Presentation
A 26-year-old man with a history of acne vulgaris and hidradenitis suppurativa presented to our rheumatology clinic with persistent back pain and stiffness of three years’ duration. He described bilateral low back pain that was worse when he arose in the morning and at night when he was trying to sleep.
In a similar pattern to his back pain, he described right shoulder and neck pain. He described neck stiffness preventing him from being able to look over his shoulder when driving. He worked as a cashier and did not notice any worsening pain during his shifts. On his days off, when he was less active, he noticed worsening symptoms.
Physical therapy over the previous few months had not improved his pain or stiffness. Exercise, 800 mg of ibuprofen three times daily and heating pads provided only minimal relief. He did not notice any swollen joints, and a review of systems was otherwise negative. There was no family history of arthritis.
The patient was followed by a dermatologist for his severe acne, which involved his face, scalp, axilla and groin. He had been on isotretinoin (13-cis-retinoic acid) intermittently for the previous four years. His therapy was limited by generalized myalgias. The dose of isotretinoin varied from 20 mg to 60 mg daily, with a two-year pause from therapy due to myalgias and, because the patient was attempting to lose weight, the need to take the medication with a high-fat meal. Two years prior to presentation he completed a four-month course with a cumulative total dose of 8,880 mg. Most recently, his cumulative dose of isotretinoin reached a value of 19,760 mg (170 mg/kg) and was, therefore, discontinued.
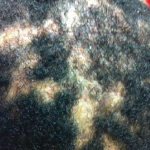
The physical exam was remarkable for a body mass index of 35, in addition to several skin and musculoskeletal findings. He had atrophic scarring of his face without papules, hypopigmented scaling lesions on his scalp, hyperpigmentation on the back of his neck and erythematous papules and scarring in both axillae. He had no nail abnormalities and no appreciable synovitis of his fingers, wrists, elbows, knees, ankles or toes. He exhibited reduced right shoulder external rotation due to pain. Bilateral hips exhibited reduced symmetrical external rotation; no back tenderness was elicited with active or passive hip movements. He did not have entheseal tenderness in his triceps, pectoris, quadriceps, patellar or Achilles tendons or plantar fasciae.
His axial mobility was markedly abnormal. The occiput to wall was approximately 8 cm (0 is normal). Tragus to wall distance measured 24 cm (less than 15 cm is normal). He had 0 cm excursion on the modified Schoeber test (greater than 5 is normal). Chest expansion only reached 3.5 cm (normal for his age and sex is 6.2–9.0 cm). Cervical spine flexion was preserved. He had decreased lateral flexion of cervical spine and slightly reduced cervical rotation. Lateral lumbar spine flexion reached 10 cm excursion on the left and 5 cm excursion on the right (greater than 10 cm is normal). Lumbar flexion was limited to 30º and he was unable to touch his toes. He did not have any sacroiliac joint tenderness.
The laboratory work-up revealed a normal complete blood count, liver function tests and hemoglobin A1C. The erythrocyte sedimentation rate (ESR) was mildly elevated to 29 mm/HR, with a previous available level of 18. His C-reactive protein (CRP) was 1.9 mg/L. He was negative for HLA-B27.