ibreakstock / shutterstock.com
SAN DIEGO—At the 2017 ACR/ARHP Annual Meeting this past November, three researchers discussed the latest ANCA-associated vasculitis (AAV) research, including studies on AAV pathogenesis, therapies and remission maintenance.
In the Philip Hench, MD, Memorial Lecture, J. Charles Jennette, MD, chair in pathology and laboratory medicine at the University of Carolina at Chapel Hill in Chapel Hill, N.C., said the pathogenesis of AAV involves a complex series of events that evolve over time, and the treatment approach is growing ever more sophisticated.
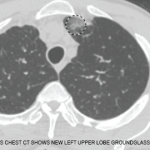
Dr. Jennette began studying the disease more than 30 years ago. In his talk, he traced his experience with the disease back to a 15-year-old patient he first encountered in 1985. The patient had severe arthritis, severe pulmonary hemorrhage, glomerulonephritis and purpuric rash. The patient did not fulfill diagnostic criteria for the types of glomerulonephritis and vasculitis that were known at the time. With no diagnosis and no known cause, a confident decision about treatment could not be made.
Dr. Jennette and his major collaborator, Ronald J. Falk, MD, chair of medicine at UNC, made important discoveries about the antigen specificity and disease associations of this new class of antibodies, which came to be known as anti-neutrophil-cytoplasmic autoantibodies (ANCA). Since then, the classification criteria for AAV has deepened, along with insights into its pathogenesis, now known to involve ANCA-induced activation of primed neutrophils resulting in acute inflammation and necrosis, and chronic inflammation and scarring.
Today, Dr. Jennette said, treatment strategies have been influenced by the understanding of AAV pathogenesis.
“B cell-directed immunosuppressive therapy must be accomplished to initiate remission and to sustain it in the long term,” he said. Therapy must also specifically interrupt the acute inflammatory “amplification loop” present in patients with active AAV, he said; that is, it must break the cycle in which the activation of neutrophils leads to activation of the alternative complement pathway, which leads to even more neutrophil activation.
Anti-macrophage and anti-T cell therapy must also be incorporated for the disease’s subacute phase, along with anti-fibrotics and immunomodulators, to sustain remission.
Treatment options continue to improve, Dr. Jennette said, with the introduction of novel therapies targeting specific components of the pathogenic process.
Promising results have been seen with CCX168 (i.e., avacopan, an oral inhibitor of complement component 5a (C5a) receptor), which disrupts the disease’s amplification loop and limits steroid use.1 In a randomized trial with 63 patients, the drug was found to be statistically non-inferior to standard treatment with steroids, with faster improvement of disease activity, according to the Birmingham Vasculitis Activity Score (BVAS). The drug is now in Phase 3 clinical trials. (Note: Dr. Jennette has received research support from the manufacturer, ChemoCentryx.)