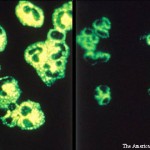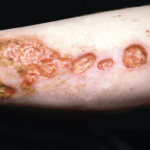
Historically, granulomatosis with polyangiitis (Wegener’s granulomatosis; GPA) and microscopic polyangiitis (MPA) were usually relentlessly progressive and often fatal illnesses. Immunosuppressive therapy has converted these diseases, which are often referred to collectively as antineutrophil cytoplasmic antibody (ANCA)–associated vasculitis (AAV), into chronic conditions in which remission is usually achieved, but subsequent relapse is common and yet unpredictable in its timing.
Because treatment with glucocorticoids combined with either cyclophosphamide, rituximab, or methotrexate leads to remission in the great majority of patients, identifying optimal strategies to maintain remission with minimal toxicity has become nearly as important a research topic as refining remission-induction regimens, and one that is highly relevant to clinical practice. Maintenance regimens have been compared in recent randomized clinical trials, but many unanswered questions remain. I will summarize these trials, highlight the important remaining questions, review the observational data that can be used to address these questions while we await trial results, and conclude with examples of how I use the available data to guide management of different types of patients.
Effects of Remission-Induction Regimen and Other Factors on Relapse Rates
Randomized trials are particularly important for answering questions about remission-maintenance in AAV for three reasons. First, subsets of AAV defined by ANCA specificity have different relapse rates. Multiple studies have indicated that patients with antibodies to myeloperoxidase (MPO) have relapse rates about 50% lower than patients with antibodies to proteinase-3 (PR3).1,2 Second, and not surprisingly, patients who have relapsed in the past are more likely to relapse again. Thus, comparing relapse rates between trials with different percentages of anti–MPO-positive patients and/or of newly diagnosed patients is problematic.
Third, different induction regimens have been found to be associated with different relapse rates in the setting of randomized trials in which induction regimens differed but maintenance regimens were the same in all groups. This finding has been made even in the setting in which the initial effectiveness of the induction regimens appeared to be the same. Thus, initial use of methotrexate or intravenous cyclophosphamide has been associated with higher relapse rates than oral cyclophosphamide.1,3
A recent trial showing that rituximab was equivalent to oral cyclophosphamide for remission-induction (RAVE) may be more difficult to interpret with regard to relapse rates, since the cyclophosphamide group received azathioprine to complete 18 months of standard treatment, whereas the rituximab group did not receive any additional treatment, and it is presumed that the drug’s effect (based on return of circulating B cells) had worn off in nearly all patients by Month 18.4 The key 18-month clinical outcome of RAVE is not yet published but was presented at the 2011 ACR annual meeting: Relapse rates were the same in patients who received one course of rituximab and in patients who continued to receive azathioprine after cyclophosphamide.5 Thus, as of Month 18, either induction therapy with rituximab led to lower subsequent relapse rates than induction with oral cyclophosphamide, or maintenance therapy with azathioprine had little or no benefit.
Key Points
- Both the remission-induction regimen and ANCA specificity (PR3 or MPO) influence future relapse rates.
- Randomized trials of maintenance regimens indicate that azathioprine and methotrexate are equivalent, and superior to mycophenolate.
- Rituximab appears to be highly effective as maintenance therapy, but reports are anecdotal and mostly unpublished.
- Uncertainties that should be addressed in future trials include comparison of rituximab to azathioprine for maintenance, comparison of different durations of maintenance, and measurement of the effect of low-dose prednisone on relapse rates.
The RAVE trial design therefore serves as a reminder that it is worth considering the evidence that maintenance treatment is effective at all. The data addressing this question are limited and mostly observational but, I think, still convincing. First, early in the era of successful treatment of GPA with cyclophosphamide, it was noted that patients treated for only a few months were very likely to relapse, which led to the recommendation to continue cyclophosphamide for a year after achievement of remission.6 Second, addition of sulfamethoxizole-trimethoprim to a variety of other medications during remission was associated with reduced relapse rates in a randomized trial.7 Third, comparison of two groups of patients separated in time but otherwise managed very similarly at one center indicated that relapse rates were much lower in patients given methotrexate rather than sulfamethoxizole-trimethoprim after remission induction.8
Trials: Immune-Suppressive Drugs as Maintenance Therapy
On that background, the current standard of care for maintenance therapy has been established by randomized trials. Most importantly, in a trial now known as CYCAZAREM, the demonstration that switching from cyclophosphamide to azathioprine (2 mg/kg daily) at the time of achieving remission (between Months 3 and 6) resulted in the same relapse rate as continuing cyclophosphamide changed standard of care.9 Incidentally, the fact that this trial was 18 months long has contributed to the widespread practice and recommendation to discontinue maintenance therapy at 18 months in patients who have remained in remission—a strategy that has never been compared to continuing therapy.