ACR Convergence 2021—Scleroderma represents a challenge for many rheumatologists: The disease is rare, the onset of symptoms can be subtle, and the condition has few effective treatments. In the Review Course held during ACR Convergence 2021, Laura Hummers, MD, MSc, clinical director of the Division of Rheumatology, Johns Hopkins, and co-director of the Johns Hopkins Scleroderma Center, Baltimore, provided an update on the extra-pulmonary manifestations of scleroderma and the best ways to approach management of these issues.
Limited vs. Diffuse Cutaneous
Dr. Hummers began her talk with a discussion of limited cutaneous vs. diffuse cutaneous systemic sclerosis. In patients with limited cutaneous disease, Raynaud’s phenomenon is often the first sign of disease and can precede other signs and symptoms by a number of years.
Patients with limited cutaneous disease tend to have more severe vascular issues, such as pulmonary arterial hypertension and digital ulcers, compared with patients with diffuse cutaneous disease. Although autoantibodies directed against centromere are the most common finding in patients with limited cutaneous systemic sclerosis, other autoantibodies that may be present in these patients include anti-Th/To and anti-U1 RNP antibodies; anti-U3 RNP antibody (i.e., fibrillarin), anti-Pm-Scl antibody, and anti-Scl-70 antibody (i.e., topoisomerase).
The vast majority of patients with limited cutaneous disease don’t need therapy directed at skin involvement; this condition tends to be confined to sclerodactyly and does not require systemic immunosuppression.
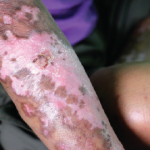
For patients with diffuse cutaneous systemic sclerosis, the skin involvement tends to be inflammatory and patients often recall the day they noted onset of puffy hands and feet. Unlike limited cutaneous disease, Raynaud’s phenomenon in patients with diffuse cutaneous disease can coincide with, rather than precede, the onset of skin disease, and cutaneous involvement can sometimes predate the appearance of Raynaud’s. The two autoantibodies typically seen in diffuse cutaneous disease are anti-Scl-70 antibody and anti-RNA polymerase III antibody.
Although patients with autoantibodies to Scl-70 tend to have a variable course of skin involvement, patients with antibodies directed against RNA polymerase III usually have a fairly consistent, progressive course. Thus, if a patient is seen when skin involvement is still considered limited (i.e., distal to the elbows and knees) but has antibodies against RNA polymerase III and is showing rapid worsening of skin involvement, it would be reasonable to consider early initiation of systemic treatment.
Dr. Hummers noted that testing for antibodies to RNA polymerase III is important because, in addition to predicting the clinical course of skin disease, these antibodies are associated with an increased risk of scleroderma renal crisis and of concurrent malignancy.
An unmet need still exists for therapies that may be more effective than methotrexate, mycophenolate mofetil, intravenous immunoglobulin & cyclophosphamide in treating skin disease in scleroderma.
Treatment Options
With respect to treatment options, Dr. Hummers’ clinical practice is to evaluate the domains involved (e.g., skin, interstitial lung disease, myositis, arthritis) and treat accordingly. She noted that, although nintedanib and tocilizumab are now approved by the U.S. Food & Drug Administration for the treatment of scleroderma-associated interstitial lung disease, neither agent has shown benefit in improving cutaneous involvement.
Lenabasum, an oral, non-immunosuppressive preferential cannabinoid-2 agonist, was tested in the RESOLVE-1 trial after showing promise in a phase 2 study. In a 52-week randomized clinical trial, Spiera et al. enrolled 365 patients with early diffuse cutaneous systemic sclerosis (with 84% of patients on background therapy) and randomized them to 5 mg or 20 mg of lenabasum twice daily or placebo.
The authors found no difference in the primary or secondary key endpoints between the study medication (lenabasum 20 mg twice daily) and placebo.1 These findings indicate that an unmet need still exists for therapies that may be more effective than methotrexate, mycophenolate mofetil, intravenous immunoglobulin (IVIG) and cyclophosphamide in treating skin disease in scleroderma.
Raynaud’s Phenomenon
Dr. Hummers next discussed Raynaud’s phenomenon, including the features that make secondary causes more likely, such as onset at older age, abnormal nailfold capillaries, positivity for scleroderma-associated autoantibodies, etc., and the importance of screening for pulmonary hypertension with annual echocardiogram and pulmonary function testing in these patients at higher risk.
Non-pharmacologic treatment for Raynaud’s includes keeping hands, feet and the central body warm; avoiding stress and quitting smoking; and avoiding common precipitants of the condition, such as caffeine and beta blockers. For patients with persistent symptoms, sustained-release dihydropyridine calcium channel blockers are indicated; if low baseline blood pressure is present, selective serotonin reuptake inhibitors, pentoxifylline and statins may be potential options. For severe acute or recurrent digital ischemia, prostacyclin analogs or botulinum toxin injection can be of help.
Renal Crisis
Dr. Hummers concluded the lecture discussing two important topics: scleroderma renal crisis and gastrointestinal manifestations of scleroderma. Risk factors for renal crisis include diffuse, rapidly progressive cutaneous disease, African American race, positivity for antibodies to RNA polymerase III, and use of corticosteroids (particularly >15 mg of prednisone per day). With only a 65% five-year survival in patients who suffer this complication, screening for the condition with daily blood pressure measurements is critical, and any new onset of hypertension (particularly blood pressure >140/90 lasting for more than 24 hours) should prompt workup and likely hospital admission.
Gastrointestinal Disease
Up to 70% of patients with scleroderma report taking medications for gastrointestinal (GI) symptoms.2 Possible risk factors for severe GI disease include the presence of anti-U3 RNP, anti-U11/U12 RNP and anti–muscarinic-3 receptor (M3R) antibodies, and African American race.2 Gastroesophageal reflux disease, gastroparesis, dysmotility and gastric antral vascular ectasia (GAVE) are among the forms of gastrointestinal involvement that patients may experience and coordination of care with a gastroenterologist is often required.
In Sum
Through this thoughtful and accessible presentation, Dr. Hummers shed light on important topics related to the care of patients with scleroderma.
Jason Liebowitz, MD, completed his fellowship in rheumatology at Johns Hopkins University, Baltimore, where he also earned his medical degree. He is currently in practice with Skylands Medical Group, N.J.
References
- SpieraR, Kuwana M, Khanna D, et al. OP0171 Phase 3 trial of lenabasum, a CB2 agonist, for the treatment of diffuse cutaneous systemic sclerosis. Ann Rheum Dis. 2021;80 (Suppl 1):102–103.
- Miller JB, Gandhi N, Clarke J, McMahan Z. Gastrointestinal involvement in systemic sclerosis: An update. J Clin Rheumatol. 2018;24(6):328–337.