Systemic autoinflammatory diseases (SAIDs) are rare syndromes characterized by alterations in innate immunity that result in a variety of clinical manifestations that are usually associated with recurrent fevers.1 Thanks to advances in genetic sequencing over the past few years, monogenic causes for some of these autoinflammatory diseases, such as Yao syndrome, have been discovered.2
Previously known as nucleotide-binding oligomerization domain 2 (NOD2) associated autoinflammatory disease, Yao syndrome is characterized by periodic fever, gastrointestinal manifestations, dermatitis, polyarthritis and sicca-like symptoms. The disease occurs sporadically in most patients, and a family history is seen in only a few.3
Because SAIDs are typically associated with a single genetic mutation, genetic panel testing usually reveals the presence of only one underlying, associated mutation. The presence of two genetic mutations associated with SAIDs is a rare occurrence and can result in the expression of just one of the mutations or a phenotypic fusion of the two.
Because these genes are often integral to innate immunity, it is possible to consider that certain interactions with pathogenic substances could spur the development of disease in predisposed individuals. This phenomenon has been reported in a patient with COVID-19.4
We report the case of a patient diagnosed with Yao syndrome who was discovered to have two genetic mutations associated with autoinflammatory disease, as well as a COVID-19 infection that may have contributed to her final clinical presentation.
Case Description
A 46-year-old woman of both Asian and Latin descent presented with a chief complaint of recurrent episodic fevers associated with abdominal pain and non-bloody diarrhea for the prior 12 years.
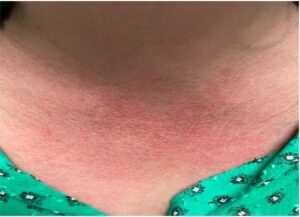
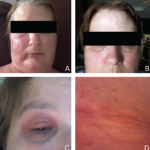
Initially these episodes lasted for several days and occurred infrequently, months to years apart. The abdominal pain was generalized with mild nausea and occasional vomiting during these episodes. Upon further questioning, the patient reported swelling along her hands, ankles and feet, with a concomitant rash and facial flushing during these episodes. The flushing was reported to be related to heat exposure, and the rash was described as non-pruritic, extending over her face and chest, and persisting up to several weeks at times.
The patient presented to our clinic only after the episodic nature of her symptoms appeared to transition into a more persistent pattern.
Apart from fatigue and mild sicca symptoms, a review of the patient’s systems was otherwise unremarkable. Pertinent negatives included lack of weight loss, night sweats, alopecia, ocular complaints, oral ulcers, parotid gland enlargement, cough, shortness of breath, chest pain, myalgias, muscle weakness or Raynaud’s phenomenon.