molekuul_be/shutterstock.com
A task force of the American Society for Bone and Mineral Research (ASBMR) has released new recommendations delineating the potential benefits and risks of prolonged therapy with oral and IV bisphosphonate therapy and providing guidance on duration of bisphosphonate therapy for postmenopausal osteoporosis.1
The task force makes clear that data and clinical experience on which to base the recommendations are limited and that the approach for long-term bisphosphonate therapy use is based on evidence in mostly white postmenopausal women. Task force co-chairs Robert A. Adler, MD, and Ghada El-Hajj Fuleihan, MD, told The Rheumatologist, “Despite all the research in osteoporosis, our knowledge base for long-term management of this common chronic disorder is very limited.”
Dr. Adler is chief of endocrinology and metabolism at McGuire Veterans Affairs Medical Center and professor of internal medicine at Virginia Commonwealth University School of Medicine in Richmond; Dr. El-Hajj Fuleihan is professor of medicine and founding director of the Calcium Metabolism and Osteoporosis Program at the American University of Beirut, Lebanon. The task force comprised experts in osteoporosis management, epidemiology, endocrinology, geriatrics and drug surveillance, a bone scientist not in the osteoporosis field and an ethicist.
Chief among the recommendations given in the report, Managing Osteoporosis in Patients on Long-Term Bisphosphonate Treatment: Report of a Task Force of the American Society for Bone and Mineral Research, is that a patient’s risk should be reassessed after five years of oral bisphosphonate therapy or three years of intravenous (IV) zoledronic acid therapy. Women at high risk, such as older women, those with a low hip T-score (less than or equal to -2.5) or high fracture risk score, those with a previous hip or spine fracture, or those who sustain a major osteoporotic fracture while on therapy, can be considered for treatment for up to 10 years of oral therapy or six years of IV therapy, with periodic evaluation, according to the recommendations.

Dr. Bolster
“This recommendation reinforces the idea that the purpose of therapy is to reduce fracture, while also reflecting the lack of long-term fracture efficacy using these drugs and the long-term retention in bone,” Drs. Adler and El-Hajj Fuleihan told The Rheumatologist.
“Based on a benefit/risk ratio approach, the Task Force recommends treatment for the person at high risk for fracture at baseline and continued treatment for up to 10 years in those who are still at such risk three to five years after initiation of therapy. The tools to assess fracture risk are limited, and periodic assessment is based on clinical information, physical examination and DXA [dual-energy X-ray absorptiometry] measurements to stratify risks,” they say.
The task force also recommends that women who are not at high risk of fracture after three to five years of bisphosphonate treatment be considered for a two- to three-year drug holiday.
Marcy B. Bolster, MD, associate professor of medicine, Harvard Medical School, in the Division of Rheumatology, Allergy and Immunology at Massachusetts General Hospital, Boston, says the recommendations “will help ensure that drug holidays are considered in all patients treated with bisphosphonates and that there are more specific reasons, or risk factors, to inform the decision to continue oral therapy for longer than five years and IV bisphosphonate therapy for longer than three years.
“It is clear from the recommendations that decisions for duration of therapy should be individualized and should include informed decision making shared between the healthcare provider and the patient,” she says.
Efficacy Data
Evidence supporting bisphosphonate therapy beyond five years is from two randomized, double-blind discontinuation trials: the FLEX study with oral alendronate and the HORIZON extension study with IV zoledronic acid. A five-year follow-up of patients in the FLEX study showed that those who continued oral alendronate therapy after four to five years of therapy had significantly less bone loss at all skeletal sites and fewer clinical vertebral fractures than those who had switched to placebo. In the HORIZON study extension, postmenopausal women who had already received three annual IV infusions of zoledronic acid and then continued therapy for another three years had fewer morphometric spine fractures than those who switched to placebo therapy.
Treatment efficacy—larger increases in bone mineral density and lower rates of fracture—is dependent on patient adherence to therapy, the task force said. Less than 50% of patients who start oral therapy continue for more than one year due to cost, co-morbidities, side effects, concern about side effects, inconvenience, use of multiple medicines and poor understanding of the benefits. About 30% of patients who receive an initial IV infusion return for the second infusion a year later.
Assessing Risk & Benefit
The report includes a discussion of the potential risks of bisphosphonate therapies. One of the potential harms of prolonged bisphosphonate therapy has been the risk for atypical femoral fractures. For the first three to five years of bisphosphonate therapy, the risk–benefit ratio clearly favors treatment for those at significant risk of osteoporotic fracture, with an estimate of averting 162 fractures of the spine, hip or forearm per one atypical femoral fracture caused, Drs. Adler and El-Hajj Fuleihan say. “In the five- to 10-year period, there is sustained vertebral fracture risk reduction for those who remain at higher fracture risk, but a similar estimate for the risk–benefit ratio is difficult to define due to insufficient data. It is probably lower due to the evidence that atypical femoral fractures increase with duration of bisphosphonate use,” they say. Even so, atypical femoral fractures are uncommon and occur in less than 0.2% of patients on eight to 10 years of bisphosphonate therapy.
