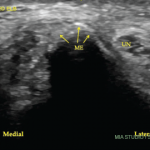
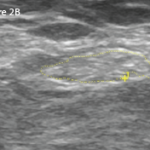
 Rheumatologists and neurologists are old friends. Practitioners of both fields have long shared a number of diagnoses, and referrals from one specialist to the other are frequent, such as for central nervous system (CNS) conditions, including giant cell arteritis, primary angiitis of the CNS, Call-Fleming syndrome, Susac’s syndrome and neuropsychiatric lupus. For the peripheral nervous system, shared spaces include evaluations of patients with mononeuritis multiplex or sensory neuropathy.
Rheumatologists and neurologists are old friends. Practitioners of both fields have long shared a number of diagnoses, and referrals from one specialist to the other are frequent, such as for central nervous system (CNS) conditions, including giant cell arteritis, primary angiitis of the CNS, Call-Fleming syndrome, Susac’s syndrome and neuropsychiatric lupus. For the peripheral nervous system, shared spaces include evaluations of patients with mononeuritis multiplex or sensory neuropathy.
Philip Seo, MD, MHS, director of Johns Hopkins University School of Medicine Rheumatology Fellowship, spoke with The Rheumatologist about what rheumatologists think neurologists should know to help strengthen the partnership between specialties.
He listed four areas of concerns. Rheumatologists must:
- Understand their limits. Sometimes a rheumatologist can treat only a portion of what’s happening to a patient with rheumatic disease;
- Realize how dependent rheumatologists are on the physical exam;
- Know that nerve conduction studies can be operator dependent; and
- Understand that neurologists and rheumatologists focus on atypical diseases. Communication is key.
“Rheumatologists generally rely on clinical assessment and try not to [request] tests when we feel that the yield [may] be low,” Dr. Seo says. “Neurologists sometimes cast a broad net, which may lead to equivocal tests that are difficult to interpret. As an example, an ANA [antinuclear antibody] test in a patient who presents with joint swelling and a malar rash is an incredibly useful test. An ANA test in a patient without the typical features of lupus may just be noise, because the test is positive in up to one-third of patients without a discernable autoimmune disease.”
Understand Your Limits
Dr. Seo says neurologists may be tempted to think that after a patient has an identified rheumatic condition, it’s smooth sailing for a rheumatologist to treat whatever problems arise. Nope.
“Often, there is a very thin slice of the patient’s problems that I can get under control with immunosuppression,” Dr. Seo says. “Many of the problems that bother the patient the most are a consequence of damage caused by previously active disease, which is no longer responsive to immunosuppression, the consequence of the drugs I use, such as steroid myopathy, or completely unrelated to the patient’s rheumatic disease, even though the patient may think that the problems are linked.”
Neurologists can help set a reasonable expectation about what their rheumatic brethren can achieve.
“My drugs can often halt the progress of a rheumatic disease, but [the treatments] can’t walk back damage that has already taken place [in the body], and they often take months to start working,” Dr. Seo says. “Patients sometimes come into my clinic with the idea that they have the autoimmune equivalent of a pneumonia. And it’s helpful if they realize that, regardless of the final diagnosis, treatment is generally a marathon, not a sprint.”