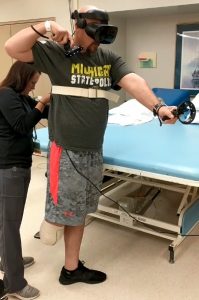
ATLANTA—What if efforts to regain daily function after an illness or injury felt less like a burden and more like … fun? It’s possible, with virtual reality, said Robert Ferguson, MHS, OTRL, stroke rehabilitation program manager at the University of Michigan, Ann Arbor, in a session of the 2019 ACR/ARP Annual Meeting.
Interest in virtual reality to promote rehabilitation is spreading, Mr. Ferguson said, but he pointed to details that are often overlooked and that, if missed, could lead clinicians and therapists astray.
Still, his firsthand experience with the possible results is persuasive that virtual reality can have big effects. Engaging with a simple screen on which patients play a game that involves a motor function needing improvement can help the patient forget—or least not mind as much—that they’re making an effort, he said.
Interest in virtual reality to promote rehabilitation is spreading.
Big Effects of Virtual Reality Rehab
“You can be so involved in that virtual context that you enter that concept of ‘flow,’ and you just lose track of time and effort,” Mr. Ferguson stated.
One patient with a below-knee amputation played a game in which he had to defend a castle against minions. “He was much more aware of what his intact limb was doing, and how it was reacting for balance,” Mr. Ferguson said. He got through 1,200 arm-movement repetitions in 45 minutes with improved active-balance reactions that he wasn’t demonstrating before the immersive virtual activity—great preparation in advance of his occupational therapy.
Another man understood that he was working, but didn’t seem to mind, saying, “It’s the hardest therapy I’ve ever done, but it’s the funnest,” giving Mr. Ferguson the best of both worlds: maximal effort and maximal patient satisfaction.
Another patient, recovering after a stroke, played a game involving steering a boat with a joystick, requiring pushing and contraction of the shoulder and arm: “[The] feedback is that if the boat’s not moving, they’re not pushing. I don’t have to say a word,” said Mr. Ferguson.
Benefits for Rheumatology Patients
Some evidence suggests benefits from the judicious use of immersive virtual reality with patients with rheumatic diagnoses.1 People tend to have a lower perception of effort compared with actual exertion and lower reports of pain with longer time to exhaustion. But patients should be monitored for appropriate responses consistent with their treatment plan and activity recommendations, Mr. Ferguson said.
Interest in using virtual reality as a medical tool has led to some misconceptions, Mr. Ferguson said. First, one’s very definition of virtual reality could be wrong. It doesn’t necessarily mean completely stepping into a digital world with no sign of the real world anywhere around you. Virtual reality can be non-immersive, such as a game played on a tablet or smartphone.2
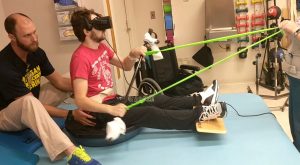
Michael Blackstock, MS, OTRL, works with a patient using a virtual reality headset while seated on an inverted Bosu ball.
Then there’s mixed reality, a combination of the real world and virtual elements, as well as immersive virtual environments, in which displays worn on the head, with or without tracking of body movements as you move through that virtual world.
Most of the research done on virtual reality actually involves a screen and not a fully immersive environment.3
“When you’re reading an article that says ‘virtual reality,’ you have to look at [it],” Mr. Ferguson said. “Is it immersive or non-immersive? Is it mixed reality? And if it is, what kind of mixed reality? All of these things you have to think about because we interact with it very differently based on the context that it gives you.”
“More and more people are using this in the clinic,” he said. “But they’re reading that research, and they’re applying it wrong, or they’re not reading the research at all.”
Virtual Reality as Adjunct Treatment
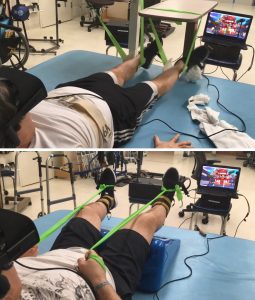
Engaging with a screen to play a game that involves a motor function needing improvement can help the patient forget—or least not mind as much—that they’re making an effort.
Crucially, he said, virtual reality is typically used only in support of other forms of occupational or physical therapy.
“We need to connect it to a goal,” he said. “The research tells us that the virtual reality is not the treatment. It’s an adjunct treatment to what you’re doing. What’s important is the goal and strategies that you’re using to achieve the goal.”
Mr. Ferguson described virtual reality—and particularly the immersive version—as context, but a powerful one.
“The great thing—and the thing that gives you so much therapeutic power in this context—is it doesn’t have to obey the laws of physics. You can do some crazy things in the virtual context that you can’t do in the real world. And it opens up and changes the way we perceive things and think about things,” said Mr. Ferguson.
Real Results
Virtual though the experience may be, the results are very real.
“My favorite day is when a patient comes in to a computer therapy lab session and says, ‘Guess what I was able to do?’ because of what they did in here,” he said. “It gave them that extra capacity to brush their hair‚ something that’s simple that we take for granted every day—brushing your hair or your teeth or feeding yourself or putting your shirt on. And when they say, ‘I finally did it,’ that, to me, makes a good day.”
Thomas R. Collins is a freelance writer living in South Florida.
References
- Matamala-Gomez M, Donegan T, Bottiroli S, et al. Immersive virtual reality and virtual embodiment for pain relief. Front Hum Neurosci. 2019;13:279.
- Milgram P, Takemura H, Utsumi A, Kishino F. Augmented reality: A class of displays on the reality-virtuality continuum. SPIE. 1994;2351:282–292.
- Aminov A, Rogers JM, Middleton S, et al. What do randomized controlled trials say about virtual rehabilitation in stroke? A systematic literature review and meta-analysis of upper-limb and cognitive outcomes. J Neuroeng Rehabil. 2018 Mar 27;15(1):29.