Image Credit: NotarYES/shutterstock.com
The Case
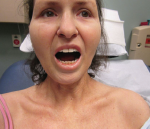
A 68-year-old woman with a past medical history of Charcot-Marie-Tooth presents with thickening of the skin on her trunk and extremities, which she has had for the past seven months (see Figures 1 and 2). Her symptoms first began with swelling of her bilateral upper and lower extremities. She is now having difficulty with writing and extending her legs. She feels well otherwise and has no other systemic complaints. On exam, she has induration of both forearms and the dorsal aspect of her hands and legs, extending from the feet to above the knees. She has flexion contractures of the fingers and knees (see Figure 3). Exam also reveals hyperpigmented, indurated plaques on the back, abdomen and inguinal folds (see Figure 4). Nailfold capillaroscopy is normal. There is no history of Raynaud’s. Laboratory findings include a normocytic anemia, ANA, Lyme titer and negative serum protein electrophoresis. The remainder of an extensive review of symptoms was unremarkable.
What’s Your Diagnosis?
- Systemic sclerosis
- Hypereosinophilic syndrome
- Lipodermatosclerosis
- Eosinophilic fasciitis
- Acrodermatitis chronica atrophicans
Correct Answer
D. Eosinophilic fasciitis
Eosinophilic fasciitis (EF) is a rare connective tissue disorder characterized by edema and induration of the extremities, and rarely the trunk, that can ultimately result in sclerosis and fibrosis, leading to joint contractures and disability. The cutaneous changes may be accompanied by peripheral eosinophilia, hypergammaglobulinemia, elevated acute-phase reactants and, rarely, underlying malignancy. Diagnosis and treatment can be challenging. Cutaneous clues can prevent misdiagnosis, which can lead to unnecessary tests, invasive workups and delays in treatment.
EF is usually a disease of middle-aged or older adults, but there are reports in children & young adults.
The pathogenesis of EF remains unknown; however, interleukin 5 and matrix metalloproteinase 13 have been postulated to play a role.1 Although strenuous exercise and trauma have been described as eliciting factors for EF, this preceding history tends to be reported in only 30–45% of patients.2 Several medications have been suggested as contributing factors in the development of EF, including statins, phenytoin, subcutaneous heparin and therapies for multiple sclerosis.3 Infectious agents, such as borrelia or mycoplasma, have been described as a possible cause in a minority of cases. Hematologic and myelodysplastic disorders, as well as a few reports of solid tumors, have been associated with EF, and treatment of the underlying disorder can result in resolution of the cutaneous findings.
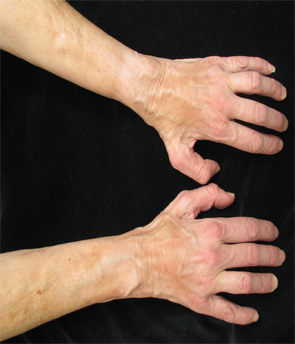
Figure 1.