Review the case…
A. Lipodermatosclerosis
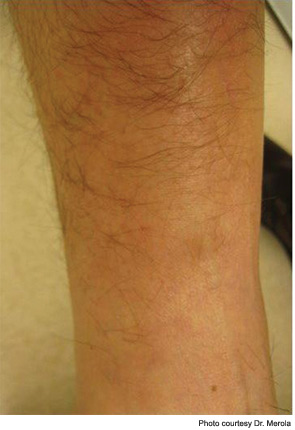
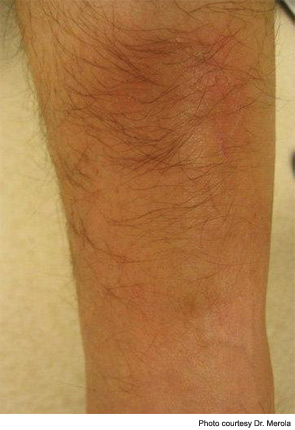
Historically, lipodermatosclerosis (LDS) was called “hypodermitis sclerodermiformis,” and terms such as pseudoscleroderma were used because of its indurated, hyperpigmented appearance, present on the distal lower extremity.1 Lipodermatosclerosis may best be described as a “sclerosing panniculitis,” found most commonly on the medial leg above just proximal to the medial malleolus. An acute and chronic phase occurs. Early, acute LDS may resemble a tender area of cellulitis or thrombophlebitis in the setting of lower extremity stasis, but its location, persistence, and indurated/ “bound-down” quality helps distinguish it from other entities. Chronic LDS is hyperpigmented, quite indurated and contracted, and may give the characteristic “inverted wine bottle” appearance. Ulceration is a complication and may occur in up to 13% of cases.2 It is generally a clinical diagnosis and caution should be taken if performing a biopsy confirmation because chronic nonhealing ulcerations may ensue. Doppler assessment of the lower-extremity venous system is often advised. The most conventional treatment involves regular use of compression stockings. Oral stanozolol, a testosterone derivative with fibrinolytic activity, has been shown superior to placebo in a small, double-blind, crossover trial and in an open trial by Dakovic et al for treating LDS.2,3 Intralesional steroids, topical steroids, topical capsaicin, oral pentoxifylline, and venous surgical intervention have been used as well.1
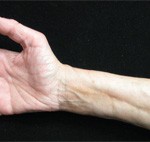
In the patient presented in our case, regular use of compression stockings (30–40 mmHg) as well as potent topical steroid use resulted in resolution of symptoms and softening of the skin in the affected area, along with hair regrowth locally (see Figure 2), which may signal improvement in dermal fibrosis, allowing hair follicle regrowth.
Discussion of Other Choices
B. Morphea: Of the subsets of clinical morphea, this case would be most consistent with an isolated plaque of morphea. Typically in its inflammatory stage, morphea has an erythematous-violaceous border around a sclerotic appearing central area of skin, which, over time, centrally tends to lose its inflammatory component. In the setting of this patient’s venous stasis changes as well as the isolated and characteristic location of the lesion, lipodermatosclerosis is a much more likely diagnosis. Biopsy is able to distinguish these entities, but is not necessary in this case.
C. Cellulitis: LDS is often initially mistaken for an area of early lower extremity cellulitis. A lack of response to antibiotic therapy, lack of systemic symptoms including fever, lack of rapid progression in size and area of involvement, a background of venous stasis disease, and two- to three-month duration make cellulitis much less likely.