the Duke football team during spring practice. Wallace Wade Stadium in Durham is usually not very full during the season, even when the contest is with the Tar Heels from down Tobacco Road, now called Highway 15-501. On a warm April day, the sky glistening Carolina blue, the stadium was virtually empty, allowing every sound to be appreciated in a way not possible when screaming fans attempt to discombobulate the opposing team with a sonic assault. The noises of collision at the scrimmage were crashing and visceral, making apparent the forces generated. What I remember most were the grunts and groans of pain during the charge of the lineman and the tackles of the backs. The sounds of pain were louder and more intense than any I have encountered in medical practice, whether from a patient with a kidney stone, dissecting aneurysm, or myocardial infarction.
I would assume that a torturer in a prison would relish such clamor but, for a physician, it was a shock, knowing how much pain accompanies the game. To me, every grunt or groan represents a potential injury that in a few years could cause a joint to degenerate or throb with pain with terrible life-long consequences.
Whenever I see a 30- or 40-year-old person with serious OA, one of the first questions I ask is “Did you play sports?” Almost always, the answer is yes.
In my practice, I see countless patients who attribute their pain directly and unequivocally to their participation in sports. Nevertheless, they keep at it, repetitively hurting themselves despite the prophylactic dose of ibuprofen, an arm brace, or running shoes with rubbers of four colors or densities to dissipate shock or prevent too much pronation.
“What can I do?” these patients asked plaintively about relieving their pain. “Stop. Take a rest,” I say, and they look at me in disbelief or pique, wondering how someone supposed to be an expert is just so plain dumb. They act as if my request for respite is tantamount to genetic rewiring or a sex-change operation.
Send Us a Letter!
Contact us at:
David Pisetsky, MD, PhD, physician editor
E-mail: [email protected]
Dawn Antoline, editor,
E-mail: [email protected]
Phone: (201) 748-7757
The Rheumatologist welcomes letters to the editor. Letters should be 500 words or less, and may be edited for length and style. Include your name, title, and organization, as well as a daytime phone number.
A Path to Victory?
As in the case of reducing neurological damage from football, I can see many ways to lessen the impact of football on bones and joints. To be fair, these strategies would need support from solid research, and I would encourage a major initiative to study the frequency of football-related arthritis and its long-term course, including the effects of surgery, either positive or negative. Research takes time but, to get started now, I would suggest some modest steps that seem eminently reasonable: independent assessment of player injury by impartial evaluators, not team physicians; limitations on the number of joint injections or surgical procedures in a player’s career; restriction on the use of pain killers, whether given systemically or injected in the joint, before the game; and increase in the time interval after surgery before a return to practice or playing.
At the high school level, I would add an education program on the dangers of sports just as I would educate young people about the hazards of smoking, unprotected sex, or driving under the influence of alcohol or drugs. Programs of education are enormously difficult to implement but, with the unquestioned dangers or participation in collision sports, young people and their families should be told honestly about the risks to make a more informed decision.
In medicine, decision making constantly balances risks and benefits, the knowns with unknowns. As a physician, my commitment is to prevent injury and damage and make sure that people live as long, happy, and pain-free a life as possible. Sadly, when it comes to football and other contact and collision sports, the risks can outnumber the benefits, the knowns of injury exceeding the unknowns of potentially other benefits. Like my colleagues who study the brain, I think that it is time to stop the carnage that football is inflicting on the bone and joints of its participants.
Coach Amundson, the coach at the helm of my high school’s football team, used to fill his pep talks with aphorisms like, “Only the game fish swim upstream,” or, “When the going gets tough, the tough get going.” One of my favorites was, “When the Great Scorer comes to mark against your name, he asks not whether you won or lost but how you played the game.”
Coach Amundson was old school in his attitudes and is long dead. While we all used to chuckle about his homespun philosophy, he taught important lessons in life. He was right about Judgment Day. I believe that, if the Great Scorer asks the medical profession how we are preventing the devastation of football injury, he would decide that, not only are we losing the game, but, sadly, we are playing it badly.
Dr. Pisetsky is physician editor of The Rheumatologist and professor of medicine and immunology at Duke University Medical Center in Durham, N.C.