“We are hopeful that in the future we can determine which patients are more likely to suffer them,” they added.
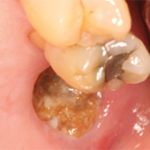
Another safety concern with bisphosphonate therapy has been osteonecrosis of the jaw. Current estimates of the incidence of osteonecrosis of the jaw range from about 1/10,000 to 1/100,000 patient treatment-years. Factors that can potentially increase this risk for patients treated with bisphosphonates include poor oral hygiene, smoking, diabetes, concomitant glucocorticoids and/or chemotherapy use, and invasive dental procedures. The report says that there appears to be a trend for increased risk of osteonecrosis of the jaw with duration of bisphosphonate use, but the quality of the evidence for such an association is poor. The task force recommends that risk factors for osteonecrosis of the jaw be included in the periodic assessment of benefits and risk of bisphosphonate therapy.
“For most patients treated for osteoporosis, the bisphosphonate-associated benefit of reduced fracture risk beyond five years, albeit with evidence for vertebral fracture only, is greater than the risk of developing either osteonecrosis of the jaw or an atypical femoral fracture,” the report states.
Dr. Bolster says the risks and benefits of bisphosphonate therapy should always be considered, with the risk of therapy at the initiation of treatment different from the risks to consider after three to five years of treatment. “Fracture risk reduction is the tremendous benefit attained with initiation of treatment, and this is weighed against the potential risk of therapy, including gastrointestinal effects, flu-like symptoms, bone pain.”
A patient’s risk should be reassessed after five years of oral bisphosphonate therapy or three years of intravenous (IV) zoledronic acid therapy.
Risk stratification is warranted at the time more prolonged therapy is being considered, she says, with a consideration of the patient’s hip T-score, prior history of hip or spine fracture, fracture while on therapy (e.g., hip, spine, humerus, forearm), age, medication use (such as aromatase inhibitors, glucocorticoids) or a new diagnosis of a condition associated with a secondary cause of bone loss.
Drs. Adler and El-Hajj Fuleihan note that risk stratification is based on DXA scans and various calculators, such as FRAX (Fracture Risk Assessment Tool), that incorporate clinical factors, such as age and personal history of fractures. It’s also important to have the patient on adequate dietary calcium, keep their 25-hydroxyvitamin D level of at least 30 ng/mL, maintain muscle strength, avoid falls, improve home safety and take medications correctly and regularly, they say.
Other Populations
The report additionally considers what is known about use of long-term bisphosphonate therapy in patients taking continuous oral glucocorticoids. Spine fractures occur with greater frequency in older patients on higher doses of glucocorticoids, regardless of their bone mineral density. The report suggests that for women who require continued bone-protective therapy and who have received bisphosphonates for more than five years, switching to teriparatide may be considered. Men older than age 50 who are treated with long-term glucocorticoids greater than 5 mg/d are also at increased risk of fracture and may benefit from continuation of bisphosphonate therapy.
Although little evidence is available for men, the approach advocated by the task force can be considered generally applicable to older men, the task force says. It is assumed that men on long-term bisphosphonate therapy have safety issues similar to postmenopausal women, with no greater risk identified in men. The task force indicates it is reasonable to continue treatment in men on long-term bisphosphonate therapy who have a history of hip, spine or multiple other osteoporotic fractures or major osteoporotic fracture while on therapy. A drug holiday of two or three years is reasonable for men who are not considered at high risk because of age or other risk factors, such as androgen-deprivation therapy for prostate cancer. Men at higher risk could continue treatment and be reassessed for a drug holiday in two to three years, according to the report.
Clinical Judgment
No trials have evaluated the antifracture efficacy of switching therapies after three to five years of bisphosphonate treatment, none have extended beyond 10 years, and none have assessed the utility of reinitiation of treatment after a drug holiday, the report states. Because of this lack of data, the task force strongly recommends a tailored approach that includes assessment of each patient’s individual risk profile, shared decision making with the patient and careful follow-up. “The clinician caring for the patient with the chronic disorder of osteoporosis will need to use the art in addition to the science of medicine,” with the approach created by the task force being one tool that will help in decision making, the report says.
Several cases included in the report’s appendix illustrate the challenges of clinical care for patients with osteoporosis. Drs. Adler and El-Hajj Fuleihan say that a clinician has to periodically assess the patient’s risks in view of their evolving profile and the accumulating new evidence: Are there new risks? Does the patient fall? Is the patient taking medications properly? What are new pharmacologic and nonpharmacologic interventions that can be used to decrease fracture risk in a given patient?
“The clinician will complement the evidence derived from scientific studies with the art of practicing medicine to make a reasonable and individualized treatment plan, engaging the patient in the process,” they say.
Kathy L. Holliman, MEd, is a medical writer based in Beverly, Mass.
Reference
- Adler RA, El-Hajj Fuleihan G, Bauer DC, et al. Managing osteoporosis in patients on long-term bisphosphonate treatment: Report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res. 2016;31(1):16–35.