Prior to the widespread use of bisphosphonates for the management of osteoporosis, multiple myeloma and metastatic cancer to the skeletal system, osteonecrosis of the jawbones was an infrequent condition seen after radiation for oral cancers (osteoradionecrosis) and in chronic odontogenic infections.1
Since the mid-2000s, osteonecrosis of the jawbones has been noted to occur as a result of taking bisphosphonates.2 Bisphosphonates have been shown to not only reduce the incidence of osteoporosis-related fractures, but also skeletal-related events in cancer patients, namely fractures, bone pain, necessity for radiation and
surgery for bone pain and hypercalcemia.3,4 The terms osteonecrosis of the jaw, bisphosphonate osteonecrosis of the jaw, bisphosphonate-related osteonecrosis of the jaws and anti-resorptive osteonecrosis of the jaws (to include denosumab) have now been replaced by the term medication-related osteonecrosis of the jaw (MRONJ), because use of not only anti-resorptive medications, but also anti-angiogenic agents, such as bevacizumab and sunitinib, may also result in this condition.5-7
At this time, anti-resorptive agent-related osteonecrosis by far outnumbers cases caused by other agents.
In addition to their use for osteoporosis and primary and metastatic bone cancer, bisphosphonates are also used for the management of skeletal conditions, such as Paget disease and osteogenesis imperfecta, as well as sporadically for other conditions that cause extensive osteolysis.
Pathogenesis
Bisphosphonates are either non-nitrogen-containing or nitrogen-containing (heterocyclic or alkylamino) agents.9 Alkylamino bisphosphonates (e.g., alendronate and pamidronate) are 100 times more potent that non-nitrogen-containing bisphosphonates (e.g., clodronate and etidronate). Zoledronic acid is the most potent amongst the heterocyclic nitrogen-containing bisphosphonates.
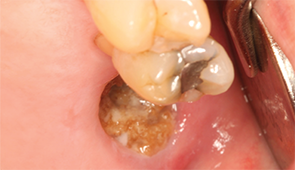
Figure 1: Necrotic
bone in non-healing extraction socket.
Bisphosphonates are potent inhibitors of osteoclast-mediated bone resorption. They bind to hydroxyapatite, and approximately 60% of the absorbed oral dose is deposited into the bone.9 During bone remodeling, bisphosphonates are released from the hydroxyapatite and taken up by osteoclasts. Non-nitrogen-containing bisphosphonates are converted to adenosine triphosphate analogs and accumulate in the osteoclast, leading to markedly reduced bone resorption and bone turnover.10
Nitrogen-containing bisphosphonates inhibit farnesyl pyrophosphate synthase through the mevalonate pathway, also leading to osteoclast apoptosis.11
The theory that emphasizes reduced bone turnover as the primary etiopathogenetic event is also sometimes termed the Inside-Out theory. The theory is that bone necrosis initiates within the bone (whether or not exacerbated by micro-trauma) and spreads outward, to be ultimately exposed. This is well illustrated in an animal study by Allen and Burr.12 In addition, bisphosphonates inhibit the angiogenic response induced by the vascular endothelial growth factor (VEGF).13