Look inside the oral cavity of a patient for answers that go beyond what we perceive as the dentist’s domain. So goes the thinking of medical professionals interested in how oral health and bacteria-driven disease, such as periodontitis, may be linked to rheumatic disease, especially rheumatoid arthritis (RA).
Look inside the oral cavity of a patient for answers that go beyond what we perceive as the dentist’s domain. So goes the thinking of medical professionals interested in how oral health and bacteria-driven disease, such as periodontitis, may be linked to rheumatic disease, especially rheumatoid arthritis (RA).
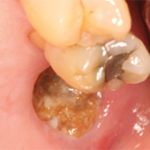
Bad bacteria that live in the mouth can cause gingivitis and periodontitis, which pose risk to a patient’s oral health and could lead to loss of bone and teeth. Plaque, a destructive film of bacteria found on and in between teeth, contributes to these different stages of disease that leave the gums swollen and inflamed, but what happens when those bacteria enter the bloodstream and move through the body?
Periodontitis & RA
For several years, researchers have investigated associations between RA and gum disease, also known as periodontitis. Research conducted at Johns Hopkins Arthritis Center by Clifton Bingham III, MD, associate professor of medicine and director of the center, and research fellow Malini Moni, BDS, MS, found that out of 100 RA patients studied, 70% had gum disease and 30% had severe gum disease, which was much higher than among the 40 healthy participants (35% of whom had gum disease and 5% of whom had serious gum disease).1
Chronic inflammation is common to both RA and gum disease, and some theories explore the possibility that infection of the mouth may travel into the bloodstream and trigger inflammation and disease elsewhere in the body. But whether one disease causes the other is not clear.

Dr. Scher
“What’s been known for several decades now is this idea that periodontal disease at a population level is significantly correlated with rheumatoid arthritis and rheumatoid arthritis activity,” says Jose U. Scher, MD, a New York University School of Medicine assistant professor of rheumatology and director of the Arthritis Clinic and Microbiome Center for Rheumatology and Autoimmunity at NYU Langone Medical Center.
Exactly what causes RA is still unknown, and whether periodontal disease is a triggering factor remains to be seen, explains Dr. Scher to The Rheumatologist. Perhaps more important, he notes, is the question of whether both could be treated in a concomitant fashion.
“If you could treat rheumatoid [arthritis] patients with periodontal disease with both rheumatoid [arthritis] medications and periodontal nonsurgical approaches, then that would be the ultimate answer,” says Dr. Scher. “It has not been done yet.”

Ms. Slusher