vrx/shutterstock.com
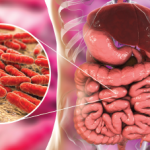
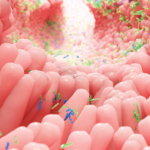
New research reinforces the hypothesis that the gut microbiome triggers mucosal and systemic immune responses in patients with rheumatoid arthritis. The research, published in Arthritis & Rheumatology May 2017, found that subgroups of patients with RA have differential immunoglobulin G (IgG) or IgA immune reactivity with Prevotella copri, an intestinal microbe that appears to be specific for the disease.1 These observations “provide evidence of the immune relevance of P copri in the pathogenesis of RA,” the investigators say.
Lead author Annalisa Pianta, PhD, at Massachusetts General Hospital and Harvard Medical School, says the research she and her colleagues conducted found that about half of patients with RA have T and B cell responses to P copri. Their responses were either IgA antibody responses to P copri, “suggestive of a mucosal immune response, or IgG antibodies to the organism, suggestive of a systemic immune response,” Dr. Pianta says.
For the study, the investigators developed an unbiased, discovery-based approach to identify novel, immunogenic T cell epitopes in patients with chronic inflammatory arthritis. They obtained synovial tissue, synovial fluid mononuclear cells or peripheral blood mononuclear cells from five patients to use for isolation of HLA-DR-presented peptides.
Implicated peptides and their source proteins were tested for immunoreactivity in a larger number of patients, which included a cohort with new-onset RA from whom clinical information, peripheral blood mononuclear cells, serum samples and, for some, synovial fluid samples were available. For comparison, researchers obtained serum samples and peripheral blood mononuclear cells from patients with Lyme arthritis. They also used serum samples from patients with other types of arthritis or connective tissue disease as well as from healthy control subjects.

Dr. Pianta
P copri DNA was detected in synovial fluid in three of the five patients tested who were positive for IgG P copri antibodies, Dr. Pianta says. “These responses appeared to be specific for RA and were not found in patients with other rheumatic diseases or in healthy control subjects.” The frequencies of P copri antibody responses were similar in patients with new-onset RA and those with chronic RA, “suggesting that, once initiated, these antibody responses may persist for years,” the researchers reported.
Previous research by Scher et al in 2013 reported an overexpansion of P copri in patients with new-onset untreated RA compared with patients with chronic RA or psoriatic arthritis or healthy controls.2 According to Dr. Pianta, this “implies that gut dysbiosis may lead to gut inflammation or vice versa, but the reasons for dysbiosis are not yet known. Since P copri overexpansion seems to occur primarily in patients with RA, this likely explains why antibody responses to P copri were rarely found in patients with other rheumatic diseases,” Dr. Pianta says.