 Giant cell arteritis (GCA), a large- and medium-vessel vasculitis, mainly involves the thoracic aorta and its branches. Few studies have evaluated the predictive factors for increased mortality in GCA patients. Recent findings of an Italian study of patients with incident temporal artery biopsy-proven GCA suggest large-vessel involvement at GCA diagnosis independently contributes to increased mortality. Also, the presence of polymyalgia rheumatica and isolated adventitial involvement or vasa vasorum vasculitis were associated with reduced mortality.1
Giant cell arteritis (GCA), a large- and medium-vessel vasculitis, mainly involves the thoracic aorta and its branches. Few studies have evaluated the predictive factors for increased mortality in GCA patients. Recent findings of an Italian study of patients with incident temporal artery biopsy-proven GCA suggest large-vessel involvement at GCA diagnosis independently contributes to increased mortality. Also, the presence of polymyalgia rheumatica and isolated adventitial involvement or vasa vasorum vasculitis were associated with reduced mortality.1
According to histopathological patterns of the study patients, the differences in survival present new perspectives in predicting disease severity and mortality risk, says Pierluigi Macchioni, MD, a rheumatologist in the Department of Rheumatology, Azienda USL-IRCCS di Reggio Emilia, Italy, and an investigator in the study.
Previous studies evaluating mortality associated with GCA have concluded that mortality risk may be increased in some patients and may vary over time.2,3 Research has also demonstrated the value of imaging for better recognition and diagnosis of large-vessel involvement in GCA.4 However, none have considered temporal artery biopsy results or the presence of large-vessel involvement at disease presentation, Dr. Macchioni notes.
“The presence of these factors are more relevant for survival than cardiovascular risk factors,” he says.
Key Findings
The retrospective study analyzed data from 281 patients with incident temporal artery biopsy-proven GCA from the Reggio Emilia province of Northern Italy. Patients were diagnosed over a 26-year period, from 1986–2012. Investigators used multivariate analysis to analyze clinical, imaging and laboratory findings at diagnosis; pathological patterns of temporal artery biopsy; corticosteroid treatment and therapeutic outcomes; and traditional cardiovascular risk factors for predictive survival, including hypertension, hypercholesterolemia, hypertriglyceridemia, diabetes and smoking.
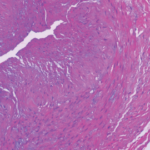
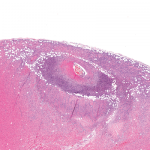
At the time of disease diagnosis, traditional cardiovascular risk factors and past history of cerebrovascular accidents and ischemic heart disease were not associated with a reduced survival in these patients. On histological examination of the temporal artery, patients with localized inflammation at only the adventitial layer were found to have significantly increased survival, which may represent a subset of patients with less severe disease and reduced mortality. Additionally, long-term GCA remission in this study was associated with reduced mortality, suggesting the efficacy of controlling inflammation.
Clinical Implications
Dr. Macchioni points to several implications for clinical practice that can be understood from identifying these survival predictors:
- Determining the presence of large-vessel involvement at disease presentation using imaging, such as ultrasound or positron-emission tomography (PET) scan of the large vessels;
- Defining the contemporary presence of polymyalgia rheumatica by asking the patient for signs and symptoms of this diseases and looking for typical alterations in shoulders or hips on ultrasound; and
- Identifying the relevance of temporal artery biopsy, because patients with inflammation localized at only the adventitial layer have the best possibility of survival.
Two follow-up studies to this research are currently in progress. One is evaluating microRNA and cytokines and other inflammatory factors in biopsy specimens and blood of GCA patients as prognostic factors of survival and disease flares. The second study is investigating the evolution during follow-up of the large-vessel lesions found by PET scans and/or ultrasound as prognostic factors of survival.