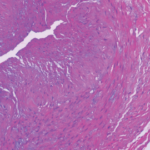
The autopsy showed significant internal hemorrhage, as well as aneurysmal dilatation of the aortic arch; aneurysmal dilation, medial dissection and intramural thrombus in the major branch of the celiac artery; transmural dissection of the superior mesenteric artery and dissection of the left common iliac artery. He was found to have a gene mutation in the COL3A1 gene consistent with Ehlers-Danlos syndrome (EDS) type IV, the vascular type.
Discussion
The subtypes of EDS were defined in the 1997 Villefrache classification, based on clinical features, mode of inheritance and genetic findings. The six major types, from most to least common, are:1
- Classical;
- Hypermobility;
- Vascular;
- Kyphoscoliosis;
- Arthrochalasia; and
- Dermatosporaxis.
In 2017, an updated EDS classification was proposed by the International Consortium on Ehlers-Danlos Syndromes & Related Disorders, which now recognizes 13 subtypes.2 The Beighton hypermobility scale can help assess for classic EDS, considering hypermobility of the peripheral joints and spine.
Vascular EDS is uncommon, with inheritance almost always in an autosomal dominant manner, although the exact incidence and prevalence remain unknown. The clinical diagnosis of vascular EDS is characterized by four clinical criteria: easy bruising, thin skin with visible veins, characteristic facial features and the rupture of arteries, uterus or intestines. Unfortunately, it is often only recognized after a catastrophic complication.1,3 The diagnosis can be confirmed by culture of fibroblasts, which synthesize abnormal type III procollagen molecules, or identifying a mutation in the gene for type III procollagen, COL3A1, by sequencing. The COL3A1 gene provides instructions for making a component of type III collagen, which is found in such tissues as the skin, lungs, intestinal walls and walls of blood vessels. The resultant arterial and tissue fragility is responsible for the often catastrophic complications. Midsize arteries are most commonly involved, and arterial rupture is the most common cause of sudden death. Spontaneous arterial rupture has a peak incidence in the third or fourth decade of life, but it may occur earlier.3
Although no treatment is known or currently available, physician unfamiliarity with the disease may compromise care and lead to loss of life. Patients with vascular EDS should avoid trauma, elective surgery, arteriography and colonoscopy. Also of note, intracranial aneurysms associated with vascular EDS should be considered in the differential diagnosis of cerebral vascular disorders and stroke in early childhood, and this may have been relevant given our patient’s family history.4
Vascular EDS is an uncommon, but important consideration, when one is evaluating a patient for diseases that affect the medium-caliber blood vessels (e.g., PAN), and SAM, a non-inflammatory arterial disease. Although systemic inflammation is generally seen in PAN but not SAM, both may have a similar appearance on an angiogram, with aneurysms, dissections, stenoses and occlusions. Histopathology is the gold standard for the diagnosis of SAM, which mainly affects intra-abdominal vasculature.5 Although a challenge, identifying vasculitis is particularly vital, because other vasculopathies discussed in this article won’t respond to treatment with corticosteroids and immunosuppressive agents.